By Virginia Miraldi, BA, Arun D Singh, MD, and Bennie H. Jeng, MD
Edited Thomas A. Oetting, MD
This article is from March 2007 and may contain outdated material.
Eleanor Green* looked once again in her bathroom mirror as she got ready for her early morning kickboxing class. She had noticed a bluish gray color in the whites of her eyes for the past two months. At 79 years of age, she had initially dismissed the change as a normal part of aging until she observed that her 105-year-old mother had no such changes. She decided to ask her ophthalmologist about the color change at her next visit.
Case Presentation
Ms. Green initially presented to her general ophthalmologist with the bluish gray discoloration of her sclera. She was then referred to our ophthalmic oncology service to be evaluated for ocular melanosis. Her past ocular history was significant for bilateral cataract surgery, ptosis repair and dry eye. Her past medical history also was significant for hypertension, multiple cutaneous cancers (including squamous cell carcinoma, basal cell carcinoma and melanoma), rosacea, hypothyroidism and arthritis. Her medications included irbesartan, amlodipine, warfarin, minocycline, propoxyphene/acetaminophen, levothyroxine, atorvastatin, calcium, and vitamins D and E.
What we saw. On examination, her uncorrected visual acuity was 20/40 in her right eye and 20/20 in her left. Her pupillary examination, extraocular movements and intraocular pressures were all within normal limits. We observed that she had bluish gray scleral pigmentation bilaterally (Figs. 1 and 2), with mild episcleral injection bilaterally. The rest of her slit-lamp examination and her funduscopic examination were within normal limits.
What's Your Diagnosis?
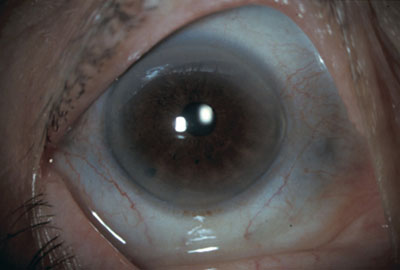 |
| Diffuse illumination view of right eye, demonstrating bluish discoloration of nasal and temporal sclera. |
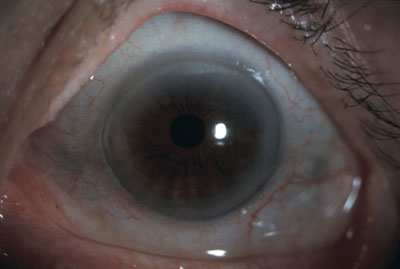 |
| Diffuse illumination view of left eye, demonstrating bluish discoloration of nasal and temporal sclera. |
The Differential Diagnosis
The differential diagnosis included three types of conditions—localized, systemic and toxic.
Localized conditions were considered:
- Primary acquired melanosis (PAM) usually appears as a golden brown, flat, patchy area with an irregular margin. These lesions are usually unilateral with onset in middle age. They can progress to malignant melanoma if cellular atypia is present.
- Conjunctival melanoma typically appears as a pigmented, raised, nodular lesion that may involve any portion of the conjunctiva. It may arise de novo, from a pre-existing nevus or from PAM with atypia.
- A conjunctival nevus is a small, pigmented lesion. Unlike melanoma or PAM, these lesions rarely involve the palpebral conjunctiva.
- Oculodermal melanocytosis is a congenital disorder resulting from defective neural crest cell-derived melanocyte migration. These lesions typically appear on the facial skin and globe. The episclera often has bluish, fusiform spots underlying normal conjunctiva. These lesions are usually unilateral, but occasionally are bilateral. These patients have an increased risk for uveal melanoma and glaucoma.This disorder tends to be more prevalent in the Asian population.
Systemic conditions were considered: Pigmentation of the skin and eyes can be secondary to systemic conditions.
- Alkaptonuria is an autosomal recessive amino acid disorder that involves a defective homogentisic acid oxidase, an enzyme that is critical in the metabolism of phenylalanine and tyrosine. This defect leads to the accumulation of homogentisic acid that polymerizes to form a pigment that is deposited in connective tissue throughout the body. Alkaptonuria consists of the triad of homogentisic aciduria, ochronosis and arthritis, although renal and urinary calculi also are common. Blue pigmentation of the sclera and ears are often the earliest changes, with the arthritic complications usually presenting after the age of 40.
- Primary adrenal insufficiency (Addison’s disease) is usually caused by autoimmune destruction of the adrenal glands leading to cutaneous hyperpigmentation and salt-wasting. The hyperpigmentation is secondary to increased production of adrenocorticotropic hormone (ACTH). The precursor molecule for ACTH, proopiomelanocortin, also produces melanin-stimulating hormone as a by-product leading to skin hyperpigmentation.
- Collagen synthesis diseases were considered. Congenital defects in collagen synthesis cause thinning of the sclera, which causes a bluish hue on examination. These defects include Ehlers-Danlos syndrome, osteogenesis imperfecta and, occasionally, Marfan’s syndrome.
Toxicity from systemic medications, topical medications and argyrosis also were considered:
- Systemic medications such as amiodarone, phenothiazines, minocycline and antimalarial agents may cause changes in skin and ocular pigmentation. Long-term use of prednisone has also been reported in the literature to cause scleral discoloration.1
- Topical medications such as epinephrine-containing eye drops can lead to pigmented deposits of the conjunctiva and eyelids. These deposits consist of the oxidized metabolites of epinephrine.
- Exposure to soluble silver compounds can lead to staining of the skin (argyria) or eyes (argyrosis). This staining can range from bluish gray to gray-black. Silver may be deposited in the skin either from industrial exposure or as a result of medications containing silver salts. These deposits are usually permanent.
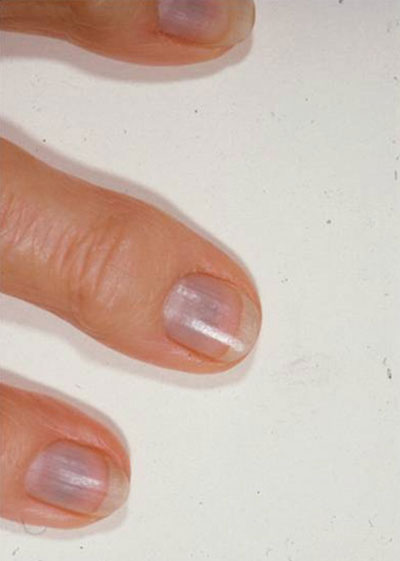 |
| Bluish discoloration of the fingernail beds of the patient's right hand. |
The Definitive Diagnosis
In addition to the scleral discoloration, we noticed that Ms. Green’s fingernails were a bluish color.
External examination also showed bluish discoloration of her brow, cheeks and pinna.
While the patient was referred to us for evaluation of oculodermal melanocytosis, that disease usually presents in childhood, is often unilateral and includes iris hyperpigmentation and uveal thickening, with no fingernail involvement. This patient’s findings were not consistent with that diagnosis.
Likewise, alkaptonuria seemed unlikely as the patient denied history of recent arthritis and there was no family history of a genetic disorder.
Given the discoloration of both sets of fingernail beds, pinna and sclera bilaterally, together with her long-term use of minocycline for rosacea (she had been taking 50 mg daily for 10 years, for a cumulative dose of 182.5 g), we diagnosed the patient as having minocycline-induced hyperpigmentation.
About the Discoloration
Minocycline is a semisynthetic tetracycline-derived antibiotic that is commonly used in the management of rosacea and acne vulgaris, and as an adjunct therapy in rheumatoid arthritis. Minocycline is a yellow crystalline substance that turns brownish black upon oxidation.
One of the metabolites may form insoluble complexes with melanin, iron or calcium and become deposited in various tissues of the body with a preponderance in sunlight-exposed tissues.2 Pigmentation generally results with long-term administration of accumulative doses greater than 100 g.3
In the eye, minocycline typically causes a bluish gray pigmentation of the sclera, although brownish black pigmentation has also been reported. The characteristic pattern consists of 3- to 5-mm bands that start at the limbus.4 The scleral pigmentation may or may not be accompanied by hyperpigmentation of other tissues such as the mucosa, gingivae, lips, heart valves, skin, teeth, fingernails and bone.3 The hyperpigmentation may resolve within years or it may be permanent after the drug is discontinued.3,4
Rare eye manifestations of minocycline use include eosinophilic conjunctival infiltrates5 and macular pigmented deposits.6
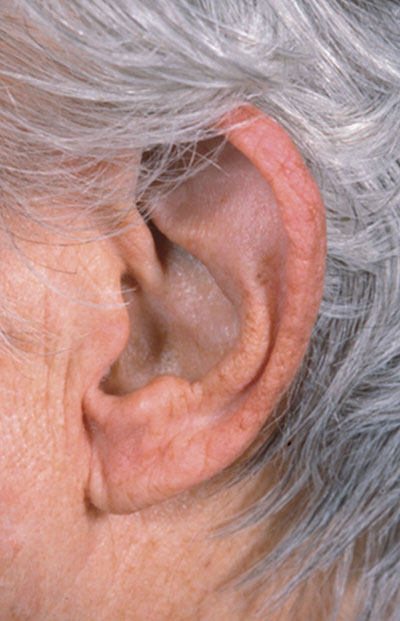 |
| Bluish discoloration of the pinna of the patient's left ear. |
Treatment
Patients generally should be screened for hyperpigmentation after one year of minocycline use. Hyperpigmentation of skin or sclera is an indication to discontinue the drug due to the permanent staining potential and the unknown effects on thyroid and other mucosal surfaces.4
Patient’s progress. The minocycline was discontinued, which led to partial reduction of ocular and nail pigmentation.
___________________________
* Patient name is fictitious.
___________________________
1 Henderson R. P. and R. Lander. Cutis 1984;34:76–77.
2 Hardman, J. G. et al. Goodman and Gilman’s The Pharmacological Basis of Therapeutics, 10th ed. New York: McGraw-Hill, 2001.
3 Eisen, D. and M. D. Hakim Drug Saf 1998;18:431–440.
4 Fraunfelder, F. T. and J. A. Randall Ophthalmology 1997;104:936–938.
5 Parc, C. et al. Br J Ophthalmol 2002;86:1313–1314.
6 Bradfield, Y. S., et al. Arch Ophthalmol 2003;121:144–145.
___________________________
Ms. Miraldi is a fourth-year medical student at Case Western Reserve University, Cleveland. Dr. Singh is associate professor of ophthalmology at the department of ophthalmic oncology and Dr. Jeng is assistant professor of ophthalmology at the department of cornea and external diseases; both are at the Cole Eye Institute, Cleveland.
Calling All Cases
Interested in sharing a mysterious or challenging case with your colleagues? Submit it to us at:
Morning Rounds, EyeNet Magazine,
655 Beach Street,
San Francisco, CA 94109
Phone: 866-561-8558
or 415-561-8500
eyenet@aao.org
Please contact us regarding writers guidelines and art requirements. Samples of previous columns also can be provided.
|