NOV 08, 2015
By Elias I. Traboulsi, MD
A Compendium of Inherited Disorders and the Eye, Oxford University Press
Genetics
OMIM Number
Inheritance
Gene/Gene Map
- Cystathionine b-synthetase
- 21q22.3
Epidemiology
- Incidence in Europe has been estimated at 1 in 40,000 newborns, which corresponds to a carrier (heterozygote) frequency of about 1%.
- In Ireland, where neonatal screening for homocystinuria is mandatory, incidence is 1 in 52,544 births.
- Incidence varies in different populations between 1 in 30,000 and 1 in 60,000 live births.
Clinical Findings
- Developmental delay
- Coarse, fair hair
- Connective tissue abnormalities cause skeletal and ocular findings similar to those of Marfan syndrome including ectopia lentis and myopia.
- Homocystine effects on vascular endothelium, platelets, and coagulation factors that predispose to repeated thromboembolic episodes.
- Malar flush
- The diagnosis is based on elevated homocystine in serum and urine.
- The urine nitroprusside test may be falsely negative in mildly affected adult patients. The sensitivity of this test can be improved by methionine loading.
Ocular Findings
- 38% of 5 year-old patients with untreated homocystinuria have lens subluxation, and almost all patients have it by age 25 (Figure 1). The zonules are absent, as compared to the stretched zonules in Marfan syndrome.
- The lenses move down and nasally in 50% of patients, posteriorly in 20%, and anteriorly in 10%. Pupillary block occurs in some patients with anterior lens subluxation and leads to elevation of intraocular pressure and to corneal decompensation from lens-endothelial contact.
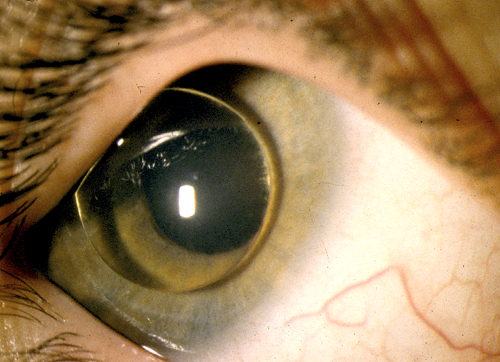
Figure 1. Totally dislocated lens in a patient with homocystinuria.
Therapeutic Aspects
- Supplementation with pyridoxine (50 to 1000 mg/day) results in clinical and biochemical improvement in 50% of patients.
- Vitamin B6 non-responders may benefit from a diet low in methionine and supplementation with cystine.
- Early detection and treatment using dietary restriction and vitamin supplementation in an Irish study of 14 patients by Burke et al resulted in the prevention of ectopia lentis after a mean follow-up of 8.2 years, compared with a 70% dislocation rate in untreated patients with a similar follow-up period. Ectopia lentis developed and progressed in 5 patients diagnosed later in life, despite tight biochemical control.
- The largest management series comes from a study of 45 patients from Saudi Arabia. 84 surgical procedures were performed on 40 patients: 82 were done with general anesthesia and 2 with local anesthesia. Medical therapy was attempted initially in all patients with lens dislocation and was the sole therapy used for 5 patients. 14 of the 45 patients (31%) were receiving dietary treatment at the time of presentation and 29 (64%) were mentally retarded. There were 2 surgical complications and 1 postsurgical complication. Lens dislocation into the anterior chamber was the most frequent indication for surgery (50%), followed by pupillary-block glaucoma (12%). Prophylactic peripheral iridectomy was not successful in preventing lens dislocation into the anterior chamber in 5 patients. Anesthetic precautions, such as stockings to prevent deep venous thrombosis, preoperative hydration, or aspirin, were taken in 85% of cases. Other common ophthalmic complications included optic atrophy (23%), iris atrophy (21%), anterior staphylomas (13%), lenticular opacities (9%), and corneal opacities (9%). The authors concluded that with the appropriate anesthetic precautions and modern microsurgical techniques, the risks associated with the surgical management of ocular complications of homocystinuria are reduced.
- If the lens is in the anterior chamber, dilation of the pupil and gentle pressure over the cornea can lead to repositioning of the lens behind the pupil. Patients are then administered pilocarpine, and a laser peripheral iridotomy is performed to prevent pupillary-block glaucoma. In the case of recurrent dislocations into the anterior chamber, a lensectomy should be performed. A primary lensectomy can also be performed.
- Prophylaxis of thromboembolic phenomena should be considered whenever these patients need general anesthesia. This should include a few weeks of supplementation with vitamin B6 before surgery, good intravenous hydration before and during surgery, and dipyridamole or acetylsalicylic acid daily before and after surgery is performed.
References
- Burke JP, O'Keefe M, Bowell R, et al: Ocular complications in homocystinuria: early and late treated. Br J Ophthalmol. 1989; 73:427-431.
- Cross HE, Jensen AD: Ocular manifestations in the Marfan syndrome and homocystinuria. Am J Ophthalmol. 1973; 75:405-419.
- Harrison DA, Mullaney PB, Mesfer SA, et al: Management of ophthalmic complications of homocystinuria. 1998; 105:1886-1890.
- Ramsey MS, Dickson DH: Lens fringe in homocystinuria. Br J Ophthalmol. 1975; 59:338-342.
Resources
Traboulsi EI. Compendium of Inherited Disorders and the Eye. New York: Oxford University Press; 2005. Adapted with permission.