Introduction
Although increasing myopia in the general population has been under much investigation, the normal development of the eye has traditionally been thought to be toward emmetropization. Statistically, the distribution of human refractive error is different from over variables like height, which typically have a Gaussian distribution. Human refraction is leptokurtic (Figure 1) and negatively skewed (toward myopia). There is, however, a preponderance of emmetropia in the human population as compared with refractive errors, which suggests that there is a process for emmetropization of the human eye.
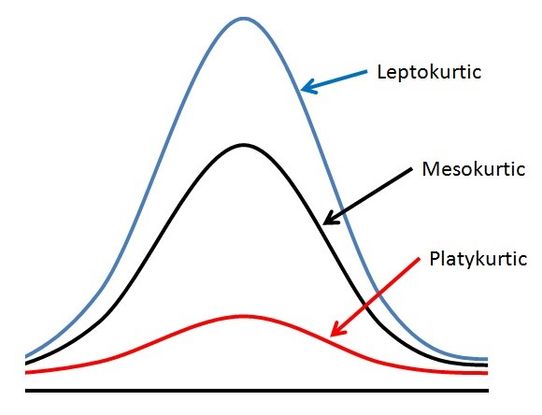
Figure 1. Leptokurtic: of a frequency distribution or its graphical representation, having greater kurtosis than the normal distribution; more concentrated about the mean.
There has also been much study of how the retina affects eye growth and refraction. Many animal studies and some human studies have shown that myopic defocus allows for hyperopic development, whereas hyperopic defocus allows for myopic development.1 This part of the eye development has led to significant research on optical corrections to halt myopic progression.
In refractive development, however, there seem to be 2 separate mechanisms. In infancy, there appears to be a mechanism toward emmetropia/low hyperopia. In later childhood, there is a tendency for myopic development. This has been previously shown, and adult refractions are illustrated in Figure 2.2,3
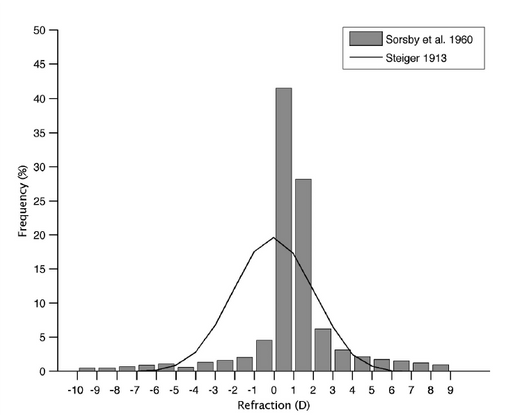
Figure 2. Adult refractions.
Development of Refraction Up to Age 6
At birth, infants display a wide range of refractive errors, which undergo a shift in average and reduction in the standard deviation, as shown in Figure 3.4 During this early stage, there are changes to the corneal curvature, axial length, and lens power. It is interesting to note that while during infancy there is a decrease in lens and corneal power, the cause of the increasing axial length is a process thought to be passive emmetropization.
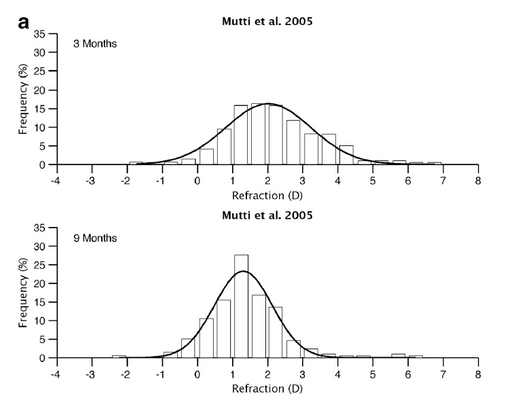
Figure 3. Shift in refraction between 3 months and 9 months of age.
At 1 year of age, there is a further shift toward emmetropization. There is significant reduction in the standard deviation, owing to a decrease in variability of refraction (which results in the leptokurtic shift in distribution) (Figure 4). Ingram and Barr also noted a decrease in astigmatism correction from 1 to 3.5 years of age.
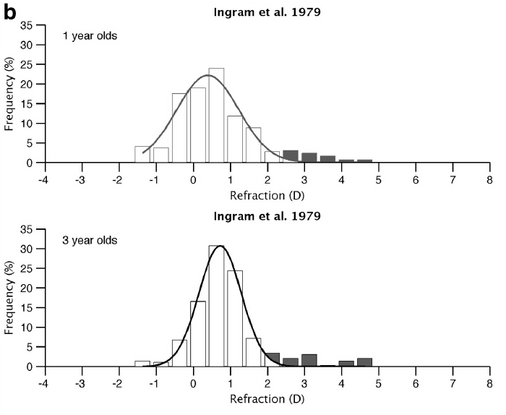
Figure 4. Reduction in standard deviation due to decreased variability in refraction between 1 and 3 years of age (leptokurtic shift).
Emmetropization continues at a slower rate after the age of 3 until around 6 years of age. Most children by the age of 6 will be, on average, 0.75 hyperopes with a shift toward higher hyperopia. The mean refraction is, however, lowest in Japan when compared to European countries and Australia. It is thought that refractive errors have been minimized in children by the age of 6, in terms of refractive error, astigmatism, and anisometropia.5 However, it is important to note that there are more children on the hyperopic side of Figure 46 than the myopic side. Those children appear to not have gone through emmetropization correctly and are effectively left behind. Between 3 and 6 years old is also the age group in which most children are diagnosed with disorders such as accommodative esotropia, which is heavily linked with high hyperopia.
Refractive Development After 6 Years of Age
After the age of 6, refractive development differs by population. In Australia, for instance, there is a continuing of emmetropization with low levels of myopia and hyperopia7 in European Caucasians. When comparing to Northern Ireland, French and colleagues note no difference in parental myopia, parental education, and educational standards, while these European Caucasian children have a higher rate of both hyperopia and myopia. The authors then speculate that further work on levels of near work and time spent outdoors is required. However, in eastern countries, there is an increasing level of myopia. In these countries, myopia is developing after the age of 6, which supports the theory that earlier emmetropization is unaltered. The rise in myopia seen, 49.3% to 65.6% in 17-year-olds in Japan (Figure 5), is seen as a sudden acceleration with a still-unknown mechanism.8
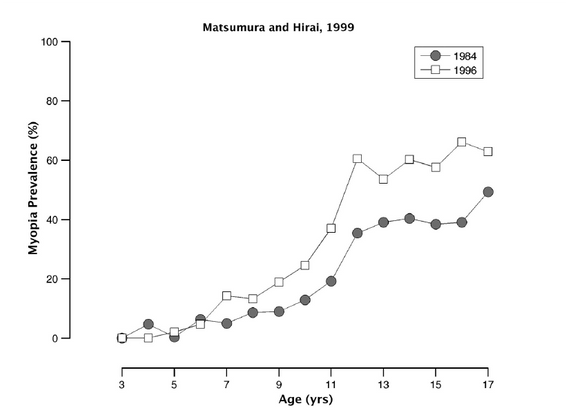
Figure 5. Rise in myopia in children between 7 and 17 years of age in Japan between 1984 and 1996.
It has been observed that if the onset of myopia is after the age of 6, there is an initial linear course followed by a rapid rise in myopia, then relative stability. The triggers for the sudden acceleration remain unknown. It is found that the increase in myopia is primarily due to increasing axial length, even when the onset is in adults.9
In contrast, refractive changes later in life appear to reflect changes in the optical power of the lens rather than the axial length. The lens continues to grow throughout adulthood and undergoes a change in the refractive index.10 However, the balance of opposing factors allows the refractive error of the eye to remain relatively stable. Even later, with the development of cataracts, the refractive shift is usually in the myopic direction.
References
- Wallman J, Winawer J. Homeostasis of eye growth and the question of myopia. Neuron. 2004;43(4):447-468. doi:10.1016/j.neuron.2004.08.008.
- Sorsby A, Sheridan M, Leary GA, Benjamin B. Vision, visual acuity, and ocular refraction of young men: findings in a sample of 1,033 subjects. Br Med J. 1960;1(5183):1394-1398.
- Stieger A. No Title. Die Entstehung der spharischen refraktiomen des menschlicen Auges. 1913;Krager(Berlin).
- Mutti DO, Mitchell GL, Jones LA, et al. Axial growth and changes in lenticular and corneal power during emmetropization in infants. Invest Ophthalmol Vis Sci. 2005;46(9):3074-3080. doi:10.1167/iovs.04-1040.
- Flitcroft DI. Emmetropisation and the aetiology of refractive errors. Eye (Lond). 2014;28(2):169-179. doi:10.1038/eye.2013.276.
- Ingram RM, Barr A. Changes in refraction between the ages of 1 and 3 1/2 years. Br J Ophthalmol. 1979;63(5):339-342.
- French AN, O’Donoghue L, Morgan IG, Saunders KJ, Mitchell P, Rose KA. Comparison of refraction and ocular biometry in European Caucasian children living in Northern Ireland and Sydney, Australia. Invest Ophthalmol Vis Sci. 2012;53(7):4021-4031. doi:10.1167/iovs.12-9556.
- Matsumura H, Hirai H. Prevalence of myopia and refractive changes in students from 3 to 17 years of age. Surv Ophthalmol. 1999;44 Suppl 1:S109-115.
- McBrien NA, Adams DW. A longitudinal investigation of adult-onset and adult-progression of myopia in an occupational group. Refractive and biometric findings. Invest Ophthalmol Vis Sci. 1997;38(2):321-333.
- Hemenger RP, Garner LF, Ooi CS. Change with age of the refractive index gradient of the human ocular lens. Invest Ophthalmol Vis Sci. 1995;36(3):703-707.