By Peggy Denny, Contributing Writer, interviewing Elizabeth A. Bradley, MD, John B. Holds, MD, and Ron W. Pelton, MD, PhD
Download PDF
Among the challenges faced by oculoplastic surgeons, management of patients on antithrombotic agents is one of the most complex. When deciding whether towithhold an antithrombotic, the surgeon must balance the systemic risks of thromboembolism against the very real possibility of periocular or orbital hemorrhage—which can potentially result in a compartment syndrome and blindness.
Compounding this dilemma is sparse clinical evidence and a lack of validated guidelines for perioperative management of antithrombotics for oculoplastic procedures.1,2 However, surgeons can benefit from guidance from their colleagues3 as well as from other medical specialties.
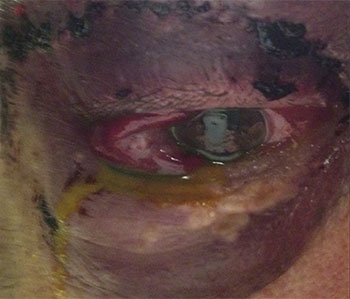 |
BLEEDING COMPLICATION. This patient, who was on aspirin, had retrobulbar hemorrhage in both eyes after blepharoplasty and subsequently lost vision in the right eye. Adapted from: Lee DW et al. Unilateral blindness due to retrobulbar hematoma after lower blepharoplasty. Arch Aesthetic Plast Surg . 2019;25(3):124-127. http://e-aaps.org. This is an Open Access article distributed under the terms of the Creative Commons Attribution Noncommercial 4.0 International License.
|
A Growing Concern
One thing is clear: The use of antithrombotic drugs is increasing in the oculoplastic patient population. John B. Holds, MD, who practices in St. Louis, has experienced this increase in his 30-plus years of practice. “When we count aspirin, we are now looking at 40% to 50% of my patients.” Ron W. Pelton, MD, PhD, who practices in Colorado Springs, Colorado, concurred: “I would estimate that more than half of my patients who are older than 75 are taking some type of blood thinner.”
Good news, bad news. Despite the burgeoning use of these drugs, however, it’s important to maintain perspective on the risk: Severe hemorrhagic complications have been reported in less than 1% of oculoplastic and orbital surgeries,4 said Elizabeth A. Bradley, MD, at the Mayo Clinic in Rochester, Minnesota. “One of the challenges of postoperative hemorrhages is that they’re such rare events that it can be very hard to learn from any specific event; you can’t generalize to your upcoming patients.” This is especially true given the specific characteristics of the various antithrombotic agents, the range of indications, and underlying risk factors such as hypertension.
Antiplatelets
The most widely used antiplatelet (APT) is aspirin, which may be suggested by a patient’s physician for prophylaxis against heart attack or stroke. More significantly, it may be prescribed by a cardiologist to reduce complications after heart valve replacement or cardiac stent, often in combination with another APT such as Plavix.
Most APTs are irreversible inhibitors of platelet function. That is, their effects last for the lifetime of a platelet, approximately eight or nine days. Thus, if these drugs are withheld perioperatively, they are stopped seven to 10 days before surgery3—a much longer time than with anticoagulants (ACs).
On the horizon? All available antithrombotics pose the risk of bleeding events. Now, cutting-edge research is investigating a novel pathway for reducing platelet adhesion without affecting hemostasis. The drugs under investigation target phosphoinositide 3-kinase, which plays a role in platelet structure, and early results show promising antithrombotic properties without increased bleeding time.5
Anticoagulants
This category of antithrombotics has attracted the greatest interest in the last decade, with the approval of the first direct-acting oral anticoagulant (DOAC) in 2010. Since then, DOACs such as Eliquis and Xarelto have been rapidly adopted.6
Advantage: DOACs. Dr. Bradley said that she sees patients on DOACs daily. “Atrial fibrillation (AFib) is a big issue, and it seems that these patients are more likely now to be on one of the newer agents than on warfarin.” The revised joint guidelines issued by the American Heart Association, American College of Cardiology, and Heart Rhythm Society favor DOACS over warfarin for most patients with AFib because of proven efficacy, better safety profile, fewer drug interactions, and simpler dosing regimens.7
Of particular interest to ophthalmic surgeons, a 2019 study found a 22% relative risk reduction overall in intraocular bleeding in patients taking DOACs compared with those on warfarin.2
Special considerations. Despite their many advantages, DOACs “may be more vexing than warfarin,” said Dr. Holds. Because warfarin has been in wide use since 1954, many ophthalmologists are better acquainted with its action and side effects, so it is important for surgeons to be informed of the ways in which DOACs are different.
DOACs have shorter half-lives than warfarin and, more significantly, much more rapid onset and cessation of anti-thrombotic action. Thus, they can be discontinued closer to surgery but are generally withheld longer postoperatively, than warfarin. Although DOACs may be restarted the next day in low–bleeding-risk surgeries,8 some experts suggest delaying resumption up to four days after higher-risk surgery, if the patient’s cardiovascular risk factors allow.4
In addition, “The pharmacokinetic properties of each DOAC can vary depending on the renal and liver function of the patient,” said Dr. Pelton. This may necessitate consultation with the prescribing physician.3
Finally, if hemorrhage does occur, reversal of the anticoagulant effect may be more difficult with DOACs. Although a reversal agent is available for some of the DOACs, said Dr. Holds, “It’s not immediately effective, it’s quite expensive, and it may be unavailable.”
To Hold, or Not to Hold?
Should patients discontinue their antithrombotics during the perioperative period? The decision is influenced by the patient’s risk factors and the bleeding risk posed by the specific surgery.
Consider patient risk factors. “I’m more concerned about the reasons that the patient is on anticoagulant therapy than I am about the drug itself,” said Dr. Pelton. “For example, if a patient is taking ‘baby aspirin’ because their primary care physician told them it might be helpful for prophylactic reasons, I’m much less worried about stopping that medication than I would be for a patient who has had cardiac stents placed.”
Dr. Holds finds the guidelines from the American College of Surgeons to be helpful in decision-making. Although not specific to ophthalmology, they suggest timetables for perioperative management of these drugs and provide estimates of the risk of thromboembolic events if drugs are withheld.8
Consult with the prescribing physician. “It is essential to coordinate with the other physicians involved in managing the patient’s antithrombotic regimen for any proposed perioperative modification,” said Dr. Holds. Dr. Pelton uses a standard form, which he faxes to the prescribing physician.
However, Dr. Bradley said that, depending on the medical indication, she may make the decision independently. “If they’re on medication for a heart valve or a coagulopathy, I always check with the prescribing physician. If they’re taking warfarin for AFib and they’ve never had a stroke, I may make the decision to ask them to hold it for a few days before and resume a day after.”
Assess the surgical risk. Dr. Bradley listed her procedures of greatest con-cern: “Anything where I’m going behind the orbital septum, meaning all orbital surgery and most eyelid surgery. Also, lacrimal cases that involve working in the nose.” Even with these higher–bleeding-risk procedures, it’s important to remember that the incidence of hemorrhagic complications is low. Nevertheless, about 25% of oculoplastic surgeons would withhold APTs and ACs for the lower–bleeding-risk procedures, and more than 90% would do so for the higher-risk surgeries.1
Delay or Proceed?
When to delay surgery. Except in emergencies, it may be preferable to defer a procedure until the patient is able to discontinue antithrombotics. For cosmetic procedures, said Dr. Pelton, “I am more likely to ask the anticoagulated patient to wait until the medications can be stopped (if possible) before scheduling surgery.”
Dr. Holds added that he would defer procedures that are in any way elective, including dacryocystorhinostomy, in patients who are taking antithrombotics following a stent placement or stroke within the prior six months.
When to proceed with caution. However, the situation is not always clear-cut. A procedure might be beneficial, and otherwise appropriate, for a patient who cannot discontinue anti-thrombotics. Dr. Bradley said, “If it looks like they’ll be on anticoagulation long term, and they have a good assessment of the risk, I’ll go ahead in some cases. Certainly for a skin cancer, I’m always willing to go ahead with that.”
Think Outside the Rx
Patients are usually aware of the bleeding risks from their prescribed antithrombotics, but they might not realize that their gingko herbal tea can affect their surgical outcome.
Dr. Pelton said that he is especially concerned about over-the-counter NSAIDs, vitamins, and herbs. “Many of these have anticoagulant properties, but since they are not prescribed, patients often don’t consider them to be ‘medication’ and don’t include them on their meds list.” To counteract this, Dr. Pelton has created a checklist of problematic drugs and supplements to give to patients.1
___________________________
1 www.omic.com/hemorrhage-associated-with-ophthalmic-procedures/. Accessed June 1, 2021.
|
How to Mitigate Risk
Do a thorough pre-op assessment. Pay particular attention to bleeding disorders, medication history (especially ACs), and use of herbal or vitamin supplements (see “Think Outside the Rx”). Ask about a history of AFib, valvular heart disease, deep venous thromboembolism, cerebrovascular disease (stroke), hypertension, and cardiac stents; and consult with the physician who prescribed any antithrombotics, said Dr. Pelton.
Tailor the informed consent appropriately. Discuss and document the increased risk of ocular hemorrhage if medications are continued, and the increased risk of clotting and stroke if they are stopped.3 Dr. Bradley also tells patients that even if they hold the drugs for a few days, some may still be circulating systemically, so they may experience additional bleeding or bruising.
Communicate with the medical team. Dr. Pelton said that a well-informed perioperative team can help educate the patient, prepare the OR with essential equipment and drugs (e.g., suction, cautery, gel foam, thrombin), and monitor for signs of complications.
Alter your surgical plans as needed. “I alter the technique I use for eyelid surgery by not opening the orbital septum if the patient is on blood thinners,” said Dr. Pelton. He added that for procedures that require extensive dissection (such as a large Mohs surgery repair) in patients on antithrombotics, he is more likely to ask for general anesthesia because the extensive cautery can be uncomfortable and may raise the patient’s blood pressure. “I’m also more likely to use ancillary substances such as gel foam and thrombin as well as pressure bandages and drains in anticoagulated patients.”
Dr. Holds said that he is prepared to “back off” from his plan if he suspects bleeding problems. For example, in a functional blepharoplasty, he might address just the overhanging eyelid skin rather than also removing some fat to improve the appearance. He advised that good communication is essential to let patients know that any such changes are done for their safety.
Another technique that Dr. Holds finds useful in curtailing bleeding is the addition of tranexamic acid to the local anesthetic. Although its efficacy has not been proven in a randomized clinical trial in oculoplastics, a systematic review of plastic surgery literature showed a clear benefit in controlling bleeding with minimal complications.9
Know how to manage hemorrhage. Prompt intervention is critical; in severe cases, there may be little time between the onset of symptoms and irreversible visual loss. And any colleague who is covering for you must also know how to manage complications, particularly orbital compartment syndrome.3
Commonly Used Antithrombotic Agents
|
Drug (Brand Name)
|
Mechanism of Action
|
Half-life
|
Last Pre-op Dose
|
|
Antiplatelets
|
|
Aspirin
|
Irreversible COX inhibitor
|
3-10 hours
|
7 days
|
|
Clopidogrel (Plavix)
|
Irreversible ADP receptor antagonist
|
8 hours
|
5-7 days
|
|
Prasugrel (Effient)
|
Irreversible ADP receptor antagonist
|
7 hours
|
5-7 days
|
|
Anticoagulants
|
|
Warfarin (Coumadin)
|
Vitamin K antagonist
|
20-60 hours
|
5 days
|
|
Apixaban (Eliquis)
|
Direct factor Xa inhibitor
|
12 hours
|
24-48 hours*
|
|
Dabigatran (Pradaxa)
|
Direct thrombin inhibitor
|
8-15 hours
|
24-48 hours*
|
|
Edoxaban (Savaysa)
|
Direct factor Xa inhibitor
|
10-14 hours
|
24-48 hours*
|
|
Rivaroxaban (Xarelto)
|
Direct factor Xa inhibitor
|
5-13 hours
|
24-48 hours*
|
|
*Applies only to patients with normal renal function.
ADP = adenosine phosphate receptor; COX = cyclooxygenase.
SOURCE: Adapted from Hornor MA et al. J Am Coll Surg. 2018;227(5):521-536
|
Maintaining Perspective
Finally, although the consequences of not stopping antithrombotic agents can be devastating, Dr. Bradley emphasized the rarity of serious hemorrhagic events. Moreover, studies have shown the risk of thromboembolic events following perioperative cessation of drugs to be similar or higher than for hemorrhage.1
Thus, there are no simple answers—and the most important point is to consider the medical history, surgical indications, and personal preferences of each patient, Dr. Bradley noted.
___________________________
1 Esparaz ES, Sobel RK. Curr Opin Ophthalmol. 2015;26(5):422-428.
2 Makuloluwa AK et al. Eye (Lond). 2019;33:1044-1059.
3 www.omic.com/hemorrhage-associated-with-ophthalmic-procedures/. Accessed June 1, 2021.
4 Wagner LH et al. Orbit. 2021;40(2)150-154.
5 Selvadurai MV et al. Sci Transl Med. 2020;12(553):eaar8430.
6 Chen A et al. J Am Heart Assoc. 2020;9(13):e017559.
7 January CT et al. Circulation. 2019;140(2):e125-e151.
8 Hornor MA et al. J Am Coll Sur. 2018;227(5):521-536.
9 Scarafoni EE. Plast Reconstr Surg Glob Open. 2021;9:e3172.
___________________________
Dr. Bradley is associate professor of ophthalmology at the Mayo Clinic in Rochester, Minn. Relevant financial disclosures: None.
Dr. Holds is an oculoplastic surgeon and partner at Ophthalmic Plastic and Cosmetic Surgery in St. Louis. Relevant financial disclosures: None.
Dr. Pelton is an oculoplastic surgeon in private practice in Colorado Springs, Colo. He also is a Trustee-at-Large for the Academy and serves on the board of directors of OMIC. Relevant financial disclosures: OMIC: C.
For full disclosures and the disclosure key, see below.
Full Financial Disclosures
Dr. Bradley None.
Dr. Holds Cypris Medical: O; Horizon Therapeutics: C,O; Revance Therapeutics: O; Sun Biopharma: O.
Dr Pelton OMIC: C.
Disclosure Category
|
Code
|
Description
|
| Consultant/Advisor |
C |
Consultant fee, paid advisory boards, or fees for attending a meeting. |
| Employee |
E |
Employed by a commercial company. |
| Speakers bureau |
L |
Lecture fees or honoraria, travel fees or reimbursements when speaking at the invitation of a commercial company. |
| Equity owner |
O |
Equity ownership/stock options in publicly or privately traded firms, excluding mutual funds. |
| Patents/Royalty |
P |
Patents and/or royalties for intellectual property. |
| Grant support |
S |
Grant support or other financial support to the investigator from all sources, including research support from government agencies (e.g., NIH), foundations, device manufacturers, and/or pharmaceutical companies. |
|