Download PDF
Researchers have harnessed artificial intelligence (AI) to create a reliable prediction model for progression to atrophic and/or neovascular age-related macular degeneration (AMD).1 The AI algorithm identified nine risk factors from a larger set of phenotypic, genetic, and lifestyle predictors.
“The model could be used for patients showing some early signs of AMD, to identify those most at risk of progression to advanced AMD,” said Cécile Delcourt, PhD, at the Université de Bordeaux in France. It also has implications for making recommendations to patients regarding their lifestyle and the frequency of follow-up visits. Moreover, it might be used for testing or adopting new therapies or interventions and for patient selection in clinical trials, she said.
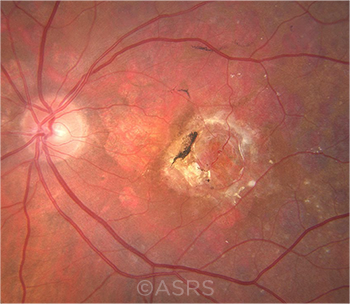 |
BIOMARKER. Human neuronal cells show fibrillar staining for NfL (red). Cell nuclei of some non-neuronal cells are also evident (blue).This image was originally published in the ASRS Retina Image Bank. Pamela Rowlett, CRA. Exudative Macular Degeneration. Retina Image Bank. 2019; Image Number 29991. © The American Society of Retina Specialists.
|
Data from two population-based cohort studies. The prediction algorithm was trained using data from 3,838 participants from the Rotterdam Study 1. These patients did not have advanced AMD at baseline and were age 55 or older. During a mean follow-up of 10.8 years, 108 incident cases of advanced AMD were detected.
The model was validated using 362 participants from the ALIENOR study, who were age 73 or older. During a median follow-up of 6.5 years, 33 incident cases of AMD were diagnosed.
Machine-selected variables. The four strongest risk factors for progression were genetic risk score, the score from AREDS (Age-Related Eye Disease Study), presence of intermediate drusen, and age.
These were followed in importance by smoking, pulse pressure, presence of retinal hyperpigmentation, education, and the Mediterranean diet score. Of note, pulse pressure and the Mediterranean diet have not appeared in earlier prediction models.
Three risk categories. The algorithm also estimated the cumulative incidence of advanced AMD, categorizing risk as low, intermediate, or high. In both the training and validation cohorts, incidence in the high-risk group increased steeply from baseline. The low- and intermediate-risk cohorts showed lower incidence rates across all time points.
Waiting for approval. The prediction model, which will be available to clinicians via www.macutest.net, is awaiting FDA approval in the United States and CE marking for Europe. Putting it into practice will require three steps: 1) The ophthalmologist will need to enter clinical exam findings, such as presence of drusen and retinal pigmentary abnormalities; 2) the patient must supply lifestyle information; and 3) a genetic sample should be taken, with results directly entered into the system. “The genetic test is performed only once,” Dr. Delcourt said, “but the ophthalmological and lifestyle information can be filled in at each visit to monitor the risk evolution.”
Because genetic testing is not currently available in routine ophthalmology practices, there is an alternative model that excludes the genetic risk score, with comparable results, she said.
—Miriam Karmel
___________________________
1 Ajana S et al. Ophthalmology. Published online Sept. 2, 2020.
___________________________
Relevant financial disclosures—Dr. Delcourt: None.
For full disclosures and the disclosure key, see below.
Full Financial Disclosures
Dr. Boland Carl Zeiss Meditec: C.
Dr. Ciolino TherOptix: C,O,P.
Dr. Delcourt Allergan: C; Bausch + Lomb: C; Laboratoires Théa: C; Novartis: C.
Dr. Subramanian None.
Disclosure Category
|
Code
|
Description
|
| Consultant/Advisor |
C |
Consultant fee, paid advisory boards, or fees for attending a meeting. |
| Employee |
E |
Employed by a commercial company. |
| Speakers bureau |
L |
Lecture fees or honoraria, travel fees or reimbursements when speaking at the invitation of a commercial company. |
| Equity owner |
O |
Equity ownership/stock options in publicly or privately traded firms, excluding mutual funds. |
| Patents/Royalty |
P |
Patents and/or royalties for intellectual property. |
| Grant support |
S |
Grant support or other financial support to the investigator from all sources, including research support from government agencies (e.g., NIH), foundations, device manufacturers, and/or pharmaceutical companies. |
|
More from this month’s News in Review