Download PDF
Stevens-Johnson syndrome (SJS) and the related entity, toxic epidermal necrolysis (TEN), may precipitate a particularly devastating conjunctivitis, in which the initial inflammatory destruction of the ocular surface is eventually superseded by a tenacious fibrosis that fuses the eyes to the surrounding adnexa. Because both SJS and TEN are so uncommon (only 7 cases per million persons annually), there is little scientific evidence regarding their ocular management; and enrolling enough patients in treatment trials to provide adequate statistical power for the results is nearly impossible.1 Possibly as a consequence, no topical or systemic SJS medical therapy has proven therapeutic benefit to the eye. The only intervention that has demonstrated efficacy is the application of amniotic membrane (AM) during the acute phase of the disease.2,3
Types of Amniotic Membrane
Two main forms of AM are commercially available in the United States. The first is large, preserved sheets, which can be applied anywhere along the eye, lids, or lashes. The second consists of AM drums stretched across circular symblepharon rings, designed to center over the cornea. They provide only limited coverage, extending just beyond the limbus. These AM-covered rings (ACRs, marketed as ProKera) have achieved widespread popularity, in part because of their ease of use.
Despite the advantage in convenience, we believe that this type of self-retained cornea/limbus-covering device alone does not provide adequate protection of the ocular surface, as the lid margin and fornix are not covered. Following is our rationale, along with a case example from our practice that demonstrates this point.
 |
|
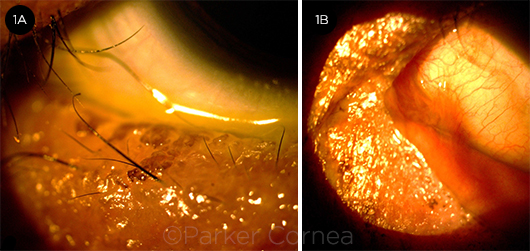
OCULAR SURFACE AFTER ACR. Several months after acute SJS conjunctivitis that was treated with bilateral ACRs, this patient has (1A) severe eyelid margin keratinization, irregularity, trichiasis, and meibomian gland dropout. (1B) Symblephara are evident nasally, beyond the area covered by the ACR.
|
SJS Requires Extensive Surface Protection
SJS is an inflammatory condition of the skin and mucous membranes. In the eyes, it manifests primarily as a palpebral, bulbar, and forniceal conjunctivitis. Secondarily, the eyelids, lashes, and cornea may also become involved. The mechanism underlying these pathologies appears to be the widespread CD8 T-helper cell–mediated destruction of the body’s keratinocytes (not keratocytes).1
From an ophthalmic standpoint, the worst damage occurs around the eye rather than to the globe itself, specifically, to the lacrimal gland tubules, meibomian glands, conjunctival goblet cells, lash follicles, and lid margins. These insults, combined with the fibrosis that frequently follows, destroy the conjunctiva and produce badly damaged and dysfunctional lids that may poorly protect and ultimately injure the cornea.
Therefore, although the cornea is often the focus of therapeutic attention in SJS, it is arguably the least directly involved structure, as it is affected secondarily by injury to surrounding tissues. Consequently, protecting the cornea may depend on preventing preceding damage to the lids, lashes, and conjunctiva during the acute phase of the disease; and anti-inflammatory therapy should be directed preferentially to these areas. Conversely, therapeutic efforts directed solely at the cornea (for example, ACRs) may be frustrated by failure in the long term, since the underlying pathology is left unaddressed.
SJS Case Study
Recently, a patient was referred to our practice after her release from a rehabilitation center where she had been recovering from an attack of SJS, with onset 2 months prior. Although skin lesions had healed, her eyes were extremely uncomfortable, and her visual acuity was reduced to 20/70 (0.3 decimal) bilaterally. Examination revealed 3+ punctate epithelial erosions, lid margin keratinization, trichiasis, and symblephara in both eyes (Fig. 1).
Severe damage despite ACRs. A review of the patient’s medical records revealed that during the acute phase of her disease, her treatment consisted of bilateral ACRs and topical steroids. Nevertheless, she went on to develop severe cicatrizing deformities in both eyes. This suggests the possibility that the therapy she received was inadequate and, specifically, that ACRs alone may not provide sufficient coverage to protect the eye against the worst manifestations of SJS.
ACRs occupy the same position in the eye as large contact lenses. Although these devices come in several sizes and profiles, none stretch far beyond the corneal limbus. Thus, the majority of the ocular surface (including the bulk of the conjunctiva, the lids, and the lashes) is left unprotected. And because these latter structures are the primary site of injury in SJS, the presence of an ACR alone may have little to no effect in preventing the most dreaded outcomes, including permanent eyelid deformities and extensive symblephara.
 |
|
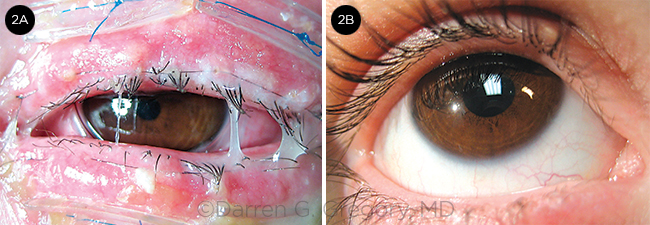
SJS RECOVERY. This patient was treated by Darren G. Gregory, MD, at the University of Colorado, Denver. (2A) Ten days after transplant, there was a mucopurulent appearance as the AM degraded, but no infection. (2B) Four months later, the patient was completely recovered, with no sequelae.
|
How to Use AM Sheets
Rather than ACRs, free sheets of AM should be used in cases similar to our patient’s. The sheets should be draped and sutured over the inner and outer aspects of the upper and lower lids, covering the lid margins and pressed deep down into the superior and inferior fornices. Likewise, the globe should be covered with a sheet of AM, placed over the cornea, sutured around the limbus, and with the edges wrapped around the eye as posteriorly as possible. Alternatively, an ACR may be placed on the eye, but this should supplement, not supplant, the use of AM sheets for the fornices, lids, and lashes.
This type of coverage, though laborious and time consuming, is—in our opinion—necessary rather than optional for patients with advanced or progressive conjunctivitis stemming from SJS. The procedure may be performed in the operating room or, less conveniently, at the bedside.3 The ideal treatment window may be within the first 2 to 3 weeks after disease onset, during the acute phase, when the predominant expression of pathology is inflammation. After this time period, a reactive fibrosis may ensue, against which AM grafts appear to be less effective.
Do all SJS patients need AM? Not all patients with SJS-mediated conjunctivitis require AM grafting. Individuals with milder manifestations (consisting of slight irritative symptoms and/or trace conjunctival injection) may be managed expectantly with daily exams and topical steroids.
However, if the ocular involvement appears more severe, if corneal or conjunctival epithelial defects are found, or if frank symblephara are present, then prompt AM transplantation may be warranted. And under these conditions, we consider that it is more appropriate to treat comprehensively, with lid, lash, and forniceal covering sheets of amniotic membrane, than with ACRs alone.
Therefore, as a general rule of thumb, it may be said that although AM transplantation may not be necessary for all patients with SJS and ocular involvement, those who do require it should receive protection for the sites of primary disease activity, including the lids, lashes, and fornices. Put another way: “If it’s worth doing, it’s worth doing right.”
Conclusion
Based on our recent experience with the above patient, from similar cases (Fig. 2), and from our theoretical understanding of the nature of SJS, we have concluded that ACRs alone are not suitable for patients with SJS and ocular involvement. Although the patient described above is not the first report of failure of AM rings in patients with SJS, we feel that the inadequacy of this treatment strategy warrants further emphasis, as it is still being used.4-7
___________________________
1 Ciralsky JB et al. Curr Opin Ophthalmol. 2013;24(4):321-328.
2 Hsu M et al. Cornea. 2012;31(12):1394-1402.
3 Gregory DG. Ophthalmology. 2011;118(5):908-914.
4 Shammas MC et al. Am J Ophthalmol. 2010;149(2):203-213.
5 Shay E et al. Cornea. 2010;29(3):359-361.
6 Kolomeyer AM et al. Eye Contact Lens. 2013;39(3)e7-11.
7 Thomas L et al. J Pediatr. 2016;175(6):235.
___________________________
Ms. Cooper is a medical student at Louisiana State University in New Orleans. Dr. John Parker is a corneal specialist at Parker Cornea, in Birmingham, Ala. Dr. Jack Parker is corneal fellow at the Netherlands Institute for Innovative Ocular Surgery in Rotterdam, the Netherlands. Relevant financial disclosures: None.