Download PDF
This month, News in Review Highlights selected papers from the original papers sessions at AAO 2016. Each was chosen by the session chair because it presents important news or illustrates a trend in the field. Only 4 subspecialties are included here; papers sessions will also be held in 6 other fields. See the Meeting Program, which you’ll find in your meeting bag, or the Mobile Meeting Guide for more information.
Unlike conventional fluorescein angiography (FA), which mainly provides information about retinal circulation, a noninvasive, 3-D alternative is able to delineate the extent of capillary dysfunction in both superficial and deep vascular plexuses in nonproliferative diabetic retinopathy (NPDR), said K.V. Chalam, MD, PhD. He added that this technique, called split-spectrum amplitude-decorrelation angiography (SSADA)–assisted OCT angiography (OCT-A), uses a specialized processing algorithm to provide information about blood flow at 3 depths: superficial capillary, deep capillary, and choroidal.
Technical progress. Developed a few years ago at the Casey Eye Institute of Oregon Health & Science University, in Portland, SSADA-assisted OCT-A is based on detecting reflectance amplitude variation of blood flow over time. By decreasing the signal-to-noise ratio of flow detection, it enhances visualization of retinal vasculature using motion contrast. “Rather than using dye to highlight movement and create a 2-D image, it captures frame after frame, enhancing the moving particles in an image while suppressing the static particles,” said Dr. Chalam, at the University of Florida in Jacksonville.
Early use of OCT for angiography was clinically impractical, he said, because it required multiple and repeated scans at each location to build the angiogram. But the new algorithm speeds the process because only 2 scans are needed at each location to produce a high-quality angiogram.
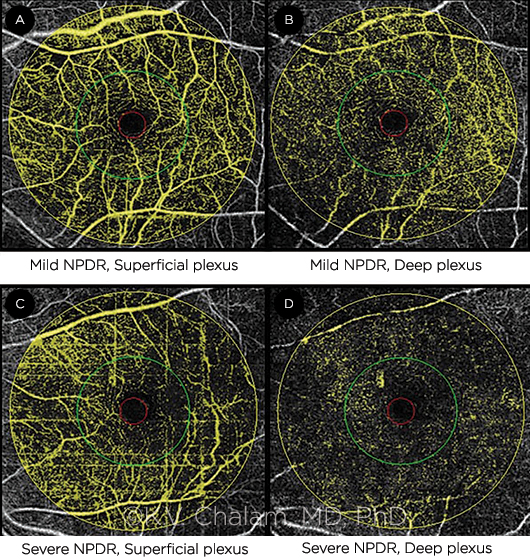 |
OCT ANGIOGRAPHY. (A, B) Mild NPDR. Vessel densities (VDs) in parafoveal and perifoveal areas, respectively, were 33% and 42% in superficial plexus (A) and 20% and 29% in deep plexus (B). (C, D) Severe NPDR. VDs were 18% and 21% in superficial plexus (C) and 7% and 9% in deep plexus (D) for the respective areas.
|
Results with NPDR. For the study being presented at AAO 2016, OCT-A was obtained in 128 eyes of patients with NPDR using SSADA software to determine indices for 3 levels of flow in the perifoveal area. Compared with age-matched controls, patients with NPDR had severe compromise of the deep capillary macular vascular flow. Specifically, the mean deep perifoveal vessel density in NPDR was 13 ± 4.71% versus 48 ± 11.01% in controls. In addition, the mean macular deep vascular flow rate in NPDR was 0.009 versus 0.055 in controls.
Clinical use. “Because this technique allows you to see movement at different depths, it can detect diabetic changes sooner than with a typical angiogram,” said Dr. Chalam. “Being able to measure the amount and density of blood flow helps quantify changes within a particular radius, he said, with the level of compromise proportional to the degree of diabetic retinopathy.
“Because of its ease and speed of use,” said Dr. Chalam, “this technology may be used more frequently, helping to identify the degree of damage in newly diagnosed patients and helping to monitor a patient’s disease progression—something that can’t be done using other technology.” On the downside, he said, it cannot evaluate vascular permeability, as can be done with a traditional angiogram.
Currently, Optovue’s Avanti with SSADA software is the only such system approved by the FDA; a similar system by Topcon is being investigated. Although the technology is not currently in widespread use, Dr. Chalam foresees its clinical utility for a range of other problems such as macular degeneration and vascular occlusion.
—Annie Stuart
| OCT Angiography Reveals Severe Attenuation of Deep Capillary Macular Vascular Flow Index in Nonproliferative Diabetic Retinopathy. When: Sunday, Oct. 16, 3:00-3:07 p.m., during the first retina, vitreous original papers session (2:00-5:30 p.m.). Where: S405. Access: Free. |
___________________________
Relevant financial disclosures—Dr. Chalam: None.
See the disclosure key at www.aao.org/eyenet/disclosures.
More from this month’s News in Review