Blink
Post-Canaloplasty Corneal Complications
By Sylvia H. Chen, MD-CM, MBA, and photographed by Glenn Ottenbreit, University of British Columbia Department of Ophthalmology and Visual Sciences, Vancouver, Canada
Download PDF
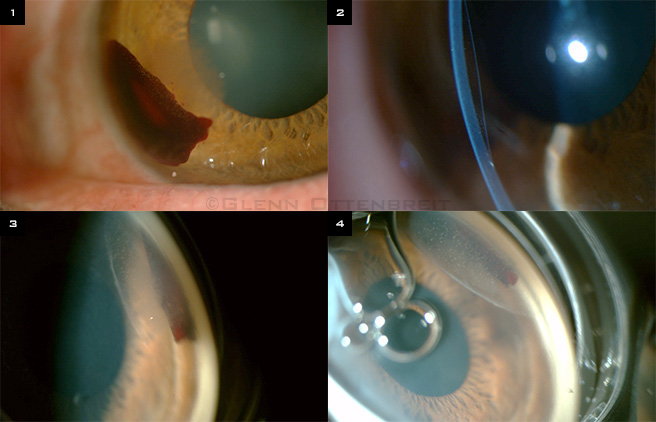
A 47-year-old man had a canaloplasty to manage his open-angle glaucoma; his presurgery intraocular pressure (IOP) was in the 30s despite maximal medical therapy. Intraoperatively, a small intracorneal hematoma was noted (Fig. 1). A small Descemet’s detachment (Fig. 2) was noted on slit-lamp examination two weeks after surgery. Both were visualized on gonioscopic examination (Figs. 3 and 4).
During this procedure, cannulation or viscodilation of Schlemm’s canal can cause a perforation from the canal of Schlemm through Schwalbe’s line and create a space between Descemet’s membrane and the corneal stroma. Viscoelastic or refluxed blood can collect there, causing a Descemet’s membrane detachment.
In a three-year follow-up of 157 canaloplasty patients, Descemet’s membrane detachment was noted in 3.2 percent.1 The intracorneal hematoma can be managed in any of the following ways: observation for resolution or worsening; YAG disruption to create a Descemet’s membrane break and disperse blood into the anterior chamber; or surgical removal (e.g., partial-thickness paracenteses and air tamponade).
We initially managed the patient with close observation for six months, until the Descemet’s detachment started to grow and encroach upon the visual axis. It was surgically removed, and the patient had a full recovery to 20/20 vision. At one year postop, his IOP of 16 mmHg was well controlled with one glaucoma drop.
__________________________
1 Lewis RA et al. J Cataract Refract Surg. 2011;37(4):682-690.
| BLINK SUBMISSIONS: Send us your ophthalmic image and its explanation in 150-250 words. E-mail to eyenet@aao.org, fax to 415-561-8575, or mail to EyeNet Magazine, 655 Beach Street, San Francisco, CA 94109. Please note that EyeNet reserves the right to edit Blink submissions. |