By Laura J. Rongé, Contributing Writer
This article is from April 2004 and may contain outdated material.
Getting patients to “stay on the wagon” is a challenge when treating chronic blepharitis, noted James P. McCulley, MD. “This is a frustrating group of patients. They have a chronic disease that we cannot cure, but with intense therapy, we can bring it under control—and then, with lesser therapy, we can maintain control over time,” said Dr. McCulley, professor and chairman of ophthalmology at the University of Texas Southwestern Medical Center, Dallas.
These patients often have a vicious cycle of disease, with blepharitis, meibomian gland dysfunction (MGD) and dry eye perpetuating each other, noted William D. Mathers, MD, professor of Ophthalmology at Oregon Health & Science University, Portland.
Dr. Mathers pointed out that the chronic inflammation of blepharitis irritates the eye surface and inhibits tear production. The reduced tear flow doesn’t wash inflammatory products away from the lid margin, so they accumulate and create inflammation.
 |
|
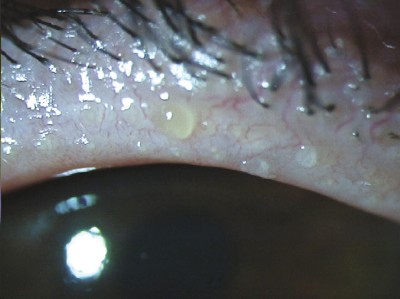
Patients with meibomianitis (shown here) have a distinct abnormality in one of the polar lipids that destabilizes the tear film, recent research shows.
|
Three Culprits to Chase
1. Bacteria. Chronic bacterial growth (usually Staphylococcus) on the lid may cause blepharitis. This is not an infection, Dr. Mathers noted. Instead, the bacteria produce toxins that inflame the lid. This causes the orifices in the meibomian gland to keratinize, obstructing the meibomian glands. In turn, this leads to chalazia and chronic inflammation.
2. Lipid layer changes. Dr. McCulley expects that a change in the biochemical makeup of the meibomian secretions contributes to disease. His research team is studying the changes in the lipid layers of meibomian secretions. “By looking at the lipid layer makeup in an individual, I can with 95 percent-plus confidence make a clinical diagnosis.”
Dr. McCulley noted that specific lipid changes occur in each type of chronic blepharitis:
- Meibomian seborrhea. In these patients, whose chief complaint is typically that of a burning sensation, he finds an increased concentration of oleic acid, a specific free fatty acid, in their tears.
- Primary meibomianitis. These patients have a distinct abnormality in one of the polar lipids that destabilizes the tear film.
- Chronic blepharitis and ocular surface drying. In these patients, Dr. McCulley has found a deficiency in two polar lipids that are key to the function of the polar lipid layer.
Do omega-3 essential fatty acids play a role? “To date, we have found no omega-3s in the meibomian secretions. We have found linoleic acid, an omega-6, but its role is not known,” Dr. McCulley said.
He is just beginning research on a dietary supplement rich in omega-3s to look for effects on blepharitis or aqueous-deficient dry eyes. “I don’t know if it will potentially be incorporated into the meibomian secretions or whether it will have an effect at an upstream point in decreasing inflammation.” Anecdotal evidence “suggests that these omega-3s do great things. We are going to find out. We don’t yet have science to direct us in one way or another,” he said.
3. Rosacea. This skin disease is associated with both obstructive and seborrheic MGD, Dr. Mathers said.
Rosacea patients have skin changes of dilation and inflammation, eye irritation and lid scarring, but Dr. Mathers pointed out that clinicians often miss these signs. Anyone with malar flushing of the cheeks and vascular changes in their facial skin should be considered to have rosacea, he said; if they have blepharitis and MGD, at least part of that can be attributed to rosacea.
In rosacea patients, who principally have meibomianitis, the normal flora produce lipolytic enzymes that break down the lipid molecules into individual components, Dr. McCulley added. The main lipid components of the meibomian gland secretions are cholesterol ester and wax ester and, to a lesser extent, triglyceride.Staphylococci produce enzymes that break down all three, he explained.
Oral minocycline (Dynacin) appears to reverse this process by inhibiting these enzymes. In addition, minocycline, unlike other tetracycline analogues, kills the bacteria that produce the lipolytic enzymes. For example, minocycline eradicates S. aureus and decreases the colony count of S. epidermidis. “Of the tetracycline analogues, minocycline seems to be significantly superior,” Dr. McCulley said. The antibiotic also retards white-cell migration, Dr. Mathers said.
Treatment Decisions
Oral antibiotics. In anterior blepharitis, Dr. McCulley recommends minocycline only in cases of severe or recalcitrant staphylococcal involvement.
For patients with primary meibomianitis, Dr. McCulley treats with 50 milligrams a day of minocycline. If they tolerate that for two weeks, he increases it to 100 mg/day for a total of three months, and then stops it. “We used to keep these patients on low-dose tetracycline analogues for an indefinite period. Minocycline, however, keeps the ocular component of their disease under control for at least three months after stopping treatment,” he said.
How long? “I don’t know, but it will not last forever,” Dr. McCulley said. “I retreat as necessary.”
Topical antibiotics. If Dr. McCulley suspects direct bacterial involvement or bacterial lipases breaking down the lipids, he has patients apply a topical antibiotic, preferentially bacitracin or fluoroquinolone ointment (Ciloxin), for one month as necessary. “The sulfonamides and erythromycin have extremely high resistant rates, so I don’t use them anymore,” he noted.
When the lids are very inflamed, topical antibiotics can help to decrease the bacterial load in the short term, but Dr. Mathers noted that resistance does develop. “Long-term topical antibiotics are not terribly effective,” he said. If long-term topical antibiotics are indicated, Dr. McCulley alternates two different antibiotics on a weekly basis.
In addition, patients with chronic blepharitis often have a dermatological abnormality, either seborrheic dermatitis or rosacea, he said, and appropriate therapy to control the broader disease also benefits the eye.
Basic hygiene. For both anterior and posterior blepharitis, Dr. McCulley recommends local mechanical hygienic maneuvers, including warm compresses for five to 10 minutes. If patients have evidence of meibomian gland involvement, he has them massage their lids to express the lipids, followed by lid scrubs with either a baby shampoo or a commercial lid scrub. Patients should do this once or twice a day. “Many of my patients stay pretty clear as long as they keep doing this. When they fall off the wagon, signs and symptoms come back,” Dr. McCulley said.
Don’t Forget Dry Eye
Don’t forget to treat the dry eye in blepharitis patients. Dr. Mathers treats both conditions with nonpreserved artificial tears as well as low-penetrating steroids and topical cyclosporine (Restasis). He also prescribes flaxseed oil or fish oil, about 6 grams a day, to provide omega-3 fatty acids and for its anti-inflammatory effect.
Both dry eye and blepharitis are inflammatory processes. If inflammation has started to contribute to the expression of disease, anti-inflammatories may be of benefit. However, Dr. McCulley does not recommend topical steroids or NSAIDs. “I stay away from topical steroids, even the milder steroids. I’ve seen enough patients with bad opportunistic infections. Steroids may let the normal flora overgrow and let opportunistic bacteria or fungi flourish on the ocular surface,” he said.
“It is better to treat the mechanisms leading to the expression of disease rather than trying to dampen the inflammation reaction,” he added. “Often, the other measures will work.”
______________________________
Dr. Mathers is a consultant for Bio-Logic Aqua Technologies. Dr. McCulley’s research is supported by an NIH grant.
Describing the Disease
Anterior. This includes seborrheic blepharitis and that caused by staphylococcal overgrowth.
Posterior. This includes patients with meibomian gland involvement, from excessive meibomian secretions (meibomian seborrhea) to primary meibomianitis (as in patients with rosacea) or secondary meibomianitis (with acute inflammatory episodes of the meibomian glands).
Obstructive. In obstructive MGD, lipid volume is decreased. The orifices of the meibomian gland keratinize—that is, the gland secretions back up, thicken and clog, leading to inflammation, Dr. Mathers explained.
Eventually, these glands get absorbed. “Under transillumination, you can see that the glands are missing,” he said. “A lot of gland dropout indicates that the meibomian gland problem is relatively severe.”
Nonobstructive. In seborrheic blepharitis and seborrheic MGD, the meibomian glands are not blocked. The oil is somewhat thickened but still liquid. “It flows all over the place,” Dr. Mathers said. “The increased lipid production and inflammation leads to a chronic irritation.”
|