Download PDF
The published evidence fails to support the use of topical nonsteroidal anti-inflammatory drugs (NSAIDs) for long-term benefit in visual acuity outcome after routine cataract surgery, an Academy Ophthalmic Technology Assessment (OTA) has concluded.
The authors reported that, although topical NSAIDs appear to offer short-term benefits, there was no conclusive evidence that the drugs led to better visual outcomes at 3 months or more after surgery.1
“The goal of an OTA is always to try to objectively analyze the literature and determine what constitutes best evidence,” said study coauthor Stephen J. Kim, MD, associate professor of ophthalmology and visual sciences at Vanderbilt University, in Nashville, Tenn.
“Visual acuity over the long term is ultimately the most important outcome of cataract surgery, and our analysis of the literature indicates that there’s no conclusive evidence of a long-term benefit with routine NSAID use in cataract surgery,” Dr. Kim said.
Methods. The authors reviewed 15 studies that they deemed to have a sound methodologic design and sufficient sample size. Ten were randomized controlled trials comparing CME incidence after use of prophylactic corticosteroids alone to NSAIDs alone or together with corticosteroids. Six of the controlled studies met the requirements for producing level I evidence and 4 for level II. Among the limitations identified by the OTA panel, the studies
- Often differed in their definition of CME and in how it was measured (angiography versus optical coherence tomography).
- Lacked sufficient sensitivity in assessing functional visual acuity.
- Sometimes compared the NSAID-treated eyes to those treated with a corticosteroid with poor corneal penetration or that were inadequately dosed.
- Did not support claims of a synergistic effect from combining a corticosteroid and an NSAID.
Dr. Kim emphasized that the panel limited its assessment to routine cataract procedures and did not evaluate short-term visual outcomes. “The OTA’s findings apply to those patients who have no risk factors and relatively healthy eyes, who are undergoing routine cataract surgery,” he said.
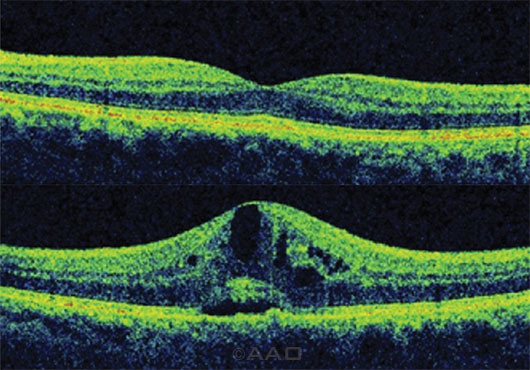 |
BEFORE AND AFTER. Clinically important cystoid macular edema pre– and post–cataract surgery.
|
In the clinic. Because many cataract surgeons already prescribe NSAID eyedrops for all patients, this OTA might face challenges in clinical acceptance, Dr. Kim said. “This runs against common practice for the majority of cataract surgeons, so it may be controversial.” He noted that during a wide review process to gain input for the OTA, one group provided feedback that the majority of their members routinely prescribed NSAIDs and felt they had a benefit for patients.
The OTA acknowledges that in routine cases, the topical application of an NSAID for 3 days before surgery reduces CME and improves early visual acuity.
“Patient satisfaction in the short term and faster recovery time in the window of the first 4 weeks may have value in certain patients, and we do acknowledge that in our report,” Dr. Kim said. “But there is no conclusive evidence that this practice affects long-term visual outcomes.”
—Linda Roach
___________________________
1 Kim SJ et al. Ophthalmology. June 2, 2015 [Epub ahead of print].
___________________________
Relevant financial disclosures—Dr. Kim: None.
For full disclosures and disclosure key, see below.
More from this month’s News in Review