By Rebecca Taylor, Contributing Writer, interviewing James Chodosh, MD, MPH; Gary N. Holland, MD; Anna Wald, MD, MPH; and Steven Yeh, MD
Download PDF
By its very nature, a global pandemic demands innovative approaches to vaccine research, data analysis, and production. With COVID-19, interim data analysis has become the norm, since vaccine developers and purchasers have needed to make strategic, life-saving decisions as quickly—and as safely—as possible.
The Johnson & Johnson/Janssen and Oxford/AstraZeneca vaccines—both of which involve viral-vector platforms—have emerged as the leaders of the second wave of vaccines. And they have a lot to live up to: The mRNA vaccines from Pfizer and Moderna reported impressive phase 3 data of 95% and 94.5% efficacy, respectively (see “COVID-19 and Novel mRNA Vaccines,” April EyeNet).
How do these viral-vector vaccines fit into the pandemic landscape? Four experts provide an overview of these newer options and discuss the issues they face.
New Vaccines, New Challenges
The rollout of these two viral-vector vaccines is taking place amid myriad challenges, including the emergence of SARS-CoV-2 variants and observed side effects.
Concern over variants. Vaccine developers have had to contend with changing prevalence of variants and a lack of widespread genomic testing to know where and how SARS-CoV-2 is mutating. In essence, while the first mRNA trials could aim directly at the original virus, the newer vaccines are facing a Russian roulette of mutations as the virus evolves.
“The variant coming out of South Africa is a concern because it has shown reduced efficacy of the vaccines for that particular set of mutations,” said James Chodosh, MD, MPH, at Harvard and Massachusetts Eye and Ear in Boston. “The specific amino acids that bind to the angiotensin-converting enzyme 2 receptor and those that form epitopes for immune recognition are not necessarily the same, so there are opportunities for the spike protein to evolve and evade the immune system, without dramatically reducing its ability to cause an infection.”
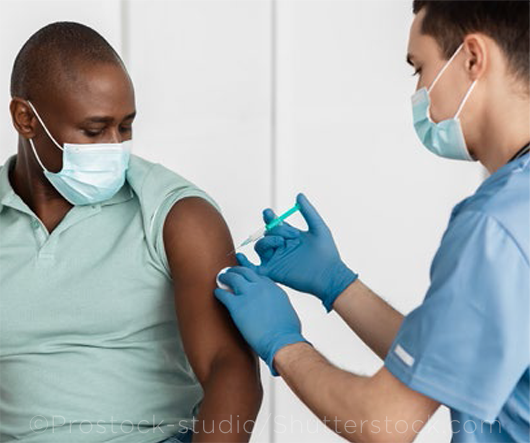
Concern over side effects. In April, the United Kingdom and European Union countries found themselves scrambling to address safety concerns when the European Medicines Agency (EMA) issued a statement linking the AstraZeneca vaccine to blood clots in a small percentage of recipients.1 And in the United States, similar reports of blood clots led to a mandated pause in the administration of the Johnson & Johnson vaccine.
 |
|
BUMPY ROAD. The newer vaccines have been hamstrung by ongoing reports of side effects, particularly clotting.
|
Johnson & Johnson Vaccine: An Overview
In January, The New England Journal of Medicine reported interim results of Johnson & Johnson’s phase 1/2a trial in the United States and Belgium, comparing combinations of low/high doses and single/double doses of their vaccine. The vaccine, Ad.26.COV2.S (also known as Ad26), uses adenovirus 26 as its vector.2
“Relatively few people have been infected with Ad26, whether you look at the United States or sub-Saharan Africa,” said Dr. Chodosh. “You want to make sure there aren’t preexisting antibodies to the adenovirus you use to deliver the spike protein.”
Phase 1/2a results on safety and immunogenicity. In initial trials, the vaccine showed spike-binding and neutralizing-antibody effects in at least 90% of trial participants on day 29 after dose 1, and in 100% by day 57. These immune responses stabilized and increased during 71 days of follow-up. Based on such positive findings, Johnson & Johnson launched two phase 3 trials, including ENSEMBLE 1, to test its single-dose protocol.3
Phase 3 efficacy. Johnson & Johnson submitted early single-dose data to a special FDA meeting on Feb. 26, 2021, as part of its application for emergency use authorization (EUA). The EUA was granted on Feb. 27,4 and the first doses were administered publicly in early March.
Across all countries in the trial, 28 days after injection, a single dose showed 66.1% efficacy against moderate/severe disease, 85.4% efficacy against severe/critical disease, and 100% efficacy against hospitalizations and deaths. Regionally, the vaccine had 85.9% efficacy against severe/critical disease in the United States and 81.7% against severe/critical disease in South Africa, where an estimated 90% of cases are caused by the South African variant.5
Community rollout. In March, Johnson & Johnson teamed up with Merck to accelerate vaccine production. And the “one and done” vaccine offers hope for more equitable access to COVID-19 vaccines in low-resourced communities. “I’ve always been enthusiastic about a single-dose vaccine because it’s more important to provide—maybe not 95% immunity but 70% to 80%—immunity to twice as many people, with potential for later boosts,” said Anna Wald, MD, MPH, at the University of Washington School of Medicine in Seattle.
However, hopes of a smooth rollout in the United States were dampened by quality-control problems at a Baltimore facility—and by the blood clotting concerns. But after a safety review, the FDA and CDC gave the go-ahead for the administration of the vaccine to be restarted.6
In the Clinic: Masking Protocols
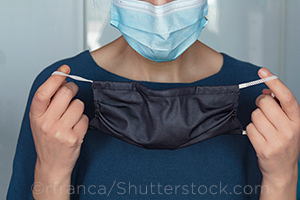
“Ophthalmologists are among the higher risk providers because of our proximity to patients during exams,” said Steven Yeh, MD, at the University of Nebraska in Omaha. “We’re examining patients with COVID-19 as well as those with unknown status, so it’s critical to continue our masking, distancing, and disinfection protocols as we move through the pandemic.”
CDC update. Results from aerosol and filtration studies published earlier this year by the CDC show just how critical masking strategies can be. Wearing a procedure mask alone intercepted 42% of cough particles, while a cloth mask alone intercepted 44.3%.1 But two new strategies decreased exposure to aerosols by roughly 95% when the “source” and “receiver” of aerosols used both:
- Double mask. Wear a cloth mask over a procedure mask.
- Knot and tuck. Knot the loops of a procedure mask close to the cloth, and tuck in folds for a closer fit to skin.
“As CDC guidelines evolve, they may differ for public and private settings, but hospitals and clinics still need to enforce infection control policies of masking and physical distancing,” said Dr. Holland. “For now, even fully vaccinated patients still need to wear masks in the clinic and adhere to workplace requirements.”
__________________________
1 Brooks JT et al. MMWR. 2021;70(7):254-257.
|
AstraZeneca Vaccine: An Overview
AstraZeneca’s vaccine story highlights the immense challenges of research during a global pandemic. The vaccine (Vaxzevria; formerly known as AZD1222) uses a nonreplicating chimp adenovirus to ferry genetic code for the SARS-CoV-2 spike protein into human cells. The Lancet published data from four ongoing trials on Dec. 8, 2020, with corrections on Jan. 7, 2021.7
Variable study designs. Interim efficacy data came from the phase 2/3 COV002 and the phase 3 COV003 studies, while safety data came from those two trials plus two phase 1/2 studies: COV001 and COV005.
COV001, conducted in the United Kingdom, excluded participants with preexisting conditions and began as a one-dose protocol, switching to two doses after seeing a booster effect in early data. COV002, which also took place in the United Kingdom, had issues with batch control and inadvertently tested some participants with low doses. “I wonder if the fact that they made a dosing error in their clinical trial might reduce confidence in the vaccine,” said Dr. Chodosh.
COV003, conducted in Brazil, targeted high-risk patients and included those with stable preexisting conditions. COV005, which took place in South Africa, included a cohort with HIV but didn’t report that data in its interim analysis. Across all sites, second-dose timing varied from six to 12 weeks.
“For AstraZeneca, the results published from the three countries are confusing,” said Dr. Wald. “It’s difficult to tease apart the components of dose and population, which differed in these studies, so I don’t really know how effective it is; I’m waiting for data from the U.S. trial to comment fully.”
Pooled efficacy data. Given the pandemic’s urgency, the vaccine was approved by the EMA and other regulators, despite AstraZeneca’s approach of combining data from four trials in different phases. This pooled data analysis reported 62.1% efficacy in preventing COVID-19 after two standard doses, 90.0% efficacy after a low-dose/standard-dose protocol, and overall efficacy across both groups of 70.4%.7
Community rollout. In February, South Africa created a stir when it paused distribution of the AstraZeneca vaccine following efficacy concerns with the country’s regional variant.8 However, the World Health Organization (WHO) issued recommendations to keep providing the vaccine after WHO scientists determined that, given the ongoing burden of disease in the United Kingdom and South Africa, its use was justified.9
In April, this back-and-forth was further complicated by additional reports of blood clots in the United Kingdom10 as well as by myriad problems linked to the developing crisis in India, notably the infectivity rate.
Looking Ahead
Measuring antibodies. Vaccine trials—and news outlets—have reported spike-binding and neutralizing antibody responses, but how significant are these data?
“Binding does not necessarily mean neutralizing,” said Dr. Chodosh. “Neutralization, tested in functional studies, means that you’ve blocked infectivity.” And Dr. Wald noted, “COVID vaccines, so far, have resulted in both high binding and neutralizing antibodies, but binding data don’t tell you anything about functional effects. Companies can talk about their laboratory data, but it’s meaningless because the immune correlate of protection has not yet been established.”
So why all the focus on spike binding? “The vaccines are made to elicit antibodies to the spike protein, so that’s what people are measuring, as a shorthand, because neutralizing antibodies are much more difficult to measure,” said Dr. Wald.
Road to full licensure. The FDA still requires a two-year follow-up with adverse events data before it will grant any of the new vaccines full licensure. “What the FDA does, which is unique, is not just look at the data submitted by the pharmaceutical company,” said Dr. Wald. “It does a very thorough job of independently analyzing the dataset.”
Viral mutations and booster shots. Many viruses mutate; the trick is knowing which resulting variants of SARS-CoV-2 increase its transmissibility and lethality. “It’s critical to vaccinate as many people as possible to slow the spread of virus,” said Gary N. Holland, MD, at the University of California, Los Angeles. “If the virus continues to reproduce at current rates, new, even more dangerous mutations may emerge.”
What might this mean for people who have already been vaccinated? “It’s worrisome,” Dr. Chodosh said. “To what degree will the FDA provide emergency use authorization this fall for Moderna and Pfizer vaccines that have been modified with a more diverse set of mRNAs chosen to reflect the variants circulating?”
Research targets. Profound advances in immunology and chronic disease may be this era’s one silver lining. In February, the NIH announced a new initiative aimed at fostering research on the spectrum of recovery following COVID and the underlying biology of prolonged symptoms.11 “COVID ‘long-haulers’ are going to teach us a lot about infection, autoimmunity, trained immunity, and how our tissues and chromosomes respond to severe inflammation that is widespread and persistent,” Dr. Chodosh said. “The entire body is affected with inflammation by COVID, with the equivalent now of post-COVID chronic fatigue.”
With regard to antibody data, Dr. Wald said, “The next thing for us to understand is how much antibody you need to be protected, and this could be expressed as either a binding or a neutralizing antibody.”
And yet more innovative approaches to this novel virus may appear in the future. “The spike protein is what’s mutating, so are there other components of the virus that cannot mutate as easily, because the virus needs them to survive?” Dr. Wald asked. “If we can make an immune response to those components, then we’ll have a more universal vaccine.”
__________________________
1 www.ema.europa.eu/en/news/astrazenecas-covid-19-vaccine-ema-finds-possible-link-very-rare-cases-unusual-blood-clots-low-blood. Accessed April 8, 2021.
2 Sadoff J et al. N Engl J Med. Published online Jan. 13, 2021.
3 www.clinicaltrials.gov; NCT04505722.
4 www.fda.gov/news-events/press-announcements/fda-issues-emergency-use-authorization-third-covid-19-vaccine. Accessed April 8, 2021.
5 www.fda.gov/media/146219/download. Accessed April 9, 2021.
6 www.fda.gov/news-events/fda-newsroom/press-announcements. Accessed April 29, 2021.
7 Voysey M et al. The Lancet. 2021;397(10269):99-111.
8 Cohen J. Science. 2021;371(6529):548-549.
9 www.who.int/news-room/feature-stories/detail/the-oxford-astrazeneca-covid-19-vaccine-what-you-need-to-know. Accessed April 8, 2021.
10 www.gov.uk/government/publications/coronavirus-covid-19-vaccine-adverse-reactions. Accessed April 29, 2021.
11 www.nih.gov/about-nih/who-we-are/nih-director/statements/nih-launches-new-initiative-study-long-covid. Accessed April 12, 2021.
__________________________
Dr. Chodosh is the Edith Ives Cogan Professor of Ophthalmology at Harvard Medical School and associate director of the Infectious Diseases Institute at Massachusetts Eye and Ear, Boston. Relevant financial disclosures: None.
Dr. Holland is professor of ophthalmology, the Jack H. Skirball Chair in Ocular Inflammatory Diseases, and director of the Department of Ophthalmology Clinical Research Center at the University of California, Los Angeles. Relevant financial disclosures: None.
Dr. Wald is head of the Division of Allergy and Infectious Diseases and professor in the departments of Medicine, Allergy and Infectious Diseases, Epidemiology, and Laboratory Medicine and Pathology at the University of Washington, Seattle. She is also professor in the Vaccine and Infectious Diseases Division at the Fred Hutchinson Cancer Research Center in Seattle. Relevant financial disclosures: None.
Dr. Yeh is the Stanley Truhlsen Jr. Chair in Ophthalmology and director of the retina and uveitis service at the University of Nebraska in Omaha. Relevant financial disclosures: None.
For full disclosures and the disclosure key, see below.
Full Financial Disclosures
Dr. Chodosh British Journal of Ophthalmology: E; FDA: C; NEI: S.
Dr. Holland Childhood Arthritis and Rheumatology Research Alliance: S; NEI: S; University of California Firearm Violence Research Center: S.
Dr. Wald NIH: S.
Dr. Yeh Santen: C.
Disclosure Category
|
Code
|
Description
|
| Consultant/Advisor |
C |
Consultant fee, paid advisory boards, or fees for attending a meeting. |
| Employee |
E |
Employed by a commercial company. |
| Speakers bureau |
L |
Lecture fees or honoraria, travel fees or reimbursements when speaking at the invitation of a commercial company. |
| Equity owner |
O |
Equity ownership/stock options in publicly or privately traded firms, excluding mutual funds. |
| Patents/Royalty |
P |
Patents and/or royalties for intellectual property. |
| Grant support |
S |
Grant support or other financial support to the investigator from all sources, including research support from government agencies (e.g., NIH), foundations, device manufacturers, and/or pharmaceutical companies. |
|