By Reena Mukamal, Contributing Writer, interviewing Deborah S. Jacobs, MD, Gerami D. Seitzman, MD, and Christine Shieh, MD
Download PDF
Demodex mites have been associated with multiple ocular conditions including chronic blepharitis, keratoconjunctivitis, chalazia, keratitis, endophthalmitis, and even periocular basal cell carcinoma.1 Although the small arthropods have long been considered a regular resident of normal skin, a debate among ophthalmologists is growing: Is Demodex simply a harmless bystander or can it also become a pathogen? Now, as the first targeted drug is about to take its place alongside numerous other therapies aimed at reducing or eliminating Demodex, this periocular parasite merits a closer look.
Mites That Grow on You
Two different types of Demodex mites live on the human body, Demodex folliculorum and Demodex brevis. Measuring 0.3-0.4 mm and 0.15-0.2 mm in length respectively, they are too small to see with the naked eye.
“They are an inhabitant of the skin’s normal microbiome; almost everyone has some Demodex,” said Gerami D. Seitzman, MD, at the University of California, San Francisco.
The mites spend much of their time burrowed head-down inside human hair follicles, gorging on dead skin cells and sebum. At night, they crawl out of the follicle to mate and lay their eggs. The mites have a life span of approximately two to three weeks.
 |
|
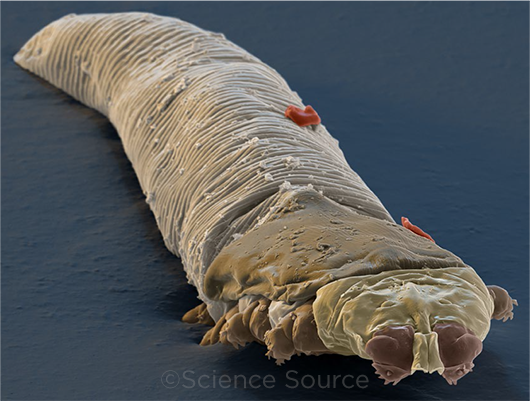
UP CLOSE. Colorized scanning electron micrograph of D. folliculorum.
|
Pervasive, But Not Always Pathogenic
Although the mites often live in a commensal relationship with humans, an overpopulation of Demodex mites is called demodicosis. A meta-analysis of dermatology studies correlated Demodex with rosacea.2
Associated with ocular conditions. A high density of the parasites in eyelash follicles has been associated with ocular rosacea and chronic blepharitis. Results of recent studies have suggested that anywhere from 42% to 81% of blepharitis patients have concomitant infestation with Demodex, and that the mites are more prevalent in older patients.3
“Demodex infestation has also been linked to blepharokeratoconjunctivitis, meibomian gland dysfunction, and chalazia, especially through the work of Dr. Scheffer Tseng and his collaborators,” said Christine Shieh, MD, at Vanderbilt Eye Institute in Nashville, Tennessee.
Questions remain. There is a lot of discussion among ophthalmologists about the exact role that Demodex may play in these eye conditions, including “what amount of Demodex population is normal,” said Deborah S. Jacobs, MD, at Harvard Medical School in Boston.
“Awareness that Demodex can be more than just a commensal organism is growing,” said Dr. Shieh. “However, some debate remains about the exact role of Demodex in blepharitis, since these mites also may be found in healthy, asymptomatic individuals,” she said.
Complicating the question is the chicken-and-egg-like origin of Demodex congestion, said Dr. Seitzman. “Does an inflammatory eye condition allow a normal amount of mites to proliferate to an abnormal amount? Or do the mites multiply out of control and induce an inflammatory eye condition? We’re still not clear which comes first.”
When to Suspect Demodex
If patients have red, swollen, sore, and itchy eyelids that are not responding to standard treatment, a Demodex overpopulation is worth investigation.
Signs and symptoms. “When a patient has chronic blepharitis or blepharokeratoconjunctivitis, this raises my suspicion of concurrent Demodex,” said Dr. Shieh, adding “Studies have also reported that eyelid itching in patients without a history of ocular or systemic allergy can be associated with Demodex.”
Dr. Seitzman adds difficult-to-control ocular rosacea and recurrent styes to the list of possible signs. “Lash loss and/or trichiasis can be additional clues that Demodex may be a culprit,” she said.
When Dr. Jacobs suspects Demodex, she looks for the presence of cylindrical sleeves at the base of the eyelid as signs of a potentially problematic Demodex infestation. When a high density of mites are proliferating on the eyelid, they cause skin inflammation at the base of the follicle, which creates a sleeve of cylindrical dandruff around the lash.
Insufficient relief. Often, patients with ongoing symptoms have tried conventional treatments for ocular surface disease without experiencing much improvement, said Dr. Seitzman. Chronic blepharitis symptoms can negatively impact a patient’s quality of life. And, according to Dr. Shieh, if it is left untreated, blepharokeratoconjunctivitis has the potential to lead to severe corneal complications and diminished vision.
Diagnosis With and Without a Microscope
External exam. A number of ophthalmologists believe Demodex may be overlooked in patients. This may be because exams tend to go “right to the eyeball” and may gloss over inspection of the eyelashes, where Demodex leave telltale signs, said Dr. Seitzman. “Every thorough external disease examination should start with the patient’s eyes closed and an exploration of eyelash health,” she said.
Visualization. The Demodex mite can be seen on confocal microscopy or on an epilated lash under a light microscope, said Dr. Shieh. According to Dr. Seitzman, mites grab tightly to the follicle, so swirling the lash before pulling helps facilitate successful epilation.
Slit-lamp exam. For ophthalmologists who don’t have a light or confocal microscope in the office, one study suggests that slit-lamp microscope techniques can also be used to confirm the mites, said Dr. Shieh.4 She recommends using the slit-lamp to zoom in to the base of the eyelashes along the patient’s closed upper eyelids.
Making the diagnosis. There is no consensus regarding the number of eyelashes that should be examined, the technique involved, and precisely what “mite density” is required to be pathogenic, and this is why most ophthalmologists will make a presumptive diagnosis by looking for the presence of cylindrical sleeves on lashes, said Dr. Jacobs. “Heavy cylindrical dandruff is considered a clinical sign of mite infestation, and even pathognomonic by some ophthalmologists,” said Dr. Shieh. However, it can easily be missed if you’re not looking for it.
Differentiate Demodex from Staphylococcus. “It’s also important to clinically differentiate lash debris caused by a Staphylococcus overgrowth—also referred to as a collarette—from a cylindrical sleeve, which is caused by Demodex. The former is a lacy bit of skin mixed with staphylococcus and can be indicative of a bacterial overgrowth. The latter is inflammatory skin protein mixed with mite debris that hugs tightly to the base of the eyelash. Patients can have either one or both together,” said Dr. Seitzman.
Patient embarrassment. It’s not uncommon for patients to feel uncomfortable after receiving a Demodex diagnosis. Reassuring them that these organisms are universal and that an overpopulation is not related to personal hygiene can help assuage feelings of embarrassment or shame. This in turn can help improve compliance, which is needed for successful treatment, said Dr. Jacobs.
Over-the-Counter Cleansers and Scrubs
Patients who have an abundance of sleeves but are asymptomatic likely do not need treatment for Demodex, said Dr. Seitzman.
For symptomatic patients, ophthalmologists may start treatment with a combination of topical over-the-counter (OTC) treatments to mechanically disrupt mite density. “I like to prescribe a tea tree oil or hypochlorous acid based scrub, spray, or cleansing wipe (i.e., Ocusoft, Oust, Optase, Cliradex) as a first-line treatment,” said Dr. Jacobs.
Tea tree oil. Terpinen-4-ol, a terpene with antimicrobial, antifungal, antiviral, antiseptic, and acaricidal properties, is the active ingredient in tea tree oil.5 Patients can use topical treatments one or two times per day for one to three months, but these therapies may be irritating to some eyes. “Keep in mind that 100% pure tea tree oil stings and is toxic to the corneal epithelium, so I recommend lower concentration doses in the range of 5% to 10%, applied daily or weekly, depending on the individual,” said Dr. Seitzman.
Dr. Jacobs noted that patients can buy products with low percentages of tea tree oil. “More and stronger may not be better,” she said.
In addition, said Dr. Seitzman, “A 50% tea tree oil solution can be applied in the office, often with topical anesthetic and a doctor-initiated lid scrub.”
Topical steroid. All three doctors said it can be helpful to prescribe a topical steroid in conjunction with OTC treatments to help reduce inflammation.
Ivermectin, Metronidazole, Doxycycline
To tackle stubborn ocular Demodex, ophthalmologists have used antiparasitic medications approved for the treatment of rosacea, taken individually or in combination.
Topical ivermectin. “I commonly use ivermectin ointment off label for patients with Demodex, and it works very well,” said Dr. Seitzman. Patients can expect a temporary increase in inflammation and discomfort in the first few days of treatment as a large volume of mites are killed. The ointment can be used as a bedtime lid scrub for one to two months, she said.
Now that topical ivermectin is available as a generic product, it is no longer prohibitively expensive for many patients, said Dr. Jacobs.
Oral ivermectin. The oral formulation of ivermectin is another effective and relatively economical option. Patients take one to three weight-based doses, spaced one week apart.
“Oral ivermectin may be more likely to reach deep follicle areas, but it wouldn’t result in debridement of cylindrical dandruff,” according to Dr. Seitzman. Patients would need to complement it with another agent to clean the eyelash margin.
Dr. Seitzman noted that the oral version of the drug may cause gastrointestinal discomfort, nausea, and diarrhea.
When choosing between topical and systemic agents, Dr. Jacobs favors a collaborative approach with each patient. “An elderly person taking a lot of medications may want to stay away from another pill, while someone who struggles to use a topical medicine nightly may be better off with the oral agent.”
Metronidazole. According to Dr. Shieh, some studies have shown that combining ivermectin and metronidazole can reduce mite count more than either drug alone. The combination can be administered in either topical or oral form.6,7
Doxycycline. Adult patients who suffer from concurrent skin rosacea may also benefit from taking doxycycline, said all three doctors. “However, the ideal treatment dose is not established and can range from an antibiotic dose to a submicrobial dose. Doxycycline may help address the inflammation of sebaceous glands, but it doesn’t attack Demodex itself, so I use it in combination with other therapies,” said Dr. Seitzman.
Follow-up. Keeping patients of any age on a consistent regimen can be a challenge. Dr. Jacobs likes to see patients back at the six-week mark to assess both symptoms and prevalence of sleeves. Maintenance therapy with topical and/or oral medications may be needed to keep flare-ups at bay.
On the Horizon: An FDA-Approved Treatment
A drug in phase 3 clinical trials might soon become the first FDA-approved treatment for Demodex blepharitis. TP-03 is a topical agent being tested by Tarsus Pharmaceuticals. The drug’s active ingredient is .25% lotilaner, an antiparasitic agent that works by inhibiting the mites’ nervous system GABA-CI channels. Phase 2/3 trial researchers reported that patients treated with TP-03 daily for four weeks had statistically significant reductions in mite numbers and lid erythema, and the treatment was well tolerated.8
“Paralyzing the nervous system of the mite is an intriguing mechanism,” said Dr. Shieh. Dr. Jacobs believes there is an unmet need for a targeted therapy. But, she noted, “the question is, will patients have access based on price and payer coverage?”
Dr. Seitzman added, “If this treatment does work, it would be a great contribution to a condition that is in need of other therapeutic modalities.”
___________________________
1 Sánchez España JC et al. Ophthalmology. 2016;123(12):2632-2633.
2 Chang Y-S et al. J Am Acad Dermatol. 2017;77(3):441-447.
3 Zhao Ya-E et al. Ophthalmic Epidemiol. 2012;19(2):95-102.
4 Man Peles I. et al. Cornea. 2020;39(7):858-861.
5 Tighe S et al. Transl Vis Sci Technol. 2013;2(7):2.
6 Ávila MY et al. Cont Lens Anterior Eye. 2021;44(3):101326.
7 Salem DA-B et al. Int J Infect Dis. 2013;17(5):343-347.
8 Salinas RG et al. Cont Lens Anterior Eye. 2021;101492.
___________________________
Dr. Jacobs is an associate professor of ophthalmology at Harvard Medical School in Boston. Financial disclosures: Simple Contacts: C,O; TecLens: C,O; UpToDate: P.
Dr. Seitzman is a cornea and external disease specialist at University of California, San Francisco. Financial disclosures: Dompé: C.
Dr. Shieh is a cornea and external disease specialist at Vanderbilt Eye Institute in Nashville. Financial disclosures: None.
See the disclosure key at www.aao.org/eyenet/disclosures.