Dislocation of Hypermature Cataract
By Homer H. Chiang, MS, and Jonathan D. Paul, MD, University of Vermont College of Medicine, Burlington
Photo by Susana Teixeira, Hospital Prof. Fernando da Fonseca E.P.E., Lisbon, Portugal
Download PDF
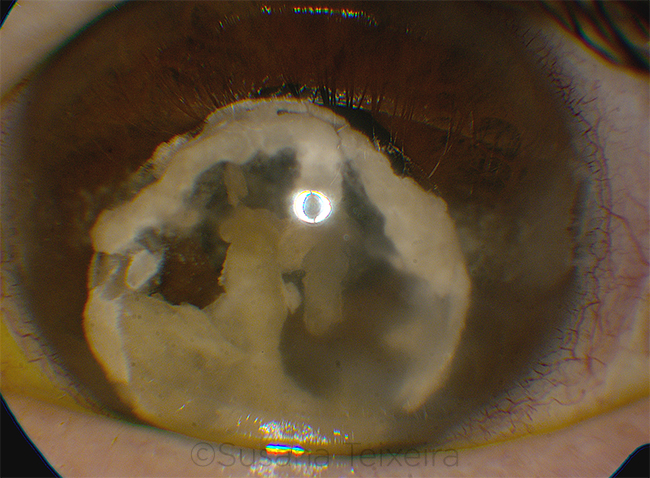
A 46-year-old man presented to the emergency room after a family member noticed a white discoloration in his left eye. He denied pain but reported a pressure sensation in the eye. He indicated that he had been “head banging” at a concert the night before. His past ophthalmic history by his own report was significant for retinal detachment in the left eye in childhood, with no light perception (NLP) since he had been treated with laser at the age of 5. No records were available.
Examination of the left eye revealed a prephthisical eye with band keratopathy of the cornea. Intraocular pressure was 7 mm Hg, and vision was NLP. There was complete dislocation of a hypermature cataract into the anterior chamber. The lens nucleus appeared to be absent. Lens material in the anterior chamber appeared to consist of fragments of opacified cortex with an intact capsule. No cell or vitreous was apparent in the anterior chamber. Funduscopy of the left eye was not possible. B-scan ultrasound showed an anteriorly dislocated lens and a retinal detachment. Examination of the right eye was unremarkable.
Options, including observation and dilating and repositioning, were discussed with the patient. He elected lensectomy to prevent corneal decompensation.
The patient was started on 2% pilocarpine to trap the lens in the anterior chamber. Lensectomy with anterior vitrectomy was performed through a clear corneal incision. Because the calcified cortical material could not be removed with coaxial irrigation/aspiration or the anterior vitrector, it was removed manually with forceps. The patient did well postoperatively without complication and remains NLP.
| BLINK SUBMISSIONS: Send us your ophthalmic image and its explanation in 150-250 words. E-mail to eyenet@aao.org, fax to 415-561-8575, or mail to EyeNet Magazine, 655 Beach Street, San Francisco, CA 94109. Please note that EyeNet reserves the right to edit Blink submissions. |