Do Normal Eyes Follow the ISNT Rule?
By Lynda Seminara
Selected By: Richard K. Parrish II, MD
Journal Highlights
American Journal of Ophthalmology, January 2018
Download PDF
Neuroretinal rim loss and thinning of the retinal nerve fiber layer (RNFL) are hallmark features of glaucoma. As a result, eyes that deviate from the ISNT rule may need close monitoring for glaucoma—but research findings on the utility of this rule for establishing glaucoma are conflicting. Poon et al. sought to determine the percentage of normal eyes that follow the ISNT rule and found that, contrary to traditional teaching, the rule applies to less than 45% of rim assessments and RNFL measurements.
The authors’ cross-sectional study included 110 normal eyes (110 participants). Neuroretinal rim assessments were made from disc photographs, and measurements of RNFL thickness were obtained from spectral-domain optical coherence tomography. The main outcomes were the percentages of eyes that obeyed the ISNT rule and its variants.
The researchers found that the ISNT rule was valid for only 37% of rim assessments and 43.8% of RNFL measurements.
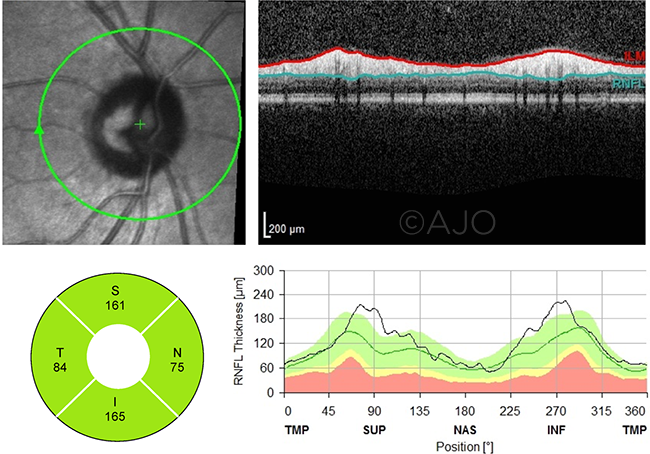 |
EXCEPTION TO THE ISNT RULE. In this example, the RNFL thickness (bottom left) in the nasal quadrant is thinner than the temporal quadrant. This violates the ISNT rule, which holds that the inferior (I) rim is the widest, followed in turn by the superior (S), nasal (N), and temporal (T) rims.
|
For both types of assessments, variance of the nasal sector from the expected ISNT pattern was a major reason for deviation. Nasal rims were wider than inferior rims in 11% of subjects and wider than superior rims in 29%. Nasal rims were narrower than temporal rims in 15%. RNFL thickness was greater in the nasal quadrant than the temporal quadrant in 43%. Exclusion of the nasal quadrant from the ISNT rule significantly increased validity of the ISNT variants: 71% and 76% of disc photographs followed the IST rule and the IS rule, respectively. For RNFL thickness, 71% and 72% coincided with IST and IS rules, respectively.
As a result of these findings, the authors advocate use of IST and IS rules for distinguishing glaucomatous from nonglaucomatous eyes.
The original article can be found here.