Download PDF
Apparently, 30,000 years of cooperative evolution between canids and hominids did not anticipate every incident between toddlers and terriers. “Violent encounters between kids and dogs have produced some of the worst trauma I’ve ever seen,” said Michael J. Hawes, MD, at the University of Colorado in Denver. “In an ideal world, very young kids would not even have dogs, especially the larger breeds like rottweilers and shepherds.” In fact, since 1989 the city of Denver has actually banned one breed—pit bull terriers—because of the daunting incidence of pit bull–related trauma.
But encounters involving many dog breeds persist all over the country, Dr. Hawes said, with perpetrators typically being nonneutered males under 5 years of age and weighing over 50 pounds.
Vikram D. Durairaj, MD, also at the University of Colorado, studied 537 pediatric patients with facial dog bites during a five-year period at the Children’s Hospital of Denver. “The average age of pediatric dog bite patients with ophthalmic involvement is 3 years,” said Dr. Durairaj. He said that these injuries are often severe. In another review of pediatric dog attacks, 17 of 1,201 children sustained injuries beyond canalicular and eyelid lacerations—including wounds to the facial nerve and fractures of the skull, nasal bone, zygomatic arch, orbital rim, orbital floor, mandible, and maxilla.1
In the United States, 4.7 million people are bitten by dogs every year, many of them children. In fact, 1 percent of all ER visits are related to dog bites. This is a significant problem for already busy ERs, and it’s important that ophthalmologists know how to handle these cases.
 |
|
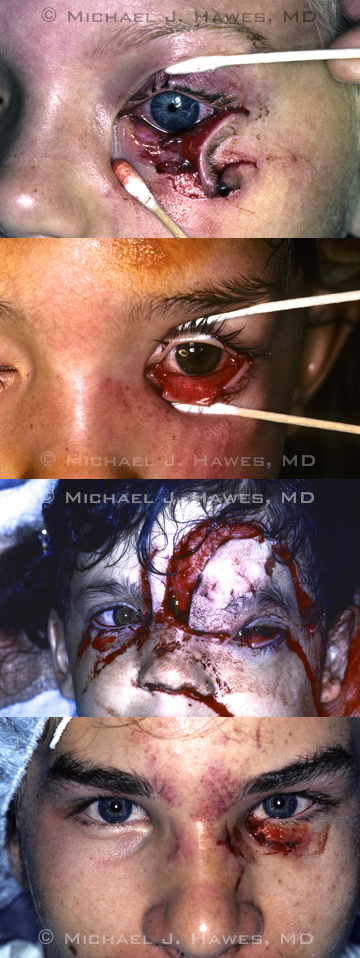
Four of Dr. Hawes' dog bite trauma patients.
|
Presentation in the ER
Although every dog bite attack is unique, these patients tend to have certain commonalities.
Victims. In Dr. Hawes’ experience, the victims of dog bites are usually children. “But even adults can present with serious bites,” he said.
John B. Holds, MD, at St. Louis University, has been confronted with a similar range of dog attack cases. “Most of my patients have been kids, although one of the worst injuries I’ve seen was an adult woman who bent over to pet a sleeping dog, which then spun around and latched onto her face and hung on, avulsing her entire upper and lower eyelids, her cheek and nose, and some of the nasal bone. We managed to put her back together, with minimal scarring.”
Evolution to the rescue. The range of motion of the canine bite is an efficient design for seizing the appendages of its prey, but it is brought up short by the structure of the orbital rim, behind which the globe enjoys a recessed security. “The orbital geometry that leaves a basketball unable to reach the globe is the same that stops a large dog jaw from harming a globe,” said Dr. Holds.
Consistent with that, Dr. Durairaj discovered that in his cohort of 537 dog bites, only one child suffered globe injury, and that was a partial-thickness corneal laceration.
Lids and lacrimals at risk. Dr. Durairaj noted that when it comes to dog bites in children, virtually 100 percent of the cases that an ophthalmologist would encounter involve the ocular adnexa. Dr. Hawes and Dr. Holds note that the preponderance of injuries they see among pediatric dog bite victims are to the lacrimal system. “I’ve never seen an open-globe injury related to dog bites,” said Dr. Holds. “Canalicular injuries are the ones we see most frequently, since the lacrimal drainage system is so easily injured by lateral traction from the dog’s teeth. Sometimes even mild pressure by the dog’s mouth can tear the canaliculus close to the punctum—it pulls and torques and produces avulsion to the soft medial or lateral canthus tissues.”
Eyelids and the canalicular drainage systems can be decimated, Dr. Holds said. “And on presentation, these eyes can look awful. Sometimes much of the tissue appears to be substantially lost. But, amazingly, the tissue is usually all there; it has just been torn and rearranged. And if you carefully salvage the fragments, you can almost always reassemble them.”
 |
|
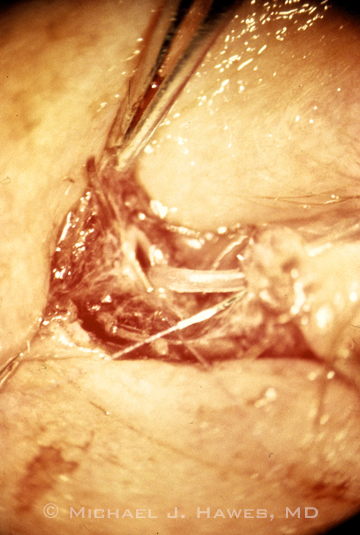
A cut canaliculus with tubing in it, taken through an operating microscope.
|
From the ER to the OR
Dr. Holds has encountered trauma so severe that he had to fall back on the “ABCs” of ER medicine: Airway, Breathing, and Circulation. “We had to transfuse one infant before she even went to the OR because she had lost so much blood from the dog attack. A child’s blood volume is small compared with an adult. If there is any question, hemodynamic stability must be assessed before considering repair.”
After stabilizing the patient, Dr. Hawes said that establishing the extent of the trauma and the need for repair can be managed with five steps:
- Irrigate the area copiously with saline.
- Initiate antibiotics and pain relief.
- Find out if the dog has been vaccinated against rabies.
- Report the attack to public health.
- Proceed with primary repairs.
Irrigation and antimicrobials. “Canalicular or lid lacerations call for cleaning meticulously with saline solution,” Dr. Holds said. After that, he considers how “dirty” the wound is. With dog bites, he added, “We want to act aggressively against infection. What I have used most commonly is amoxicillin with clavulanate [Augmentin] orally, or ampicillin with sulbactam [Unasyn] intravenously.”
Rabies alert. Ask the parents whether the dog was feral or familiar and report the dog attack to the public health department. The dog may be quarantined to determine whether it has rabies, and it could be euthanized.
Between the ER and the OR. Usually, and understandably, kids are hysterical after the dog bite experience. “Many of these are 7- or 8-year-old boys, and these little guys are unlikely to allow you to fool around with their eye while they’re awake, at least without some relief. You can begin with some anesthesia like midazolam if they are really upset,” said Dr. Holds.
In the OR. The season of dog bites—June and July are the most prevalent months—overlaps with the season most common for gun injuries and stab wounds, Dr. Holds said. That makes for competition for limited operating room space. But all three experts agreed that the best chance for success is in the OR. “Even though we try to do as much as we can in the clinic, it’s hard or impossible to repair serious oculoplastic injuries in a traumatized child without surgical loupes, an effective anesthetic, and the right lacrimal intubation set. But with all that at hand—in the OR—your success rate for primary repair of a canalicular laceration should be 95 percent,” said Dr. Holds. Being in the OR is important for another reason, he said. “If there are other complications—sometimes a dog bite to the face can even involve fractures—you might need help.”
Dr. Durairaj noted that aggressive repair in the OR may improve outcomes. “A complete ophthalmic examination and precise reconstruction of the lacrimal system and eyelids can be performed with the best chance of success when the patient is under general anesthesia in the controlled setting of the operating room.”
The surgery. For primary repair, Dr. Hawes begins reapproximating and suturing the torn tissues. “For closing up these canalicular lacerations, start with finding the cut end of the canaliculus—which you can almost always find just by looking for it. There are clues, and adjacent to the caruncle is a good place to look for the lost distal end of the canaliculus. It will look like a white tissue with rolled edges. Once you find it, pass a probe through the punctum to the proximal cut end of the canaliculus.”
Proceed into the lacrimal sac down the nasolacrimal duct and into the nose, using bicanalicular intubation, Dr. Hawes said. “Then sew the canaliculus together back over the tubing, using 7-0 vicryl absorbable sutures with a small half-circle spatula needle. The absorbable sutures and small needles minimize added trauma to the lids. Two or three sutures are sufficient, and there is no need to go through the canaliculus; you can go around the adjacent tissue and have a high success rate of patency.”
Dr. Durairaj considers a monocanalicular stent in some situations. “If there is damage to the canalicular system in the setting of an intact punctum, I will often use a monocanalicular stent anchored in the punctum. Stent placement is very straightforward and removal in the office is easily accomplished,” he said.
Dr. Holds added that deep sutures can be a reservoir for infection, so use the minimum, he advised, and use tiny sutures for typical repairs of the canthal tendon area or the tarsus. “I’ll also try to use dissolving sutures, since on kids it can be added trauma to get sutures out.”
Complications. If no tissue is missing, scarring typically involves only the tear duct or a droopy lid or canthal deformity, said Dr. Hawes. “The case with devitalized tissue is different, of course. But in general, facial and ocular tissues are very well supplied with blood, so we don’t typically see huge amounts of necrosis. I remember one time the parents brought in a kid with most of his lid missing. I asked them to go back and look carefully for any tissue left around. They found some on the kitchen floor and brought it back wrapped in a Kleenex! I used it—but there was some deformity resulting. I always tell the family to bring all body parts along with you to the ER—bring along whatever you can find!”
Dr. Holds agreed. “Even when the pieces are all there it can be quite a challenge. Make sure no tissue is devitalized.” On the other hand, Dr. Durairaj said that even in the setting of severe trauma, rarely does the surgeon need to remove any tissue.
Grafts. Sometimes Dr. Holds has to borrow tissue from elsewhere for a primary skin graft. “But because of the potential for graft infection, we do an advancement flap when possible, or place dressings and return for a secondary repair with a graft after five to seven days, when the risk of infection has been lessened. Dog bite infections are generally very rapid in progression. Typically, oral Augmentin [amoxicillin with clavulanate] is effective, along with IV Unasyn [ampicillin]. But the first attempt at repair is definitely the best shot. With kids in an amblyogenic age range—under age 6, you may have to place a frontalis sling to elevate the lid.”
___________________________
1 Wei LA et al. Ophthal Plast Reconstr Surg. 2013;29(3):179-182.
___________________________
Vikram D. Durairaj, MD, is professor of ophthalmology and otolaryngology/head and neck surgery at the University of Colorado, Denver. Financial disclosure: None.
Michael J. Hawes, MD, is clinical professor of ophthalmology at the University of Colorado in Denver. Financial disclosure: None.
John B. Holds, MD, is clinical professor of ophthalmology and otolaryngology/head and neck surgery at Saint Louis University, Missouri. Financial disclosure: None.