By Andrew D. Hsia, MD and Alla Y. Hynes, MD
Edited by Thomas A. Oetting, MD
This article is from May 2008 and may contain outdated material.
Stacy Moore,* a 45-year-old African American woman, was clearly distressed: “Doctor, I really hope you can tell me what’s going on. I’ve been told my facial droop is everything from a simple case of mumps to a stroke.” She had presented to the ER with a left facial droop, “cobwebs” and blurriness in her right eye for one week. She also reported malaise, dizziness and a macular skin rash on both of her lower legs.
Early Diagnoses
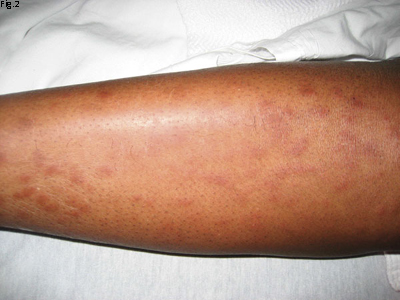
Two months earlier, Ms. Moore had presented to the ER with swollen parotid glands bilaterally and was told that she had a parotiditis secondary to mumps. She subsequently developed shortness of breath, and her primary care doctor referred her to a cardiologist. Ms. Moore underwent a transthoracic echocardiogram, which revealed a mild pericardial effusion. A week later, her shortness of breath improved, but she noticed a left facial droop (Fig. 1) and the skin rash over her lower legs (Fig. 2), sparing the soles of her feet (nor was there any rash on the palms of her hands).
The patient did not recall ever having a tick bite, but did often walk through tall grass. Furthermore, she had noticed a mosquito bite on the back of her neck around two months previously.
On review of systems, she noted intermittent joint pain, a mild fever and cobweb floaters. Her past ocular history was significant for blurriness two years previously, but she had not experienced any pain or photophobia.
She saw an ophthalmologist and was diagnosed with granulomatous uveitis, but her workup (including ACE, Lyme antibodies, RPR, PPD and chest x-ray) was negative. She was given steroid drops for two weeks and did not have any blurriness until the last week.
Neurology Gets a Look
When Ms. Moore returned to the ER this second time, she was seen by neurology. A CT scan of her brain and then a lumbar tap were performed. The CT scan was normal, but her CSF showed an elevated cell count (20 cells/mm3), with lymphocytes (82 percent), and elevated protein (116 mg/dl) and glucose (46 mg/dl). Although she did not have nuchal rigidity and her CBC with differential was normal, neurology suspected that she had a viral meningitis, or perhaps a Lyme infection based on her CSF and her symptoms.
 |
|
Paralysis. She had a left facial palsy.
|
The Physical Exam
Ms. Moore was alert and oriented, and her vital signs were stable. Cardiovascular and pulmonary exams were normal. The neurologic exam showed a left facial palsy with weakness and inability to close her left eye and mouth. The rest of her exam, including cranial nerve exam, was normal. Her UCVA was 20/50 in both eyes and her BCVA was the same. She had an IOP of 11 mmHg in both eyes. There was no anisocoria, and she had no relative afferent pupillary defect in either eye. Visual fields and motility were also normal.
In the right eye, the slit-lamp examination showed 1+ conjunctiva injection with white nongranulomatous keratitic precipitates on the cornea. The right eye also had 3+ cell and haze in the anterior chamber, posterior synechiae and 3+ vitreous haze and vitreous debris. There was a poor view of the retina, but no sheathing or snowballs were seen. The left eye showed 1+ cell in the anterior chamber and the vitreous was clear.
 |
|
Rash. We noted macular skin rash on both legs but not on the soles of her feet.
|
Positive Tests
Because of the “mosquito bite” and her physical findings (migrating rash, pericarditis, Bell’s palsy, meningitis and panuveitis), there was a high suspicion for Lyme disease. Her lab workup included Lyme IgG and IgM antibody titers, and Lyme PCR from the CSF, as well as labs to work up uveitis, including ANA, ACE, RPR, FTA-Ab and rheumatoid factor. A chest x-ray was also ordered.
In the interim, neurology considered starting her on steroids and IV acyclovir and IV ceftriaxone because of a suspected viral meningitis or Lyme disease. However, the decision was made to wait until some of the labs came back. She was started on prednisolone acetate 1 percent every two hours in the right eye.
The next day, the patient’s vision was the same, but there were fewer keratic precipitates and reduced cell in her right eye. The vitreous haze was unchanged. Her lab showed a normal ACE level, but her x-ray showed hilar lymphadenopathy, a classic sign of sarcoid. Rheumatology was consulted, and a punch biopsy of the rash was performed which showed noncaseating granulomas, also a hallmark of sarcoid.
Upon review, many of her symptoms (such as shortness of breath) and her findings (such as Bell’s palsy, panuveitis, lymphocytic meningitis and rash) could be explained by sarcoid. Her triad of bilateral parotid enlargement, uveitis and facial nerve palsy is known as uveoparotid (Heerfordt’s) syndrome. Her combination of erythema nodosum, arthritis and hilar lymphadenopathy is known as Lofgren’s syndrome.1 The results were negative. The patient was discharged on prednisone 60 mg daily.
Discussion
Sarcoid is an unusual cause of facial palsy, with Bell’s palsy the most common cause of a unilateral facial paralysis. The source of Bell’s palsy is unknown, and other causes of facial palsy—such as trauma and tumors, as well as infectious, vascular and autoimmune conditions—should be excluded. The infectious causes of facial palsy include Lyme borreliosis, otitis media, syphilis, tuberculosis and varicella zoster. A tumor in the cerebellopontine angle or in the parotid gland can lead to facial nerve palsy. Vascular causes include diabetes, or a stroke in the pontine brain stem. Autoimmune causes besides sarcoid include Guillain-Barré. CNS manifestations occur in 5 to 12 percent of patients with sarcoid.2 The neurologic manifestations of neurosarcoid include cranial nerve palsies (usually facial nerve), hypothalamus or pituitary involvement, and optic nerve infiltration leading to atrophy. If neurosarcoid is suspected, a CT or MRI of the brain should be ordered.
Because Lyme disease also can present with facial nerve palsy, rash, lymphadenopathy, uveitis and a lymphocytic pleocytosis of the CSF, a careful history should be performed, including asking about tick bites and migrating skin rashes. Imaging (chest x-ray and brain CT), lab tests (Lyme titers and serum ACE levels) and skin biopsy (as in this case) can also help to differentiate sarcoid from Lyme. Even if the chest x-ray is normal, a chest CT should be considered, because pulmonary sarcoid can be missed on chest radiograph.3Serum ACE levels reflect disease activity and can be normal in sarcoid. If there is a suspicious lesion on the skin, conjunctiva or lacrimal gland, it should have a biopsy, since the diagnosis of sarcoid can only be made from a biopsy showing noncaseating granulomas.2 A transbronchial biopsy can also be done in patients with hilar lymphadenopathy.
Patients with anterior uveitis from sarcoid can be managed with topical steroids and cycloplegics. If there is systemic involvement or if the posterior eye is involved, the use of systemic steroids or periocular steroids is apt. Before starting systemic or periocular steroids, a PPD and FTA-ABS is needed to rule out tuberculosis and syphilis.
In cases requiring high doses of steroids longer than three months, immunomodulatory therapy, such as methotrexate, should be considered.4
Follow Up
Four weeks after discharge from the hospital, Ms. Moore still had blurry vision but no longer had any floaters. Her vision was 20/40 in both eyes, and she had 2+ vitreous haze. She had been seen by rheumatology and was started on methotrexate, and the prednisolone dose was being tapered.
___________________________
* Patient’s name is fictitious.
___________________________
Dr. Hsia is a resident and Dr. Hynes is an associate professor of ophthalmology at George Washington University.
___________________________
1 Rothova, A. Br J Ophthalmol 2000;84:110–116.
2 Whitcup, S. and R. B. Nussenblatt. Uveitis: Fundamentals and Clinical Practice (Philadelphia: Mosby, 2004):301–308.
3 Kaiser P. K., et al. Am J Ophthalmol 2002;133:499–505.
4 Nelson, Mark. Ophthalmology Pearls, 1st ed. (Philadelphia: Hanley & Belfus. 2003), pp. 39–41.