Download PDF
The gabapentinoids gabapentin and pregabalin are among the most commonly prescribed drugs in North America. Now, researchers have found an association between gabapentin and the incidence of acute angle-closure glaucoma (AAG).1 A similar association was not found for pregabalin.
Both drugs are approved to treat epilepsy and selected chronic pain conditions and are widely used off-label for mood disorders and pain.2 “We were surprised that this commonly prescribed psychotropic agent might increase the risk of AAG,” said coauthor Mahyar Etminan, PharmD, MSc, at the University of British Columbia Eye Care Center in Vancouver, British Columbia, Canada.
The bottom line, he said: “If you see patients with acute angle-closure glaucoma and they are on gabapentin, this drug might be the culprit.”
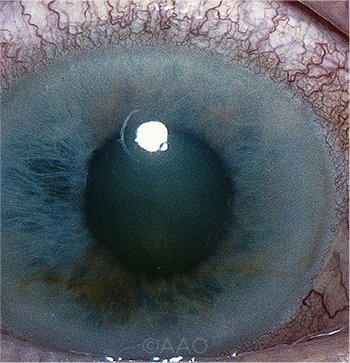 |
RX LINK. Additional evidence has emerged of a link between acute angle-closure glaucoma (shown here) and gabapentin use.
|
Study rationale. Previously, gabapentin has been linked to AAG, but only in case reports citing complaints of blurred vision, nystagmus, diplopia, and visual defects. These reports, plus the wide use of the drug, factored into the decision to conduct a large epidemiological study, Dr. Etminan said.
Study specifics. Researchers evaluated a random sample of 1,307 patients who developed AAG after gabapentin and pregabalin exposure in the year before diagnosis. The sample, drawn from a medical and pharmaceutical claims database over a 10-year period ending Dec. 31, 2016, also included 13,070 controls.
Who’s at risk? Gabapentin use in the year before AAG diagnosis was associated with a 42% increase of AAG, the researchers found. However, no association was found for current use of either gabapentin or pregabalin.
In addition, the incidence of AAG was associated with moderate drug exposure (3-5 prescriptions in the year before diagnosis). In contrast, neither limited exposure (1-2 prescriptions) nor significant exposure (6 or more) yielded an association with AAG. The small number of cases identified for significant exposure may have affected results, the researchers noted.
Method of action? The authors theorized that the mechanism of AAG associated with gabapentin use is similar to that of topiramate with regard to forward displacement of the ciliary body.
Clinical implications. While the findings need to be validated by other studies, Dr. Etminan suggested that ophthalmologists closely evaluate patients diagnosed with AAG who are on gabapentin. He added that it’s possible that patients with a previous history of AAG might be able to safely take pregabalin instead.
—Miriam Karmel
___________________________
1 Browne MJ et al. J Glaucoma. 2019;28(9):777-779.
2 Goodman CW, Brett AS. JAMA Intern Med. 2019;179(5):695-701.
___________________________
Relevant financial disclosures—Dr. Etminan: None.
For full disclosures and the disclosure key, see below.
Full Financial Disclosures
Dr. Deobhakta Alimera Sciences: C; Allergan: C.
Dr. Etminan None.
Dr. Friedlander None.
Dr. VanderBeek NEI/NIH: S; Paul and Evanina MacKall Foundation: S; Research to Prevent Blindness: S.
Disclosure Category
|
Code
|
Description
|
| Consultant/Advisor |
C |
Consultant fee, paid advisory boards, or fees for attending a meeting. |
| Employee |
E |
Employed by a commercial company. |
| Speakers bureau |
L |
Lecture fees or honoraria, travel fees or reimbursements when speaking at the invitation of a commercial company. |
| Equity owner |
O |
Equity ownership/stock options in publicly or privately traded firms, excluding mutual funds. |
| Patents/Royalty |
P |
Patents and/or royalties for intellectual property. |
| Grant support |
S |
Grant support or other financial support to the investigator from all sources, including research support from government agencies (e.g., NIH), foundations, device manufacturers, and/or pharmaceutical companies. |
|
More from this month’s News in Review