Download PDF
When researchers at the Academy’s 2013 annual meeting reported an association between birth control pills and glaucoma, it created a stir in the news media and on the Internet. The study in question found that women who used oral contraceptives (OCs) for more than three years had a twofold risk of developing primary open-angle glaucoma (POAG) later in life.1
Yet while the media played up the story, one of the coauthors, Shan Lin, MD, at the University of California, San Francisco, emphasized that further studies are needed to validate the findings, which were based on patients’ self-report of a glaucoma diagnosis. Dr. Lin noted that the results don’t indicate a direct causative effect; rather, they suggest OC use as a potential risk factor for glaucoma. “It’s just another piece of the puzzle to build a case for the role of estrogen in optic nerve health.”
Still, given the widespread publicity, as well as the common use of OCs, many women are asking their ophthalmologists about the possible risks. To respond to patients’ concerns, it’s helpful to take a step back and look at the larger context of what recent research shows about the role of estrogen and, possibly, other sex hormones in glaucoma.
|
Differences Beyond Biology
|
 |
|
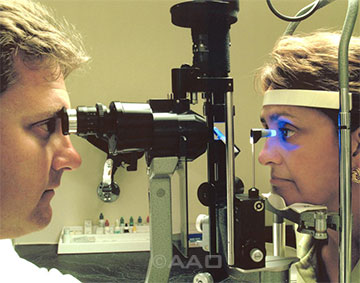
Women and their ophthalmologists need to be aware of hormonal risk factors for development of glaucoma.
|
Gender Differences in Glaucoma
“I’m excited that there’s a great deal more interest in this area of gender biology,” said Jae Hee Kang, MSc, ScD, coauthor of an earlier study that, like Dr. Lin’s, found an association between OC use and glaucoma. Dr. Kang said that these studies might reveal something about the etiology of the disease: “Estrogen affects so many processes that are involved in glaucoma.”
Thasarat S. Vajaranant, MD, at the Illinois Eye and Ear Infirmary, has explored the relation between gender and glaucoma and asks whether there is something in particular about women that predisposes them to glaucoma. “The degree of sex predilection depends on the type of glaucoma,” she said. “So the answer is yes, for angle-closure glaucoma, and perhaps ‘inconclusive’ for primary open-angle glaucoma.” What changes the odds? “Data suggest that women do have a unique risk factor. For instance, if a woman enters menopause at a much younger age, her risk for glaucoma later in life is higher,” she said.
Dr. Kang, at Brigham and Women’s Hospital, noted other factors specific to females. “Women who develop glaucoma often have lower IOP than men. We also know that IOP decreases during pregnancy and fluctuates with the menstrual cycle.”
Pieces of the Puzzle
Piece by piece, researchers are accumulating evidence to support the theory that circulating estrogen may play an important role in the pathogenesis of glaucoma. They hypothesize that reduced exposure to estrogen contributes to increased susceptibility of the optic nerve to glaucomatous damage and that estrogen may provide a protective effect against glaucoma.
Reproductive factors and glaucoma. A flurry of studies in the 2000s uncovered risk associations between various reproductive factors and glaucoma; these include early menopause, late menarche, oophorectomy, and most recently, oral contraceptive use. Some studies have found protective effects from late menopause or hormone replacement therapy.
“We know that early loss of estrogen is associated with increased risks of a variety of health outcomes, including several conditions related to brain aging,” Dr. Vajaranant said. “We also know that the major risk factor for glaucoma is advanced age. Therefore, one possibility is that an early loss of estrogen causes the optic nerve to age prematurely and predisposes the optic nerve to glaucomatous damage.
“The Rotterdam Study is the first population-based study suggesting that early menopause increases risk for glaucoma,” Dr. Vajaranant continued. The Rotterdam group found that menopause before the age of 45 was associated with a 2.6-fold increased risk of POAG.2 “Other studies, including the Blue Mountains Eye Study3 and the Nurses’ Health Study,4 in part support the theory that decreased lifetime estrogen exposure might increase the risk for glaucoma later in women’s life,” she said.
Dr. Vajaranant’s recent study of oophorectomy adds more evidence. She found that women who underwent bilateral removal of the ovaries before age 43 had a significantly increased risk of glaucoma. Hormone replacement therapy did not diminish the risk.5
How Does Estrogen Protect?
The mechanism of estrogen’s protective effect remains unclear, but most of the evidence suggests that it may be neuroprotective, said Dr. Lin. He explained that estrogen receptors are expressed in a variety of ocular tissues, including the retinal ganglion cells (RGC), where estrogen appears to have a maintenance effect.
One mechanistic theory holds that estrogen activates the synthesis of collagen fiber, increasing the amount of collagen fiber at the lamina cribrosa, thus improving the structure’s compliance. This could relieve compression on RGC axons, aiding in their survival. Increased collagen fiber also could enhance flexibility of the whole eye, which would lead to decreased IOP, Dr. Lin said.
Dr. Kang offered another theory: Estrogen has known effects on nitric oxide production, which is important in IOP regulation and in vasodilation. Thus, a decline in estrogen could diminish blood flow to the optic nerve.
New Findings on HRT
A number of studies have suggested that hormone replacement therapy (HRT) in postmenopausal women may be beneficial in reducing intraocular pressure or the incidence of glaucoma. However, most of these studies have been limited by methodological issues, particularly small sample sizes.
The size limitation was overcome in a recently published retrospective longitudinal cohort analysis of 152,163 women in a U.S. managed care system.1 Participants were aged 50 or older who had at least two eye care visits from 2001 to 2009. Of these patients, 70,292 were taking one of three types of HRT: estrogen only (E), estrogen plus progesterone (E+P), or estrogen plus androgen (E+A).
After adjustment for age, patients taking E or E+P had a statistically significant reduction in POAG compared with those not taking HRT (there was no significant difference with E+A). The researchers estimated that four years of continuous use yielded a hazard reduction of 18 percent and 26 percent, respectively for E and E+P. After adjustment for other factors including sociodemographic factors and comorbidities, the E group continued to show a statistically significant risk reduction.
___________________________
1 Newman-Casey PA et al. JAMA Ophthalmology. 2014 Jan. 30. [Epub ahead of print.] |
The Pill Paradox
If estrogen has a protective effect, why would oral contraceptives, which contain estrogen, increase the risk of glaucoma? Oral contraceptives differ from endogenous estrogens in several ways.
Different formulations. Dr. Kang noted that there are several different formulations; some contain progestin only, which suppresses estrogen. But even OCs that include estrogen contain just enough to suppress ovulation, she said, which changes the monthly hormonal patterns. “You don’t have the very high spikes of estrogen that you have when you’re not on them [OCs].”
In addition, the formulations have changed since the first oral contraceptive was approved in 1960, with the early generation containing higher levels of estrogen than current versions. Dr. Kang would like to study whether the changes in formulation over time have affected glaucoma risk.
What the studies show. Dr. Kang’s prospective longitudinal incidence study (coauthored with Louis R. Pasquale, MD) followed 79,440 women in the Nurses’ Health Study. They identified 813 cases of incident POAG among women age 40 or older who had been free of POAG at baseline. The study found no association overall between ever having used OC and POAG risk; however, with five or more years of OC use, there was a 25 percent increased risk of POAG.4
Dr. Lin’s prevalence study used data from the National Health and Nutrition Examination Survey, which included 3,406 women aged 40 or older, from across the United States. The participants completed the survey’s vision and reproductive health questionnaire and underwent limited visual testing. The data yielded an odds ratio of 2.05 for having self-reported glaucoma among women using oral contraceptives for more than three years.1
Despite the methodological differences between these studies, both point in the same direction. Dr. Lin’s OC study “nicely supports the growing body of literature on hormone-based pathophysiology of glaucoma,” said Dr. Vajaranant.
Differences Beyond Biology
In addition to biological differences in the risk for glaucoma, gender disparities in treatment also exist, said Dr. Vajaranant. She said one study found that women in the United States are 24 percent less likely to be treated for glaucoma than men.1 “I don’t think we clearly understand why.” She added, “Interestingly, the gender disparity in treatment is consistent with other studies showing lower [rates of] treatments in ICU and cardiovascular diseases.”
___________________________
1 Friedman DS et al. Ophthalmology. 2005;112(9):1494-1499. |
Clinical Implications
Despite all the buzz it generated, the OC study Dr. Lin coauthored was, as he put it, just another piece of the puzzle. “By no means are we telling women not to use birth control pills,” he said. “The recommendation at this point is a cautionary one. If women have a particular predilection for glaucoma, such as African-American heritage, family history, and/or older age, this factor of birth control use would encourage at least a baseline screening for glaucoma.”
Dr. Vajaranant agreed that anyone at risk should get a baseline eye exam and a routine glaucoma screening. She added that ophthalmologists need to be aware that changing levels of sex hormones in different phases of a woman’s life can influence clinical measurements. “For instance, intraocular pressure decreases during pregnancy, and visual field (as measured by short-wavelength perimetry) varies during a menstrual period.”6
The bottom line. “The growing evidence of the influence of female sex hormones on glaucoma suggests that there are unique, sex-specific risk factors for glaucoma in women, such as early menopause and the use of female hormones,” Dr. Vajaranant said. “We, the Eye M.D.s, should be aware of these risks and offer appropriate recommendations and management for our patients. We need to have a better understanding of sex differences that affect eye diseases when caring for our patients.”
___________________________
1 Wang YE et al. Association between oral contraceptive use and glaucoma in the United States. Poster presented at: Annual Meeting of the American Academy of Ophthalmology; Nov. 17-19, 2013; New Orleans. PO339.
2 Hulsman CA et al. Am J Epidemiol. 2001;54(2):138-144.
3 Lee AJ et al. Br J Ophthalmol. 2003;16(7):598-605.
4 Pasquale LR, Kang JH. Eye. 2011;25(5):633-641.
5 Vajaranant TS et al. Menopause. 2013 Sep 2. [Epub ahead of print].
6 Akar Y et al. Ophthalmologica. 2005;219(1):30-35.
___________________________
Jae Hee Kang, MSc, SCD, is an epidemiologist and assistant professor of medicine, Brigham and Women’s Hospital, Boston. Financial disclosure: None.
Shan Lin, MD, is professor of clinical ophthalmology and director of the glaucoma service at the University of California, San Francisco. Financial disclosure: Dr. Lin was on the advisory board for Allergan last year, but he reports no interests relevant to this topic.
Thasarat S. Vajaranant, MD, is associate professor of ophthalmology and director of the glaucoma service, Illinois Eye and Ear Infirmary at University of Illinois, Chicago. Financial disclosure: None.