Download PDF
Some cardiovascular and eye diseases share underlying mechanisms. Recognizing and responding to these interlinking “root systems” may have broad and far-reaching implications for many patients.
The patient in your office is far more than just a pair of eyes. That point has been driven home in recent years by a number of studies linking ophthalmic diseases with systemic conditions, notably cardiovascular disease. As ophthalmologists tend to focus on eye-specific mechanisms and treatment of diseases, seeing the broader picture may be quite revealing, said Tien Yin Wong, MBBS, PhD, MPH, at the Singapore National Eye Centre. “There is a growing realization that a few fundamental mechanisms underlie cardiovascular disease and many eye diseases,1 particularly those related to aging and chronic conditions such as age-related macular degeneration [AMD], glaucoma, and diabetic retinopathy.”
In addition to sharing a strong underlying pathogenesis and several risk factors with cardiovascular disease, many eye diseases may even benefit from some of the same types of treatment, said Dr. Wong.
 |
|
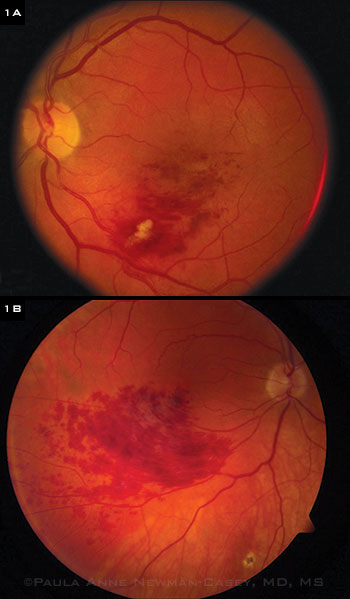
Patients with hypertension are at significant risk of developing BRVO, seen here.
|
Shared Pathways of Disease
A number of studies have shown strong links be tween carotid disease and eye diseases, said Dr. Wong. “It has been observed that if atherosclerosis is detected in carotid vessels, for example, the patient is more likely to have AMD and diabetic retinopathy.”
Atherosclerosis may cause cholesterol buildup right in the retina, which may predispose patients to AMD, said Rohit Varma, MD, MPH, at the University of Southern California in Los Angeles. “Aging macrophages clear fewer fat deposits beneath the retina, which becomes bloated with cholesterol,” Dr. Varma said. “This creates inflammation in the retina and can lead to the formation of new blood vessels, which ultimately leads to vision loss.”
Inflammation is a central pathway of both cardiovascular disease and many eye conditions, said Dr. Wong. In fact, inflammatory markers such as C-reactive protein are associated with both heart disease and wider retinal venules, said Ronald Klein, MD, MPH, at the University of Wisconsin in Madison. Although these small retinal vessels may be markers for similar changes in the heart, it’s premature to use them as a clinical screening tool to estimate risk of developing a heart attack, Dr. Klein said. “Physiological factors such as blood flow and oxygenation of the blood—not long-term structural changes—may transiently cause these vessels to widen or narrow.” Emerging technologies may one day better enable evaluation of these changes.2
 |
|
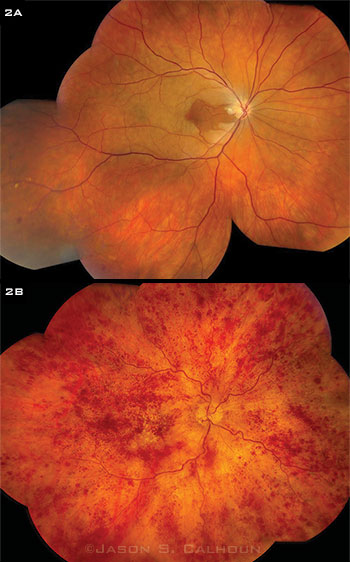
Occlusions—whether arterial (Fig. 2A) or venous (2B)—may signal the presence of significant vascular disease throughout the body.
|
Shared Risk Factors
Many well-known risk factors contribute to shared underlying pathways of disease. “Risk factors for heart disease, such as hypertension, smoking, and elevated blood lipids, also apply to ischemic disorders of the eye,” said Eric P. Purdy, MD, with Vision Care Associates in Fort Wayne, Ind. He is double-boarded in internal medicine and ophthalmology and formerly chaired BCSC section 1 on general medicine.
Hypertension. According to the NIH, about 65% of U.S. adults age 60 or older have hypertension—and the prevalence of the disease is increasing in teens and young adults. Moreover, hypertension is strongly associated with several eye diseases, such as diabetic retinopathy, said Dr. Wong. Suggesting a cause-effect relationship, “the U.K. Prospective Diabetes Study Group showed that control of hypertension reduces the progression of retinopathy,” he said.
With other diseases, there is an even stronger shared pathogenic pathway, said Dr. Wong. One investigation showed that hypertensive patients were 5 times more likely to have branch retinal vein occlusion (BRVO).3
Hypertension is a main driver and risk factor for BRVO, agreed Paula Anne Newman-Casey, MD, MS, at the University of Michigan Kellogg Eye Center in Ann Arbor (Figs. 1A, 1B). “The risk of a vein occlusion really jumps when people begin to have damage in smaller vessels,” she said. In fact, the risk of a vein occlusion nearly triples in those with complications from hypertension such as neuropathy or nephropathy.4
Two other eye diseases are also likely have a relationship to blood pressure, said Dr. Wong. The Beaver Dam Eye Study showed that an increase in blood pressure from baseline to 5-year exam was followed by an increase in the risk of AMD progression at 10 years.5 And, although glaucoma is traditionally considered a disease mediated by intraocular pressure (IOP), Dr. Wong said, blood pressure levels and oxygenation of the optic nerve head have been found to heavily influence a person’s risk of the disease.6
Cigarette smoking. Smoking has long been recognized as having a deleterious effect on blood vessels, said Dr. Klein. If you can diminish that inflammatory injury, added Dr. Purdy, you can diminish the whole cascade of atherosclerosis.
No one doubts smoking’s clear link to the risk of stroke and heart disease, said Dr. Wong, and the data linking smoking and AMD are robust. However, smoking is not uniformly associated with AMD, said Dr. Varma, pointing to a genetic predisposition in certain smokers. “We have not seen a strong relationship between smoking and macular degeneration in nonwhite groups,” he said, adding that rates of AMD may simply be lower in nonwhites.
Smoking is also associated with dry eye syndrome, which may worsen as people age, said Dr. Varma. With regard to diabetes, he said, “Although smoking increases the risk of diabetes, we don’t think it worsens diabetic eye disease.”
Lipids. “Gaining more prominence, but needing additional research, is the lipids part of the story,” said Dr. Wong. Previous studies on the relationship between lipids and eye disease have produced inconsistent data.
“We now recognize that looking only at cholesterol levels is overly simplistic,” he said. “The proteins and enzymes that control these lipid levels—the underlying pathways of cholesterol metabolism—may have more to do with these diseases than cholesterol levels themselves. Measured in the blood, markers associated with these cholesterol changes are now seen as quite important in the pathogenesis of AMD.”
Obesity. Obesity is also part of this story, but body weight is only the tip of the iceberg, as alterations in fatty deposits, lipid metabolism, inflammation, genetic predisposition, and inactivity likely contribute to some chronic eye diseases as well as to cardiovascular disease, said Dr. Wong.
Metabolic syndrome. Of course, many people do not have risk factors in isolation. For example, metabolic syndrome increases the risk of heart disease, said Dr. Varma. (To be diagnosed with metabolic syndrome, a person must have 3 of the 5 following features: central obesity, hypertriglyceridemia, dyslipidemia, elevated blood glucose, and hypertension.) “There is also an association between metabolic syndrome and retinopathy”—and, in some instances, an association between metabolic syndrome and cataract and raised IOP, he said.
An increased prevalence of metabolic syndrome among Latinos puts them at higher risk of related changes in the eye, said Dr. Varma. “Latinos should be carefully and regularly assessed for those ocular changes so that we can pick them up early.”
 |
|
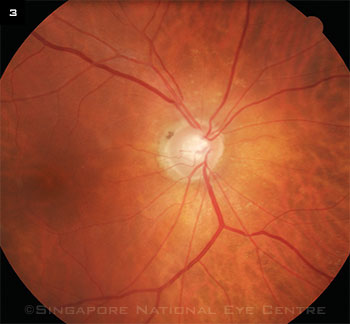
Mild hypertensive retinopathy with narrowed arterioles and arteriovenous nicking.
|
Shared Treatment?
Shared underlying mechanisms and risk factors suggest the potential for shared solutions, said Dr. Wong. “Some of the therapy that controls lipid mechanisms, inflammation, and blood pressure—treatments traditionally used for cardiovascular disease—are now being explored as possible therapies for prevention and treatment of eye diseases related to aging.”
Statins. Dr. Newman-Casey and her colleagues have found that statins lower the risk of developing open-angle glaucoma (OAG);7 and these cholesterol-lowering drugs have also been found to be protective against uveitis.8 In her study, Dr. Newman-Casey said, “We looked at different classes of medications, and statins were a standout. Other cholesterol-lowering medications did not have the same effect.” Although the mechanism of protection is unclear at this point, several anti-inflammatory and immunomodulatory mechanisms may be involved.8
CETPIs. Researchers are also evaluating novel classes of drugs such as cholesterol esterase transfer protein inhibitors (CETPIs), said Dr. Wong, to see if alterations in cholesterol levels might have an effect on macular degeneration and diabetic retinopathy.
Fenofibrates. Traditionally used to treat cardiovascular disease, fibrates more directly affect specific pathways of lipid metabolism than they do total levels of cholesterol, said Dr. Wong. They are used less commonly now that statins have become a mainstay for cardiovascular disease.
However, fenofibrates have been shown to be protective against the progression of diabetic retinopathy.9,10 One possible explanation for their protective effects is their action on inflammatory processes.
 |
|
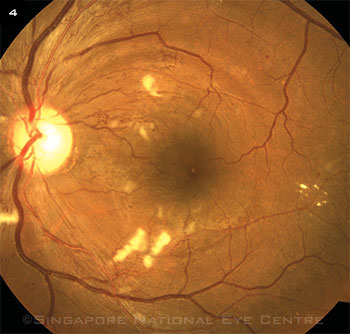
Moderate hypertensive retinopathy with cotton-wool spots, microaneurysms, and hemorrhages.
|
Signs of Shared Risk Factors
The retinal vessels of the eye provide ophthalmologists with a biomarker for what may be happening in the brain or the small vessels of the heart, said Dr. Klein.
Changes in microvasculature. The most common ocular side effects of cardiovascular disease appear in disorders that share a common pathway—atherosclerosis, said Dr. Purdy (Figs. 2A, 2B). “This affects blood vessels throughout the body, including small arteries supplying blood to the retina and optic nerve. When these small arterioles develop arteriosclerosis, their lumens become narrowed.”
Arteriovenous nicking (Fig. 3) is another ocular sign that may reflect the effects of blood pressure and other systemic factors on the retinal vasculature. Nicking appears in areas where retinal arterioles cross above venules, causing constriction in the underlying venule, said Dr. Klein.
Emboli and occlusions. In addition to these local changes, small bits of cholesterol can break off from bigger plaques in the carotid artery and get pushed into the eye’s smaller vessels, said Dr. Varma.
Dr. Purdy said, “With central retinal artery occlusion [CRAO], you might see a small embolus or thrombus wedged in the central retinal artery, blocking blood flow to the eye. Little ‘boxcars’ of blood may sit motionless in the arteries. The retina becomes fairly pale and arterioles may be very narrowed. Nearly complete vision loss may occur.”
With a branch retinal artery occlusion, partial visual loss can occur, but symptoms depend upon the location of the blockage, said Dr. Purdy. “For example, if the superior temporal retinal artery is blocked, that produces an inferior nasal visual field defect.”
Ischemic events. Complete blockage of blood flow may cause ischemic events in the eye and sudden partial or complete visual loss in one eye. “Signs of ischemic optic neuropathy include a pale and/or swollen optic nerve and hemorrhages,” Dr. Purdy said. “A patient often experiences nearly complete vision loss or an altitudinal defect.” With ocular ischemic syndrome, he said, the eye becomes starved for oxygen, which can cause discomfort, inflammation, redness, and changes in eye pressure.
Dr. Purdy added, “The eye sometimes compensates with neovascularization—also a hallmark of diabetic retinopathy—which can lead to bleeding, retinal detachment, vision loss, and possibly neovascular glaucoma.”
Other signs. Raised, yellow patches of skin around the eyelids, called xanthelasma, may appear in people with uncontrolled lipids, but with the broad use of statins, this condition is less common than in the past, said Dr. Klein.
People with xanthelasma, however, are more likely to have a heart attack or die of heart disease, Dr. Varma said. The risk of heart disease is 12% higher in men and 8% higher in women with xanthelasma,2 he said.
In uncontrolled hypertension, the ophthalmologist may see “flame-shaped hemorrhages, exudation, and swelling,” said Dr. Newman-Casey. Cotton-wool spots also may be evident (Fig. 4). The clinician also may note signs of another important cardiovascular risk factor that can occur in patients with hypertension: sleep apnea.3 Fortunately, she said, ophthalmologists are becoming a bit savvier about sleep apnea. “For example, when they see people with signs such as floppy eye syndrome, they know to send them to a primary care physician for a sleep apnea evaluation.”
A note on gender. Physicians have long suspected that women and men have different patterns of cardiovascular disease, said Dr. Wong. Women are more likely to experience microvascular, longer-lasting angina from spasms within arteriolar walls,7 instead of the typical symptoms of chest pain or large vessel blockage found in men.
“Unfortunately, standard tests such as coronary angiograms are more likely to miss this microvascular disease,” said Dr. Wong. “It requires more extensive imaging,” such as magnetic resonance imaging (MRI).
Dr. Wong and his colleagues have looked at the microvascular caliber of the retinal vessels to see if it could predict cardiovascular disease. “We found that women with microvascular narrowing in the retinal arterioles were more likely to develop heart disease, a finding that was not duplicated in men.”
This information supports the ongoing hypothesis that women are more likely to have microvascular pathways in their pattern of cardiovascular disease, Dr. Wong said. “However, it is too early to be used as a standard prognostic tool by the clinician.”
Research Update: Stroke
Two studies published earlier this year underscore the point that patients with retinal vein or artery occlusion may also be at increased risk of a stroke.
RVO and stroke. In a nationwide population-based study, Korean researchers evaluated the risk of stroke development following RVO.1 Over a 9-year period, they found that stroke developed in 16.8% of patients diagnosed with RVO and in 10.7% of patients in a comparison group. The presence of hypertension, diabetes, and chronic kidney disease also increased stroke risk.
CRAO, heart disease risk, and stroke. Researchers with the European Assessment Group for Lysis in the Eye (EAGLE) assessed underlying risk factors in patients with nonarteritic CRAO.2 They found previously undiagnosed vascular risk factors in 78% of the CRAO patients; the most meaningful was ipsilateral carotid artery stenosis.
Moreover, they found that stroke risk was highest within the first 4 weeks after CRAO was diagnosed—and they concluded that “a comprehensive and prompt diagnostic workup is mandatory for all CRAO patients.”
___________________________
1 Rim TH et al. Ophthalmology. 2015;122(6):1187-1194.
2 Callizo J et al. Ophthalmology. 2015;122(9):1881-1889.
|
The Ophthalmologist’s Role
With increasing subspecialization in medicine, it can be challenging to step back and see the bigger picture. But ophthalmologists can play a significant role in safeguarding a patient’s overall health, the experts said.
Spot the earliest signs. Ophthalmologists may be the first to see warning signs, such as retinal refractile deposits that cause no symptoms but indicate a patient might require further evaluation, said Dr. Purdy. These deposits may represent small cholesterol emboli from atherosclerotic plaque.4
“Although ophthalmologists are proficient at diagnosing ocular ischemic events, sometimes the underlying cause can be elusive, and that’s where referral for a cardiovascular workup, such as an echocardiogram or ultrasound, may be critical,” he said. “You can’t just assume the problem is due to small vessel arteriosclerosis in the eye. It may have originated with a dislodged piece of cholesterol, calcium, or thrombus from the carotid artery or from the heart, due to an arrhythmia or a diseased heart valve.”
Monitor high-risk patients. It’s also important to keep a closer watch on patients who are considered to be at high risk, said Dr. Varma. This category includes those who are obese or have elevated blood pressure, cholesterol, or blood sugar levels, as well as those who have a history of heart disease. “They are all at risk for developing changes in the retina.”
Be cognizant of drug side effects. Drugs used to treat cardiovascular conditions can have ocular side effects—and vice versa (see “Drug Side Effects: A 2-Way Street,” below).
(click to expand)

Communicate. “A retinal vein occlusion is vascular disease gone terribly awry,” said Dr. Newman-Casey. “When it appears, there is likely significant atherosclerosis present throughout the body.” (See “Research Update: Stroke,” above.)
Systemic risk factors need to be addressed to prevent other problems, she said. “This is a teachable moment for the patient and an opportunity to engender good communication between the specialist and primary care physician. We do this well for diabetes, and we need to do the same for vein occlusions.”
Dr. Varma agreed. “It is critical for us to identify early signs of systemic conditions and refer those persons to our cardiology and internal medicine colleagues,” he said. “It is possible to lower cholesterol, blood pressure, and blood glucose. We can help people lose weight, exercise more, or stop smoking—there are many ways to potentially reduce risks of cardiovascular and eye diseases. That’s where we can really add value.”
___________________________
1 Cheung CM, Wong TY. J Intern Med. 2014;276(2):140-153.
2 Pinhas A et al. Biomed Opt Express. 2013;4(8):1305-1317.
3 Wong TY, Mitchell P. Lancet. 2007;369(9559):425-435.
4 Newman-Casey PA et al. Ophthalmology. 2014;121(10): 1939-1948.
5 Klein R et al. Ophthalmology. 2003;110(6):1273-1280.
6 Zhao D et al. Am J Ophthalmol. 2014;158(3):615-627.
7 Stein JD et al. Ophthalmology. 2012;119(10):2074-2081.
8 Borkar DS et al. Am J Ophthalmol. 2015;159(4):707-713.
9 Keech AC et al. Lancet. 2007;370(9600):1687-1697.
10 Wong TY et al. Am J Ophthalmol. 2012;154(1):6-12.
Further Reading
For further reading about the links between eye diseases and cardiovascular disease, the following may be of interest.
Basic and Clinical Science Course. Section 1, Update on General Medicine. American Academy of Ophthalmology; 2015.
Cheung N, Wong TY. Obesity and eye diseases. Surv Ophthalmol. 2007;52(2):180-195.
Cheung N, Wong TY. Diabetic retinopathy and systemic vascular complications. Prog Retin Eye Res. 2008;27(2):161-176.
Silva PS et al. Effect of systemic medications on onset and progression of diabetic retinopathy. Nat Rev Endocrinol. 2010;6(9):494-508.
Wong TY et al. Associations between the metabolic syndrome and retinal microvascular signs: The Atherosclerosis Risk in Communities study. Invest Ophthalmol Vis Sci. 2004;45(9):2949-2954.
|
Meet the Experts
Ronald Klein, MD, MPH Professor of ophthalmology and visual sciences at the University of Wisconsin in Madison; coprincipal investigator of the Wisconsin Epidemiologic Study of Diabetic Retinopathy and the Beaver Dam Eye Study. Relevant financial disclosures: None.
Paula Anne Newman-Casey, MD, MS Assistant professor of ophthalmology and visual sciences at the University of Michigan Kellogg Eye Center in Ann Arbor. Relevant financial disclosures: None.
Eric P. Purdy, MD Double-boarded in internal medicine and ophthalmology and in practice with Vision Care Associates in Fort Wayne, Ind. Relevant financial disclosures: None.
Rohit Varma, MD, MPH Professor and chair of ophthalmology at the University of Southern California and director of the USC Eye Institute in Los Angeles. Relevant financial disclosures: Aerie Pharmaceutical: C; AqueSys: C; Bausch + Lomb: C; Genentech: C,S; NEI: S; Research to Prevent Blindness: S.
Tien Yin Wong, MBBS, PHD, MPH Professor and medical director of the Singapore National Eye Centre; chair of ophthalmology and vice-dean of clinical sciences at the Duke-NUS Medical School at the National University of Singapore. Relevant financial disclosures: Allergan: C,L; Allergan Singapore: C,L; Bayer Healthcare: C,L,S; Bayer Healthcare Pharmaceuticals: C,L,S; Novartis: C,L,S.
For full disclosures and the disclosure key, see below.

|