This article is from March 2007 and may contain outdated material.
Like anyone with refractive errors, the patient with keratoconus seeks the best visual acuity possible. Yet performing refractive laser surgery on such a patient is a potential recipe for disaster, and the reason is obvious.
“The pathology of a thinning cornea, together with further removing tissue with a laser, is not in the patient’s best interest, an observation shared by most ophthalmologists,” said Michael W. Belin, MD, professor of ophthalmology and director of cornea and refractive surgery at Albany Medical College in New York.
Nor is laser correction in the physician’s interest, said Walter J. Stark, MD. “If a cornea is thin and has keratoconus, it is more prone to bowing forward, which further weakens the cornea,” he said. “This poses a medical risk to the patient, as well as a legal risk for the doctor.” Dr. Stark is professor and director of the cornea service at the Wilmer Eye Institute in Baltimore.
But the consumer demand for perfect vision has created controversy over the best approach for correcting these patients. Indeed, Dr. Belin explained that some patients with early keratoconus have difficulty tolerating contacts, and so seek other solutions, including refractive laser surgery.
Before considering any treatment, physicians must distinguish between true keratoconus, early keratoconus and suspicions of keratoconus, which may make a difference in some physicians’ decision-making process.
First Question: Forme Fruste
Ophthalmologists may avoid refractive surgery on patients with established keratoconus, but another challenge comes when evaluating a patient for refractive surgery and determining whether that patient is predisposed to develop keratoconus, or presents with its early stages: forme fruste keratoconus. This is especially relevant given that keratoconus is more prevalent in young adults, who often seek out refractive surgery.
Difficulties with diagnosis. Even diagnosing forme fruste keratoconus is fraught with controversy. “Suspicious findings may be found on corneal topography,” explained Mitchell A. Jackson, MD, founder of Jacksoneye in Lake Villa, Ill. “However, there is some question about which topography system is better at picking up keratoconus in the early stages—Orbscan or Pentacam.”
In many instances, patients with forme fruste keratoconus do not present with any clinical signs or symptoms, Dr. Jackson pointed out. “There is no loss of best-corrected visual acuity, and everything looks perfectly normal on slit lamp, except for some strange topography.” Yet this can also be confusing, as topography findings that appear to be early keratoconus can mimic other eye conditions such as pellucid marginal degeneration, Terrien’s degeneration or contact lens warpage.
Contacts can be confounding. To rule out contact lens warpage, Dr. Jackson asks patients to go without their gas permeable lenses one month for every 10 years of wear, and watch for normalization. Soft lens users keep their lenses out three days to a week, and soft toric lenses may even take longer for stabilization. “We look at corneal thickness, shape of the cornea, and results from the Orbscan in an attempt to discover whether the patient has forme fruste keratoconus,” he said. “But this isn’t foolproof. When considering refractive surgery, we still don’t know the true corneal thickness that should be left in the bed to keep the cornea stable. You can follow all the right protocols, and your patient can still get corneal ectasia after refractive surgery.”
 |
|
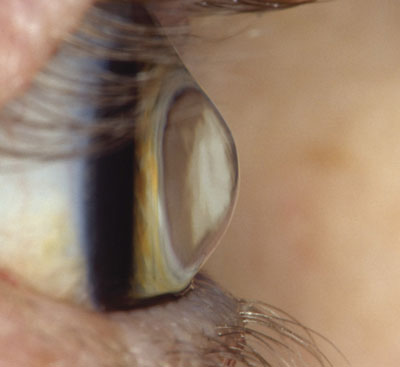
Lateral view of a keratoconic eye.
|
Next Question: Surface Ablation
Are all refractive procedures off-limits for keratoconus? “While it is pretty well-accepted that LASIK is contraindicated in patients with keratoconus, there is some debate whether you can use another surface treatment,” said Dr. Belin.
“Most people think that you are asking for trouble because you are already working with a structurally weak cornea, and to remove any anterior surface would be pushing the envelope,” said Roger F. Steinert, MD. “As for forme fruste keratoconus and surface treatment, the truth of the matter is the jury is still out. Conservative surgeons would say no, and the aggressive surgeons would say yes, but there are not enough long-term cases to say one way or another.” Dr. Steinert is professor of ophthalmology and biomedical engineering, and director of cornea, refractive surgery and cataract surgery at the University of California, Irvine.
Dr. Stark agreed. While some ophthalmologists will treat patients with forme fruste keratoconus using a surface treatment such as PRK, he said, “We are more conservative, and would prefer that patients stick with contact lenses until they need a cornea transplant.”
Misleading success? Dr. Belin pointed out that “a large number of reports in the literature showing reasonable results with surface treatment were not true keratoconus patients, but those with false positives, which result from the limitations of corneal topography and the lack of a complete analysis of the shape of the cornea. These patients are effectively normal, but appear to have keratoconus. I personally do not believe in performing corneal surgery on true keratoconus patients.”
Causes of Keratoconus
According to the National Eye Institute, keratoconus is the most common corneal dystrophy in the United States, affecting one in 2,000 Americans. Keratoconus is not fully understood, and its progression is unpredictable. Dr. Stark explained that the cause of the condition is multifactorial.
“Keratoconus is an abnormality of the collagen and can be associated with skin disease, such as atopic dermatitis,” he said. “So the condition is partly linked to this skin condition and partly linked to excessive eye rubbing.” About 7 percent of those with the condition have a family history of keratoconus. “We see this condition in families, especially in the Middle East where cousins sometimes marry cousins,” Dr. Stark added.
Keratoconus has also been linked to several other eye diseases, including retinitis pigmentosa, retinopathy of prematurity and vernal keratoconjunctivitis, as well as systemic diseases such as Leber’s congenital amaurosis, Ehlers-Danlos syndrome, Down syndrome and osteogenesis imperfecta.
|
Four Other Solutions
Contacts. Approximately 90 percent of patients with keratoconus are managed very early with glasses or standard gas-permeable contact lenses, Dr. Belin said. Only about 10 percent of patients require any surgical treatment.
Corneal inserts. Dr. Jackson noted that Intacs, or corneal inserts, are one alternative for patients with keratoconus. In this procedure, two tiny, clear, crescent-shaped pieces of plastic polymers are placed just under the eye’s surface in the periphery of the cornea to achieve a flatter cornea. “Any long-term effects that Intacs may have on the natural course of keratoconus are unknown,” he said. “However, the initial results are promising, and the best candidate is someone in the early to moderate stage of keratoconus who cannot wear glasses or be fitted with contact lenses, and who has little or no corneal scarring.”
Dr. Steinert added that while there is not much of a track record using Intacs for mild cases of keratoconus, it is theoretically an interesting approach. The virtue of the procedure is that Intacs can be removed with good reversibility of the effect should there be a problem.
Dr. Belin views Intacs as an alternative or intermediary step prior to corneal transplant surgery. “Intacs have allowed some patients to avoid the need for corneal transplants and others to have the procedure delayed.”
Phakic IOLs. The other possible alternative for patients with mild keratoconus is implanting a phakic IOL. “In this procedure,” Dr. Steinert explained, “you are not violating the cornea, so you won’t change the natural history of the cornea in terms of the effects of keratoconus. However, there are risks with phakic IOLs. In a situation where a corneal or refractive procedure is an ambiguous option, then it may be worth discussing phakic IOLs with the patient.”
New corneas. The traditional, and largely successful, treatment alternative for the patient with advanced keratoconus is corneal transplant. Dr. Steinert is involved in a new approach to corneal transplantation using the femtosecond laser. He says that preliminary results appear promising.
Window on the Future
Dr. Stark and his colleagues have started a keratoconus center at the Wilmer Eye Institute, looking at all aspects of keratoconus, not only the therapies but also the etiologies (see “Causes of Keratoconus”). “There are exciting new fields such as special contact lenses, and ultraviolet light and chemicals to harden the cornea,” he said. “We are now studying molecular genetics and hope to identify people who are predisposed to the condition in an effort to discover and apply preventive therapy.”
______________________________
Dr. Belin reports financial interests in Oculus but none related to products in this story. Dr. Jackson reports interests in Bausch & Lomb but none related to products in this story. Drs. Stark and Steinert report no related interests.