Download PDF
Researchers at the National Eye Institute (NEI) have discovered that the eye has the potential to regenerate the intraretinal immune cells that it needs to keep retinal synapses functioning properly.1
The finding represents the first time that neuroscientists have been able to observe the regeneration of these immune cells, called microglia, directly in a living animal and demonstrate that the repopulated cells can do their normal job within a neural system, said the study’s lead investigator, Wai T. Wong, MD, PhD, at the NEI.
It also suggests that targeted control of these cells might one day allow ophthalmologists to tamp down destructive inflammation in diseased retinas without the use of corticosteroids, Dr. Wong said.
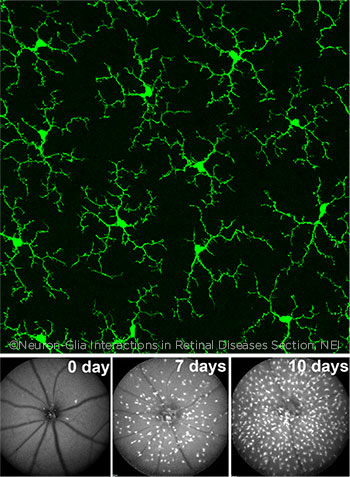 |
RECOVERY. Top: Healthy microglia in an adult mouse retina. Bottom: Mouse eyes after being treated with a drug that nearly eliminates microglia. On Day 0, almost all microglia are gone, except for a few near the optic nerve head. By Day 7, the microglia have migrated across the retina, and by Day 10, they have increased in number.
|
Rethinking neurodegeneration. “In the business of trying to save neurons from dying, people have been trying to directly sustain the neurons,” Dr. Wong said. More recently, however, researchers have recognized that “many diseases in which neurons degenerate actually involve a maladaptive, maladjusted immune system within the brain or retina.”
As a result, “finding ways in which the immune cells behave and can change, as well as discovering the agents that can manipulate them, is a new way of thinking about cures to neurodegeneration,” he explained.
Road to repopulation. In this animal study, Dr. Wong and his colleagues were following up on their own and other scientists’ work showing that microglia in the brain and the retina are essential to synaptic functioning of the neurons. “This is something that is quite recent in the field. We had studied this question a few years ago and found that, in the prolonged absence of microglia, the fidelity of the transmission of the signal between retinal neurons begins to break down. It’s like having a bad electrical connection. You still get some transmission, but the amount is decreased,” he said.
The researchers used the investigational drug PLX5622 (Plexxikon), an inhibitor of the colony-stimulating factor 1 receptor, to almost entirely deplete the microglia in the inner and outer plexiform layers of mouse retinas. When they withdrew the drug 1 week later, the few surviving cells began multiplying and, over subsequent weeks, redistributed themselves across the plexiform layers into the same functional, mosaic arrays that existed before the drug treatment, they reported.
“We were actually able to witness the repopulation process by looking into the eyes of living animals and document it in a video,” Dr. Wong said.2
Looking ahead. Dr. Wong said that reversibility of microglial depletion suggests that targeted delivery of PLX5622 or another drug with similar action might someday be used to temporarily suppress microglia from sending inflammatory signals that would eventually lead to photoreceptor malfunction or death.
However, more research is needed to understand how to time and deliver the treatment in each disease scenario, he cautioned. Because the molecule is not soluble, intravitreal injection would require a special formulation or delivery device, Dr. Wong said. Human research on the drug is limited but ongoing; www.ClinicalTrials.gov lists only 2 PLX5622 clinical studies, both safety trials in patients with rheumatoid arthritis, and the outcomes have not been published.
For now, much research remains to be done, Dr. Wong said. “We were aiming at a proof of concept. So this is a step toward understanding what the retina’s immune system is capable of and how to control and manipulate that for therapeutic purposes,” he said.
—Linda Roach
___________________________
1 Zhang Y et al. Sci Adv. 2018;4(3):eaap8492.
2 See http://advances.sciencemag.org/cgi/content/full/4/3/eaap8492/DC1. (Note: Three movies are toward the bottom of the web page.)
___________________________
Relevant financial disclosures—Dr. Wong: None.
For full disclosures and the disclosure key, see below.
Full Financial Disclosures
Dr. Lee: None.
Dr. Moutray: Bayer: C; Novartis: C.
Dr. Smith: None.
Dr. Wong: None.
Disclosure Category
|
Code
|
Description
|
| Consultant/Advisor |
C |
Consultant fee, paid advisory boards, or fees for attending a meeting. |
| Employee |
E |
Employed by a commercial company. |
| Speakers bureau |
L |
Lecture fees or honoraria, travel fees or reimbursements when speaking at the invitation of a commercial company. |
| Equity owner |
O |
Equity ownership/stock options in publicly or privately traded firms, excluding mutual funds. |
| Patents/Royalty |
P |
Patents and/or royalties for intellectual property. |
| Grant support |
S |
Grant support or other financial support to the investigator from all sources, including research support from government agencies (e.g., NIH), foundations, device manufacturers, and/or pharmaceutical companies. |
|
More from this month’s News in Review