By Sue Vicchrilli, COT, OCS, Academy Coding Executive, and Michael X. Repka, MD, MBA, Academy Medical Director for Governmental Affairs
Download PDF
What do these three pairs of procedures have in common: pterygium excision and cataract surgery; visual fields and blepharoplasty; and gonioscopy and argon/selective laser trabeculoplasty (ALT/SLT)? All are subject to National Correct Coding Initiative (NCCI) edits. This means that when, for instance, you perform pterygium excision and cataract surgery together, you’ll get paid only for one of them—if you submit codes for both, don’t be surprised if you are reimbursed for the one with the lower allowable.
NCCI Overview
The goal of the NCCI is to prevent fraud and promote accurate coding.
CMS publishes pairs of codes, known as NCCI edits, that should not be billed together. Each NCCI edit identifies a pair of services or procedures that typically should not both be billed when performed by the same provider on the same patient on the same day.
CMS publishes NCCI edits as a table of codes. CMS publishes a four-column table that it posts online and updates quarterly. The first two columns list codes (including both CPT and HCPCS codes), the third lists an implementation date, and the fourth lists a single-digit number known as the “indicator.” Each time CMS identifies a new NCCI edit, a new line is inserted into the table.
The two codes in an NCCI edit are “bundled” together. The code that appears in column 1 generally represents the major procedure or service. The corresponding code in column 2 may represent a component of the column 1 code. Consequently, the code in column 2 is generally not payable in addition to the first code because its value is accounted for—or bundled—in the payment for the code in column 1.
NCCI edits are used to review claims prior to payment. Automated claims processing systems can use the table of NCCI edits to review claims for irregularities. All Part B Medicare claims are processed in this way.
How to Use the NCCI Table
For some NCCI edits, CMS allows you to bill both codes—in a process known as “unbundling”—if certain criteria are met. For each edit, see if unbundling is permitted by checking the numeric indicator in column 4.
0 indicates that you cannot unbundle the edit. This is a “mutually exclusive edit.” There are no circumstances in which both procedures of the code pair should be paid. Bottom line: Appending modifiers to the column 2 code when a 0 indicator is present will not bypass the NCCI edit.
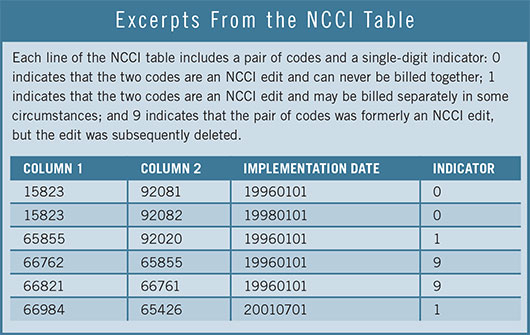
Examples featuring indicator 0. The NCCI table shows that CPT code 15823 Blepharoplasty, upper eyelid; with excessive skin became bundled with CPT codes 92081 Visual fields exam; limited and 92082 Visual fields exam; intermediate on Jan. 1, 1996, and Jan. 1, 1998, respectively. Both edits have an indicator of 0, showing that it is never appropriate to unbundle these tests from the blepharoplasty code when performed on the same date.
1 indicates that there are circumstances in which the edit can be unbundled. The two codes can be unbundled when the column 2 code represents one of the following:
- a different session or patient encounter,
- a different procedure or surgery,
- a different site or organ system,
- a separate incision/excision,
- a separate injury or area of injury in extensive injuries.
When unbundling, use modifier –59. When unbundling is deemed appropriate, modifier –59 Distinct procedural service should be appended to the code in column 2.
Examples featuring indicator 1. The NCCI table shows that CPT code 92020 Gonioscopy became bundled with CPT code 65855 Argon laser trabeculoplasty or selective laser trabeculoplasty on Jan. 1, 1996, with an indicator of 1. Correct claim submission would be CPT code 65855–eye modifier and 92020–59–eye modifier. Payment would be 100 percent of the ALT and 100 percent of the gonioscopy. The rule that there is a 50 percent reduction on the second procedure does not pertain to testing services.
Similarly, the NCCI table shows that CPT code 65426 Pterygium excision with graft became bundled with CPT code 66984 Cataract extraction with IOL on July 1, 2001. The indicator is 1, which means that it can be unbundled. Correct claim submission would be CPT code 66984–eye modifier and 65426–59–eye modifier. Payment would be 100 percent of the allowable for the cataract surgery and 50 percent of the allowable for the pterygium excision with graft.
9 indicates that a former edit has been deleted. In other words, although the two codes were formerly bundled together, that is no longer the case.
Examples featuring indicator 9. The NCCI table shows that the edit for CPT codes 66762 Iridoplasty and 65855 ALT/SLT was assigned an indicator of 9 on Jan. 1, 1996. This means the edit was deleted on that date and both codes can be billed. The table also shows that CMS deleted the edit for CPT codes 66821 YAG and 66761 Iridotomy.
Check for NCCI Updates
Be sure to check code pairs each quarter (in January, April, July, and October). For a link to the CMS edits, go to www.aao.org/coding and click on “Coding Tools,” and then “CCI Edits.”
Coding in Chicago
Got a Coding Conundrum? Bring your queries to the Coding Desk at the Academy Resource Center (Booth 508), where you can chat with AAOE experts and browse the AAOE’s coding resources, such as the Ophthalmic Coding Series and Ophthalmic Coding Coach.
TWO SPECIAL EVENTS. Coding SOS. Enjoy hands-on ICD-10 training. When: Saturday, Nov. 10, 8-11 a.m. Where: Room S105. Access: Register in Hall A for $330.
Coding Camp. An intermediate/advanced workshop. When: Saturday, Nov. 10, 12:30-3:30 p.m. Where: Room S105. Access: Register in Hall A for $270.
NINE INSTRUCTION COURSES. All approved for group A CE credits. When: From Sunday, Nov. 11, to Tuesday, Nov. 13. Where: Rooms S501-S504. Access: Academy Plus course pass required.
ONE FREE PRESENTATION. Physicians + ICD-10: What Can’t Be Delegated. Learn what Eye M.D.s must do differently with ICD-10. Seating will be limited. When: Sunday, Nov. 11, 2-3 p.m. Where: Technology Pavilion (Booth 880). Access: Free.
|