This article is from November/December 2005 and may contain outdated material.
Photophobia is a vexing problem for patients and physicians alike. Although extreme light sensitivity was first described in the 1930s, its origins and management remain elusive even today. But researchers at the University of Utah are working to decipher this troubling and often misunderstood symptom.
“Light sensitivity is a very common problem, and most ophthalmologists—most physicians in general—don’t know what to do with it,” said Kathleen B. Digre, MD, professor of ophthalmology and neurology at the University of Utah in Salt Lake City. “They need to know that this is a real symptom and not a figment of someone’s imagination.”
Dr. Digre noted that the literature is rife with references to psychiatric disease among people complaining of photophobia and with suggestions that photophobia really doesn’t have any pathophysiology.
Co-investigator Bradley J. Katz, MD, PhD, added, “Photophobia is not a psychological problem. It is a neurologic problem, and physicians should take it seriously.”
Two Possible Connections
Because photophobia is a symptom, the key to managing it is to identify and treat the underlying condition. The list of potential causes is long and includes both ophthalmic and nonophthalmic conditions (see “Conditions Commonly Associated With Photophobia”). Iritis, uveitis and corneal disease all produce photophobia, and light sensitivity is a common complaint with dry eye and migraine.
The migraine connection. About 80 percent of people who have migraines have photophobia. It is one of the diagnostic criteria and is considered one of the predictors of the debilitating headaches nearly 98 percent of the time. Migraine sufferers are more sensitive to light between migraine episodes than are other people. Moreover, people who have chronic migraines are more light-sensitive than those who have sporadic migraines. Research has shown that migraine sufferers also have a low threshold of tolerance to loud noises and are more susceptible to motion sickness than are people who do not have migraines.
Although photophobia is not a psychiatric disorder, people with agoraphobia, depression, bipolar disease and seasonal affective disorder are more light-sensitive than are people without these conditions. “In fact, some people can tell how depressed they are by how light sensitive they are,” Dr. Digre noted.
Blepharospasm, too. Photophobia is known to be associated with blepharospasm. In one survey, four out of five blepharospasm patients cited bright lights, television viewing, driving, reading and stress as factors that aggravate their condition.1
In a series of studies reported at North American Neuro-Ophthalmology Society (NANOS) meetings over the last three years, the University of Utah researchers have explored the relationship between blepharospasm and photophobia. In one study, they tested the light sensitivity of 30 people with blepharospasm, 30 people known to have migraines and 30 normal controls. Using a rheostat to measure light intensity, the researchers exposed each study participant to increasing light intensity in 50-lux increments every two seconds. The volunteers were instructed to stare at the light and signal when the light intensity became uncomfortable. The researchers found that the participants with blepharospasm were as light sensitive as those who had migraines, and both were more sensitive than the controls.
Dr. Katz, assistant professor of ophthalmology and neurology at the University of Utah, said that his group also surveyed members of the Benign Essential Blepharospasm Research Foundation about their light sensitivity. “We found that 94 percent of the blepharospasm patients reported some level of light sensitivity and that their light sensitivity made their blepharospasm worse and sometimes triggered spasms,” he said. “They also reported that many activities of daily living, such as walking about, driving, reading, watching television and shopping, were adversely impacted by their abnormal light sensitivity.”
A Constellation of Causes
The mechanisms that cause certain people to experience light as painful have not been well-understood, but neuro-ophthalmologists are beginning to untangle some of the mysteries.
In a presentation at the 2005 NANOS meeting, Dr. Digre highlighted some of what is known about the pathophysiology of photophobia. In addition to the associations with migraine and blepharospasm, these are among the findings about light and photophobia:
- Individual thresholds of light sensitivity vary among most people.
- Light sensitivity may be modulated by seasons, with lower discomfort thresholds in the winter months than in the summer months.
- The total amount of light influences the discomfort threshold. For example, binocular viewing of a light stimulus is associated with a lower discomfort threshold than uniocular viewing.
- Retinal adaptation (dark adaptation, for example) determines the interpretation of light brightness.
- Different wavelengths affect an individual’s comfort level. Some studies have indicated that migraine sufferers experience more discomfort with blue- or red-wavelength light.
- Flickering lights cause discomfort in people with migraines. A photogenic stimulus of 2 to 8 cycles/second has been shown to cause the greatest discomfort among people with migraine or photoinduced epilepsy.
- Certain patterns of light, especially stripes, also cause greater discomfort for people with migraine or photoinduced epilepsy.
- Migraine patients appear to have a hyperexcitable occipital lobe, which increases sensitivity to stimulation by light, sound, odors and touch.
- Light-sensitive individuals may have different levels of photopigments in the retina. People with blepharospasm or migraine, for example, have been found to have higher macular levels of the carotenoids lutein and zeaxanthin, perhaps as protective mechanisms.
Maybe not an “eye” problem? Where does light-induced pain originate? Prevailing theories focus on a connection between the trigeminal system and the retina. “For sure it has to do with the trigeminal system, which is the sensory input for the orbit, the eye, the head and the meninges of the brain,” Dr. Digre said. “The first division of the trigeminal system is intimately involved in light sensitivity.”
She pointed out that vision is not required to have light sensitivity and that light can stimulate the trigeminal nerve in other ways. “Even people who have retinitis pigmentosa and are almost blind have horrible light sensitivity,” she said. “We’re hungry for studies to help us understand this.”
Dr. Katz noted that they are looking at this phenomenon in conjunction with Craig Evinger, PhD, professor of neurobiology and behavior, and ophthalmology, at the State University of New York, Stony Brook.
Dr. Evinger has studied light sensitivity in rats. “Dr. Evinger has shown that sectioning the optic nerve does not eliminate blinking in response to bright light,” Dr. Katz said, “but cutting the trigeminal nerve does eliminate spontaneous blinking in the presence of bright light. These data indicate that it may be the trigeminal system, not the visual system, that is responsible for photophobia.”
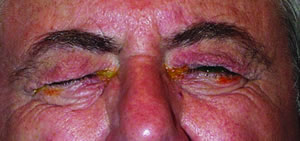 |
| Light sensitivity is often associated with blepharospasm. |
Relief Remains a Challenge
For now, the most important step is to diagnose and treat any associated conditions, and to talk with patients about a few things they can do, including not wearing sunglasses indoors. “People who wear really dark glasses can actually dark-adapt themselves and increase their photosensitivity,” Dr. Digre said. “Sunglasses outside, of course, are fine, but the darker the glasses inside, the more light-sensitive the person will become.”
Rose-colored sunglasses. Preliminary research at the University of Utah suggests that specially tinted lenses may help some people with photophobia. Anecdotally, many photophobic patients prefer an FL-41 tint on their sunglasses instead of green or yellow. The FL-41 tint, which has a pinkish look to it, is a mixture of colors that blocks the blue-green wavelengths.
“We randomized patients with blepharospasm to wearing FL-41 sunglasses for two weeks and then to wearing plain sunglasses for two weeks,” said Dr. Katz. “The patients filled out questionnaires at the end of each period. We found that patients with blepharospasm definitely preferred wearing lenses with the FL-41 tint to wearing conventional sunglasses. So there does seem to be some therapeutic benefit.”
In a new study, the researchers have used electromyography to measure blink frequency, duration and amplitude in blepharospasm patients while they read for five minutes at a time with regular eyeglasses, glasses with a light gray tint or glasses with an FL-41 tint. The results are still being analysed, but Dr. Katz said they appear to provide more objective evidence that FL-41 does reduce blepharospasm.
"FL-41 lenses are noninvasive, they have no side effects and they're not expensive," Dr. Katz added. "So it's a cheap, easy way to improve the lives of these patients, who in some cases are very disabled by their disease."
Be sure glasses block blue-green. FL-41 lenses are available in optical shops, but Dr. Digre cautioned that some so-called FL-41 lenses are not the real thing. "You really have to know who your supplier is in order to know whether the lenses are real or not," she said. "Some lenses can look like FL-41, but they don't act like it. We have done spectral analysis of our lenses to make sure they are blocking the right light."
Where does photosensitivity research go from here? Dr. Katz said more research is needed at the basic science level. "Work with animal models of light sensitivity will help determine the anatomical pathway that controls the sensitivity. Once we better understand the wiring of light sensitivity, we'll be able to treat it better."
____________________________________________
1 Anderson, R.L. et al. Ophthal Plast Reconstr Surg 1998; 14:305-317.
Conditions Commonly Associated With Photophobia
Ocular
- Dry eye
- Corneal diseases
- Uveitis
- Blepharitis
- Conjunctivitis
- Iritis
- Asthenopia
- Keratoconjunctivitis
- Retinal disease (e.g., cone dystrophy, retinitis pigmentosa)
- Vitreous disease
- Optic neuritis
- Papilledema
Nonocular
- Migraine
- Blepharospasm
- Depression
- Head injury
- Meningitis
- Pituitary tumors
- Subarachnoid hemorrhage
|