Download PDF
Conventional wisdom holds that glaucoma treatment may preserve vision but cannot reverse damage. Now, researchers at the Jules Stein Eye Institute (JSEI) at UCLA report that damage may be reversible, at least for some patients following trabeculectomy.1 They found that filtering surgery not only slowed the rate of perimetric decay from glaucoma but also provided evidence of sustained, long-term improvement of visual function.
The implications for clinical treatment are profound. Rather than simply treating glaucoma patients to maintain stability, doctors should understand that long-term improvement of visual function is possible, said Joseph Caprioli, MD, professor of ophthalmology at JSEI. He said that clinicians should begin to “evaluate visual fields in a different way, and not always dismiss apparent improvement as an artifact.”
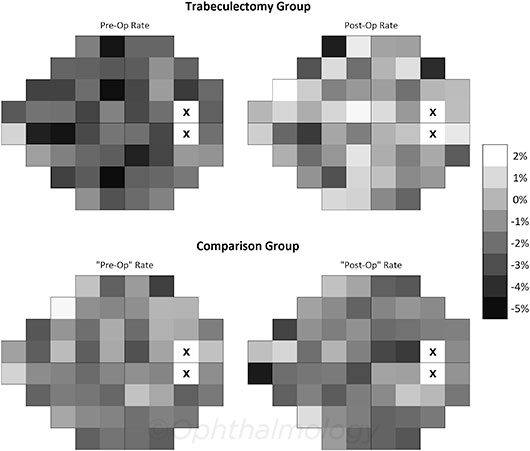 |
VF CHANGE. Distribution of the average rate of change at each location for the 2 groups, comparing the first study period (“pre-op”) and the postop follow-up. The scale shows change in percentage/year; positive numbers indicate improvement.
|
Study design. The retrospective, comparative, longitudinal cohort study involved 2 groups. In the surgery (“Trab”) group, 74 eyes of 64 patients underwent trabeculectomy with mitomycin-C. The comparison group included 71 eyes of 65 patients with open-angle glaucoma who did not have surgery. Baseline damage, number of visual field (VF) tests, and follow-up were similar in both groups.
Patients were followed for about 5 years before and 5 years after surgery. To mitigate “noise” effects, VF tests were acquired at multiple time points before and after surgery.
Key results. “The finding that surprised me the most was that improvement was a fairly common event, if you look for it properly,” said Dr. Caprioli.
Among the findings:
- The magnitude of IOP reduction correlated with the number of VF locations that exhibited long-term improvement postoperatively.
- 80% of Trab eyes improved at 5 or more test locations in the VF.
- More than half of the Trab eyes (57%) showed improvement at 10 or more VF test locations.
Possible mechanism. While medical therapy might also yield VF improvement, “a more dramatic effect can be seen with the kind of robust pressure reduction that one can achieve with trabeculectomy,” Dr. Caprioli said. (Mean IOP fell 32%, from an average of 15 mm Hg preoperatively.)
To explain their findings, the researchers theorize that retinal ganglion cells that are damaged, but not dead, contribute to decreased perimetric sensitivity. Reduction of IOP-related stress after surgery may restore function in these damaged cells. This insight could lead to an approach called neurorescue—novel treatments to revive dying nerve cells.
The researchers will follow these patients to monitor duration of effect. They are also planning studies to help predict which patients would achieve visual gains from treatment.
Clinical implications. In the meantime, Dr. Caprioli has modified his therapeutic approach. “In patients who are not too elderly, do not have too much visual damage, and who have relatively high pressures, I am becoming more aggressive about lowering eye pressure to a level at which some reversal of visual loss occurs.”
He encouraged others to be mindful of the study’s findings. “I would like those physicians who care for glaucoma patients to simply have a mind-set that allows them to believe that sustained improvement of visual function after treatment can occur.”
—Miriam Karmel
___________________________
1 Caprioli J et al. Ophthalmology. 2016;123(1):117-128.
___________________________
Relevant financial disclosures—Dr. Caprioli: Allergan: S; Alcon: S; National Eye Institute: S; New World Medical: S; Research to Prevent Blindness: S.
For full disclosures and disclosure key, see below.
More from this month’s News in Review