By Lindsay K. McConnell, MD, Amit K. Reddy, MD, and Richard C. Allen, MD, PhD, FACS
Edited by Steven J. Gedde, MD
Download PDF
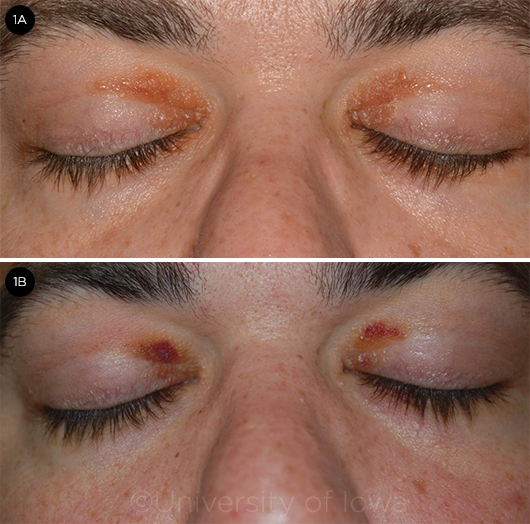
James Cruise* was mystified by the yellow-orange papules on the medial portion of both upper eyelids (Fig. 1A). The lesions occasionally felt irritated, but there wasn’t any discharge or pain. Six months after he had first noticed them, the 37-year-old made an appointment to see his dermatologist. Mr. Cruise—who considered himself to be in good health—was surprised to be told that what he had on his eyelids was probably related to high cholesterol or lipids.
His cholesterol and lipid levels were checked by his primary care provider and found to be within normal limits. He even had them checked a second time, and again they were normal. He was prescribed a topical cream but never filled the prescription due to the cost.
We Get a Look
We saw Mr. Cruise about 6 months after his visit with the dermatologist. Two weeks prior to presentation, he had contracted an upper respiratory infection, and he noticed that the lesions occasionally turned “black and blue.” He brought photos to demonstrate this (Fig. 1B). Sometimes the lesions bled if he rubbed them. He had not used topical creams or ointment on his eyelids and denied any history of trauma to the area. He had no significant medical or ocular history and did not take any medications. No one in his family had a history of similar lesions. He said that he did not use tobacco but did drink socially.
Further questioning. At our visit, Mr. Cruise mentioned that he had been feeling a bit more fatigued than usual over the past 6 months. He had seen commercials on TV about low testosterone and wondered if that could be the cause. During this time, he had unexpectedly experienced a 20-pound weight loss—though he wasn’t complaining; indeed, he said that he could probably stand losing another 10 pounds. He also noted shortness of breath with moderate exertion and swelling in his legs, but he attributed this to a somewhat sedentary lifestyle. He denied fevers, rashes, easy bruising, or new bone or joint pain. Physical and ocular examinations were normal, other than the eyelid lesions.
What further testing revealed. Due to the atypical appearance of the lesions and their history of periodic bleeding/bruising, a biopsy was performed. Pathology revealed numerous paucicellular areas of eosinophilic deposition throughout the dermis. These areas stained positively with Congo red and demonstrated apple-green birefringence with cross-polarization, which indicated the presence of amyloid.
The patient was subsequently referred to the hematology/oncology service for further evaluation. Bone marrow biopsy revealed approximately 20% plasma cells with the presence of atypical cells, leading to the diagnosis of multiple myeloma and lambda light chain disease, which is a monoclonal deposition disease that is highly associated with multiple myeloma. Echocardiography and cardiac magnetic resonance imaging (MRI) showed findings consistent with an infiltrative cardiomyopathy—specifically amyloidosis. (He was susceptible to developing amyloidosis due to the overproduction of abnormal antibodies by the plasma cells.)
 |
|
LESIONS. (1A) The patient had first noticed the yellow-orange papules about 12 months before we saw him. (1B) Approximately 2 weeks before he presented to us, he noticed that they intermittently turned “black and blue.”
|
Discussion
Amyloidosis of the ocular and orbital region is relatively uncommon; one report found that only 4% of head and neck amyloidosis was located in the orbit.1 Two recent case series examined 34 patients who were diagnosed with ocular and/or orbital amyloidosis.2,3 Of the 34 patients, on initial presentation 17 had only conjunctival involvement, 10 had only orbital involvement, 6 had both, and 1 had neither. Conjunctival involvement appears to be associated with localized disease, whereas involvement of the eyelids—as in this patient—is more likely to be associated with systemic involvement.4 Localized orbital amyloidosis has often been treated with surgical excision; however, the diffuse infiltration leads to frequent recurrences.
The exam and history, particularly the report of hemorrhage and bruising occurring at the lesion sites during a recent respiratory infection, are especially concerning for cutaneous amyloidosis. There are multiple reports in the literature of both localized and systemic amyloidosis presenting as periorbital purpura5,6 or subconjunctival hemorrhage. This is suggestive of amyloidosis and is believed to be due to the infiltration of amyloidosis into blood vessels, causing increased fragility that can lead to hemorrhage spontaneously or with increased pressure from a Valsalva maneuver, either of which might have occurred in this patient.
The potential for underlying malignancy highlights the need for increased clinical suspicion in cases of easy bleeding in the subconjunctival or periorbital regions. Biopsy should be performed, and the pathologist should be alerted to look specifically for amyloid. Patients with confirmed amyloid deposition should be referred to a hematologist or oncologist to be evaluated for systemic amyloidosis and hematologic malignancy, in particular multiple myeloma.
Patient Outcome
Following the diagnosis of multiple myeloma, the patient received D-PACE induction chemotherapy followed by autologous stem cell transplant and a second autologous stem cell transplant 3 months later. Maintenance chemotherapy was initiated 6 weeks after the second transplant.
___________________________
* Patient name is fictitious.
___________________________
1 Gean-Martin AD et al. Radiol. 1991;181(2):521-525.
2 Al-Nuaimi D et al. Orbit. 2012;31(5):287-298.
3 Leibovitch I et al. Ophthalmol. 2006;113(9):1657-1664.
4 Nielsen NS et al. J Proteomics Bioinform. 2014;S8:002.
5 Lee H et al. J Dermatol. 2008;35(6):371-372.
6 Goldstein DA et al. Cornea. 2005;24(6):757-758.
___________________________
Dr. McConnell is a resident at the Department of Ophthalmology and Visual Sciences at the University of Iowa Hospitals and Clinics in Iowa City, Iowa. Dr. Reddy is starting an ophthalmology residency this year at the University of Colorado. Dr. Allen is professor at the Section of Ophthalmology in the Department of Head and Neck Surgery at the MD Anderson Cancer Center in Houston. Relevant financial disclosures: None.