Download PDF
Topical therapy may be able to close small secondary macular holes and potentially eliminate the need for surgery.1
Study specifics. This retrospective analysis involved nine cases of topically treated, secondary full-thickness macular holes (FTMH). Eight of the eyes (89%) had successful hole closure and resolution of their associated cystoid macular edema. The hole in the ninth eye, in a patient with topically treated bilateral holes, did not close after six weeks of topical therapy, and the patient was then lost to follow-up.
All patients received corticosteroid drops (difluprednate ophthalmic emulsion 0.05%). Six eyes also received a topical carbonic anhydrase inhibitor (dorzolamide 2% or brinzolamide 1%), and two eyes received a nonsteroidal anti-inflammatory drug (bromfenac 0.07%). The average initial hole diameter was 79.6 μm (range, 44 to 132 μm), and the average time until closure was six weeks (range, two to 19 weeks).
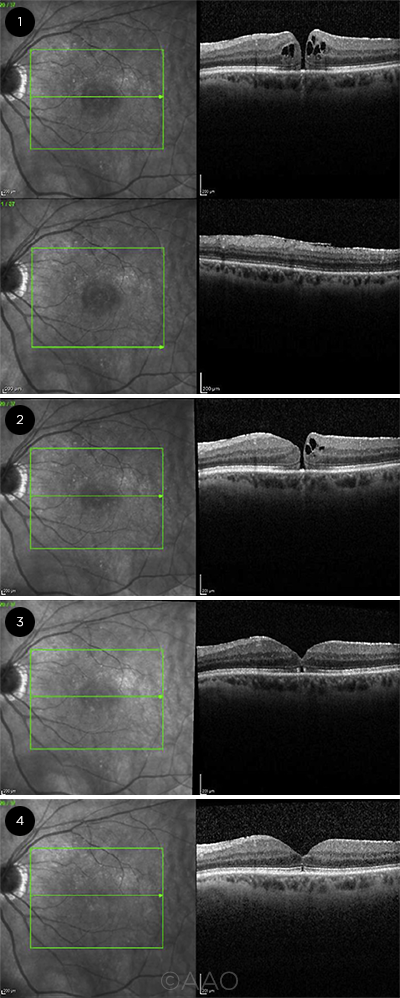 |
OCT SEQUENCE. (1) Cystoid macular edema, high retinal surface reflectivity from epiretinal membrane, and a FTMH. The patient was started on difluprednate three times daily. (2) At four weeks, the hole is closed, and the drops are reduced to twice daily. (3) At 22 weeks, the hole remains closed, the outer retinal break is decreased, and treatment is discontinued. (4) At 81 weeks, the hole remains closed without drops.
|
A paradigm shift? “The standard of care for primary macular holes caused by vitreomacular traction is vitreoretinal surgery,” said coauthor John Niffenegger, MD, at Retina Associates of Sarasota, Florida. “In cases of small holes (<250 μm) that are secondary to something other than vitreomacular traction, patients often would like to avoid surgery, and interest in addressing their problem with topical therapy has been increasing.”
The outcomes of this study support a role for comprehensive ophthalmologists to consider medical therapy for patients who have small, secondary macular holes, Dr. Niffenegger said. “With spectral-domain optical coherence tomography fairly available now, it’s easier for a comprehensive ophthalmologist to determine the hole’s size and etiology,” he said. “So, in the absence of vitreoretinal traction, it would be reasonable for them to consider a trial of topical therapy as they refer the patient for vitreoretinal consultation or await scheduling for macular hole surgery. You might be able to spare these patients the expense and possible complications of surgery.”
—Linda Roach
___________________________
1 Niffenegger JH et al. Ophthalmol Retina. Published online Jan 28, 2020.
___________________________
Relevant financial disclosures—Dr. Niffenegger: None.
For full disclosures and the disclosure key, see below.
Full Financial Disclosures
Dr. Mainster Ocular Instruments: C.
Dr. Menko None.
Dr. Niffenegger None.
Dr. Tonorezos This study was supported by the National Cancer Institute’s Intramural Research Program, a Sloan-Kettering Institute of Cancer Research Cancer Center Support Grant (P30CA008748), and the Meg Berté Owen Fund. The funding sources had no role in the study design, data acquisition, analysis, manuscript preparation, or decision to submit this work.
Disclosure Category
|
Code
|
Description
|
| Consultant/Advisor |
C |
Consultant fee, paid advisory boards, or fees for attending a meeting. |
| Employee |
E |
Employed by a commercial company. |
| Speakers bureau |
L |
Lecture fees or honoraria, travel fees or reimbursements when speaking at the invitation of a commercial company. |
| Equity owner |
O |
Equity ownership/stock options in publicly or privately traded firms, excluding mutual funds. |
| Patents/Royalty |
P |
Patents and/or royalties for intellectual property. |
| Grant support |
S |
Grant support or other financial support to the investigator from all sources, including research support from government agencies (e.g., NIH), foundations, device manufacturers, and/or pharmaceutical companies. |
|
More from this month’s News in Review