27-year-old woman has pain and blurry vision after not removing her contacts for days.
Cataract/Anterior Segment
What is your diagnosis?
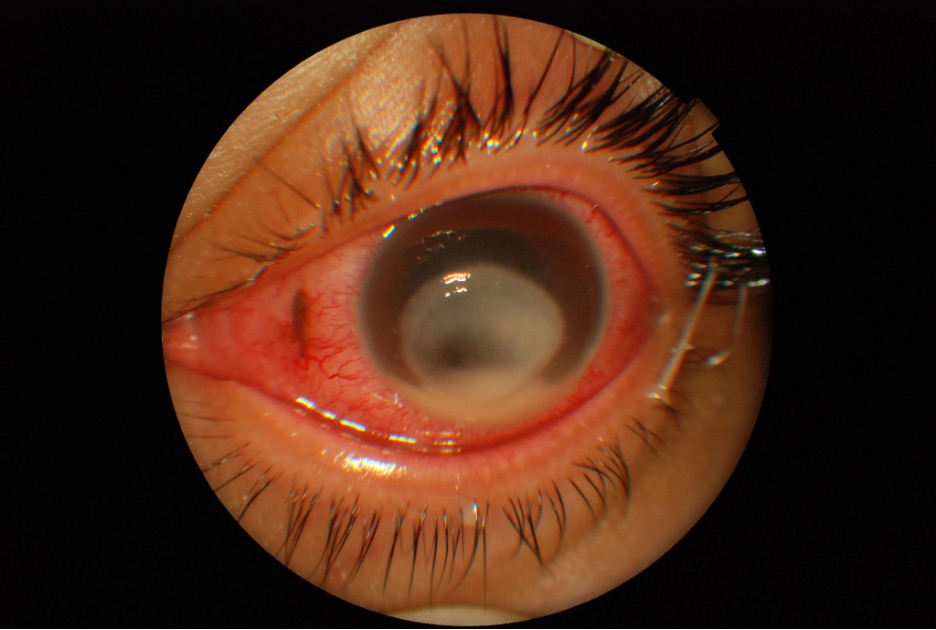
The diagnosis is...
![]()

The image is consistent with a diagnosis of corneal ulcer.
- Corneal ulcers typically result from trauma associated with contact lens or injury.
- Corneal ulcers may be caused by bacteria, fungi, or parasites.
- Risk factors include extended-use contact lenses and diseases affecting proper closure of the eyelids (causing exposure), such as Bell palsy, Graves ophthalmopathy, and being a patient who is post stroke.
- Patients sedated for extended periods of time, such as those in the intensive care unit (ICU), are at a higher risk of developing a corneal ulcer.
What is the role of the primary care or emergency medicine physician?
![]()
Corneal ulcers may become an ophthalmic emergency due to the potential for permanent damage or vision loss resulting from a
perforated globe or scarring of the corneal surface.
- Because of the urgency of corneal ulcer treatment, primary care and emergency medicine doctors should obtain a focused history including symptom onset and promptly refer patients to ophthalmology for further management and evaluation.
- Emergency medicine doctors could be asked to perform an eye examination. If a small ulcer is seen, they could initiate antibiotics and then refer patients to ophthalmology.
What is the role of the ophthalmologist?
![]()
Managing corneal ulcers can be challenging.
- Begin empiric treatment with antibiotics, such as 4th-generation cephalosporins, or fluoroquinolones, to prevent expansion of the ulcer and corneal scarring.
- Gently swab the corneal surface to obtain a sample to send for speciation (bacterial, fungal, parasitic, viral keratitis) and susceptibility.
- Treatment with steroids may also be involved.
What is the treatment?
![]()
- If there is high suspicion for a bacterial ulcer, initiate broad-spectrum antibiotics.
- Steroids may be used to prevent inflammation and scarring of the corneal surface, but they should not be used if the ulcer is due to a fungal infection, or they should be used cautiously if the pathogen is unknown.
- Other causes of ulcers are fungi, parasites, and viruses.
- Supportive measures include frequent artificial lubrication and shielding the cornea.
- If the ulcer perforates, tissue glue can be used. Delay corneal scar revision therapies to allow resolution of infection.
- If the ulcer is severe enough, a corneal transplant may be recommended. During a corneal transplant, all or part of the damaged cornea is replaced with healthy tissue from a donor.
Learn more: Ophthalmology resources for medical students
![]()