By Galton Vasconcelos, MD; Luciene C. Fernandes, MD
Definition
Low-vision devices are designed to improve visual performance in children with low vision, thus enabling academic and social adaptation and providing enrichment of daily experiences.1,2 They can be optical or optical and electronic.
Types of Devices
Optical
When conventional lenses do not provide required visual range, aids that have optical properties capable of promoting better visual performance through lenses are indicated.2
Types of optical aids for
- Distance
- Intermediate distance
- Near
Optical Aids for Distance and Intermediate Distance
The telescopic system (TS) or telescope is an optical instrument that improves the resolution of an object by increasing the size of the image projected on the retina, making it closer. (Faye, 1984). It is available for far, near, and middle distances (Figure 1).
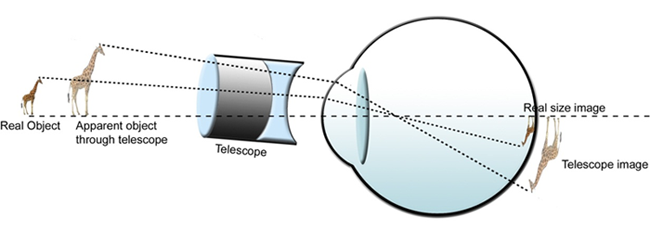
Figure 1. Telescope for distant view.
A telescope enables greater participation in daily and social activities such as watching television and reading white boards, street signs, house and building numbers, billboards, and menu boards. On the other hand, restriction of visual field and illumination, difficulty in locating and focusing on objects quickly, and limited focus depth are disadvantages of the telescopes. Telescopes are not universally accepted due to expense, difficulty in using the devices, and asthetic considerations. Good coordination and training are essential.1–3
Types of Telescopes (Figure 2)
- Galilean or Keplerian
- Hand-held, spectacle-mounted, or clip-on
- Monocular or binocular
- Fixed focus, focusable telescope, or autofocus

Figure 2. Telescopes for distance, near, and middle distance.
Galilean Telescope
The Galilean telescope is a simple system consisting of 2 lenses:
- Objective lens: convex (plus) lens, closest to the object
- Ocular lens: minus lens, closest to the eye
The distance between the 2 lenses is determined by the difference in their focal lengths. The image produced is real and erect. It's lighter, shorter, and cheaper than the Keplerian type, thus the first-choice prescription for children. It is also the first choice in cases of peripheral field loss; in these cases, the lens order is designed in reverse (plus lens closer to the eye), providing a wider visual field.
Keplerian Telescope
Also known as astronomical or prismatic, the Keplerian telescope is an optical system that uses 2 convex (plus) lenses, the objective lens being of smaller diopter power than the ocular. The distance between the lenses is the sum of their focal lengths. The image is real and inverted, requiring a prism to reverse the image, making it longer and heavier. It produces greater visual field and better optical quality than Galilean type and costs more.
Hand-Held, Spectacle-Mounted, or Clip-On Telescope
A hand-held telescope is simpler, lighter, and cheaper than the Galilean and Keplerian types. It is particularly indicated for short activities and could be a first prescription choice for children (Figure 2).
A spectacle-mounted telescope leaves the hands free. It is useful for prolonged activities and activities that require visualization of details. However, they both weigh and cost more
The clip-on model has the advantages of both: It is lighter than the spectacle-mounted model, however, it can scratch the lenses and reduce the visual field to further distances.
Monocular or Binocular
A monocular telescope is indicated when there is a significant difference in visual acuity (VA) between the 2 eyes. It is more discreet, lighter, and cheaper. It can be used in the dominant or better-seeing eye. Binocular telescope is indicated when there is similar VA in both eyes, with the purpose of increasing the visual field, and for nystagmus. The binocular style both weighs and costs more than monocular (Figure 2).
Fixed-Focus, Focusable, or Autofocus Telescope
A fixed-focus telescope is indicated for children with poor motor coordination. Nowadays it is rarely prescribed; a focusable telescope reaches far, near, and intermediate distance and is preferred for and by children. The autofocus telescope both weighs and costs more and it does not constitute the first choice prescription for children.
Optical Aids for Near Tasks
Children, especially in the preschool age group, tend not to complain about their difficulty with near tasks. With adequate accommodation by getting closer for small print, they can read without a problem. However, as school activities get more sophisticated and the fonts of reading material get smaller, greater magnification is required and objects are brought too close, making reading more fatiguing. When and if this becomes an issue, near aids can be beneficial.
Near low-vision aids:
- High-plus spectacles (microscopes)
- Hand-held magnifier
- Stand magnifier
- Telescope system for near (telemicroscope)
High-Plus Spectacles (Microscopes)
High-plus spectacles are convex (plus) lenses mounted in a spectacle frame (Figure 3). They provide maximum magnification when objects are positioned at or near the focal distance of the lens, producing parallel rays and the image forming at optical infinity (Figure 4).2,3

Figure 3. Optical aids for near tasks.
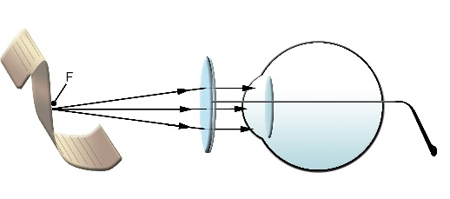
Figure 4. High-plus spectacles working distance.
Advantages:
- Familiarity
- Both hands free
- Greater visual field
- Greater comfort for prolonged reading
- Can be prescribed binocularly by adding up to 10 diopters
- Can be implemented with other aids
Disadvantages:
- Fixed optical center makes adaptation on eccentric vision difficult.
- Reduces visual field in high-power lenses and obstructs light at closer distances
- Often not well-accepted in children with sufficient accommodation; however it is a good option for patients with aphakia or pseudophakia.
Hand-Held Magnifier
Hand-held magnifiers are either convex (plus), convex sphere, or aspheric lenses with a handle that allows them to be held in various positions (Figure 3). They increase the size of a retinal image and bring the image into focus, producing a virtual and erect image located in a distance greater than the focal length of the lens. Hand-held magnifiers provide maximum magnification when an object is standing at or close to its focal distance, producing parallel rays and the image forming at infinity optically (Figure 5).
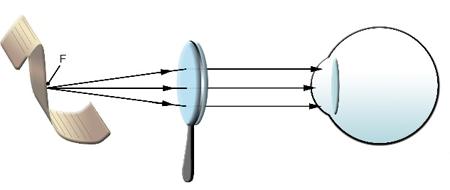
Figure 5. Hand-held magnifier at appropriate working distance.
The distance of the hand magnifier away from the object needs to be at the focal length, to supply maximum magnification. The distance between the observer and the magnifier can vary; the higher the distance, the smaller the visual field will be. Variable eye-lens distance is an advantage when used by patients with constricted field, making this the preferred aid for those with eccentric fixation and those with a visual field less than 10 degrees. The device can be illuminated. It offers a better working distance compared to microscopes and is useful for short duration of reading such as price tags and phone numbers. However, it presents some disadvantages such as a smaller field of vision and lower reading speed compared to glasses, occupation of the hands, and difficulty of maintaining focus. These disadvantages restrict its use in children or in patients with poor motor coordination.
Stand Magnifier
Stand magnifiers are convex (plus) lenses designed with a rigid mounting placed close to the object (Figure 3). Rays emerging from the stand are not parallel, but divergent, requiring accommodative effort or a moderate reading aid to bring the image into focus (Figure 6).2 The device can be illuminated. It is the aid of choice for patients who cannot hold a lens or tolerate the distance of microscopes. Because of the fixed focus, stand magnifiers work well for children. The focal length is determined by the height of the support. If the object is positioned at a distance less than the focal length, the image is formed at a finite distance from the eye and the patient needs to use accommodation or might require corrective glasses for near. It provides a smaller visual field when compared to a microscope and requires good hand-eye coordination.
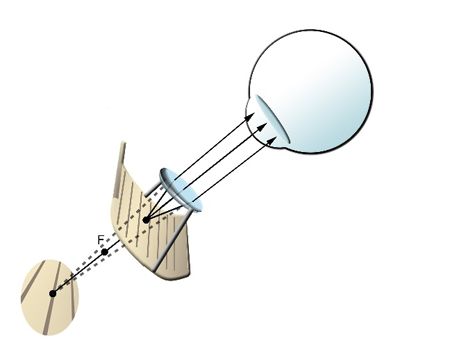
Figure 6. Stand magnifier: Divergent rays come from the lens.
Telescope System for Near (Telemicroscope)
Telescope systems for near, or telemicroscopes, are distance telescopes that can be focused from infinity to near range or that can be modified by putting a reading cap over a distance unit (Figure 2). Telemicroscopes usually are more difficult to use because of their smaller visual field, critical depth of focus, and the apparent displacement of the material to be viewed. However, they allow students to perform tasks at a greater distance than spectacles or hand magnifiers at the same power. A binocular prescription might be possible for adds more than 12 D. However, the reduction of visual field, lighting, depth of focus, weight, and aesthetics restrict the acceptance by a child.1–4
Nonoptical
Nonoptical aids are visual aids that do not use magnifying lenses to improve visual function.2 They can improve the other visual aid's function or can even replace optical aids. They enhance visual function by
- Linear magnification
- Lighting control
- Enhanced contrast
- Reduction of glare
- Improving physical comfort (accessories)
Linear Magnification
Relative size or linear magnification is magnification brought about by enlarging the object itself. This can be done with many kinds of objects, perhaps the most familiar being large-print books, newspapers, and magazines. (Figure 7).
Formula
Ms = S/S'
Ms = Relative size magnification
S = Enlarged print size
S' = Size of the original print
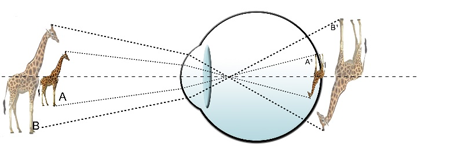
Figure 7. Relative size magnification.
Large print permits unrestricted fields of view and allow more normal working distances and greater speed of reading than optical aids. It is especially useful for preschool children or a child in the early stages of training with low-vision aids. It can be used with other methods of magnification, requiring a lower final power for the chosen optical aid. However, few books are available in large print, they are more expensive, and they are larger and heavier than standard print, sometimes expanding from a single volume to multiple. This makes their handling and transport difficult.
Lighting Control
Lighting necessity varies for every individual and depends on the diagnosis and extent of pathology. Diseases such as aniridia, achromatopsia, and albinism require low-level lighting; glaucoma, retinitis pigmentosa, optic atrophy, and nuclear cataract require high illumination.
Natural light is the adequate lighting for most low-vision children; however, artificial light allows better control of illumination. Incandescent light of 60–75 watts is preferred because it provides a more continuous spectrum than fluorescent light, but might be harder to find, particularly in the United States where some states have banned incandescent lighting. Fluorescent light emphasizes the "cooler" blue spectrum, which can intensify glare. Everyone, even those without low vision, should avoid single-tube fluorescent lamps without a diffuser because they are intermittent, and can cause eyestrain and inhibition of accommodation.
The light should be shone directly on the reading material, avoiding reflective surfaces. The focus should be placed at shoulder height corresponding to the better-seeing eye, forming a 45‑degree angle with the visual axis. When using natural light, the child should sit with their back to the window or on the side leading to the best lighting and visualization.
A typoscope, caps or visors, side shields, and/or polarizing lenses should be prescribed to control the reflection of light. A typoscope can also be used as a guide to reading, writing, and signature in cases of large defects of visual field (Figure 8).

Figure 8. Typoscope and yellow filter.
Light-filtering lenses are useful and frequently prescribed. They should filter ultraviolet radiation below 400 nm, minimizing the loss of VA and color discrimination. It is important to consider comfort; protection from ultraviolet, infrared, and visible light; increased contrast; and glare reduction.
Several factors should be considered when choosing a filter: lens color, photochromaticity, optical density, polarization, and spectrum of protection. The filters can be adapted in glasses, clip-ons, or contact lenses.4
Different filters can be prescribed for different situations, paying close attention to the goals to be achieved, levels of lighting, cost, and especially the individual preference.
Enhanced Contrast and Reduction of Glare
Lighting control is of great importance to enhance contrast and reduce glare. The type, position, and intensity of the light source should be monitored. Absorptive lenses in yellow for low-light environments and amber for more intense lighting are good prescription options. It is also important to support daily activities with aids such as black felt-tipped pen, bold lines, and contrasting colors.
Accessories to Improve Physical Comfort
For a better acceptance and adaptation to the optical aid, physical comfort is key. An inclined board set at a 45‑degree angle can be of help.
Electronic
Assistive technology is an interdisciplinary field of knowledge comprising products, resources, methodologies, strategies, practices, and services that promote functionality for visually impaired people with regard to autonomy, quality of life, and social inclusion. High-tech aids are increasingly of benefit to people with low vision.
Electronic devices include video magnifier systems, closed-circuit televisions, Bluetooth connections to smart projectors, large-print computer programs such as Zoom Text, screen readers such as Virtual Vision and Jaws, and computer tablets.
Electronic devices can be very helpful in moderately or severely visually impaired children and in children who do not respond to other proposed aid. A computer and a tablet can be a good option for a multihandicapped child.
Different electronic devices are currently available:
Video Magnifier System
A video magnifier system consists of a monitor and a camera that projects the enlarged image on the screen. Advantages are higher reading speed (2.5 times) and greater working distance (3 times) when compared to other aids. The larger working distance makes it easy to use for writing, drawing, or painting. It provides additional visual field, brightness, contrast, and polarity control, making it the choice for diseases with low contrast and glare. It allows magnification of 2 to 60 times and binocular vision. It can be fixed or portable, black and white or color, mouse or tray, and fixed-focus or autofocus, allowing objects to be seen at various distances (Figure 9).

Figure 9. Video magnifier system.
A video magnifier system requires coordination and training, but it is the only aid that effectively improves contrast and residual vision and it is well indicated for
- Greater working distance
- Prolonged and less tiring reading
- Allows contrast to be reversed
- Glare
- Large visual-field defects (less than 5 degrees)
- Low response to contrast
- VA less than or equal to 20/800 or better than 20/800
Visual Functions
VA directly influences the successful rehabilitation with optical aids. They are indicated for those with a visual acuity of 20/200 or better. When large magnifications are required it is recommended to start with a telescope system (TS) with lower magnification,
The visual field (VF) has a great influence on the telescope adaptation. For eccentric viewing educational training of the TS must be performed before prescription. For those with concentric VF loss, mainly for VF less than 5 degrees, aids should be prescribed with caution. The patient will have difficulty localizing and tracking objects when there is a central or paracentral scotoma with normal peripheral vision or scotomas above the fixation area.
In cases of low contrast, adaptation to the device can also be more difficult. Early use during childhood leads to better acceptance compared to teen years and beyond.1,2
Why to Prescribe
The prescription of low-vision devices gives the child
- Independence
- Increased adaptation to the daily activities materials
- Exposure to enriching experiences
It constitutes an important factor for socioeconomic and cultural integration.
How to Prescribe
A careful clinical history is important to setting goals based on real expectations. A child who participates in selecting the aid is more likely to learn how to handle it.1,2
How to Prescribe Optical Devices
- Determine the best corrected VA for near/distance.
- Determine the VA that the patient requires.
- Calculate the magnification needed to achieve the goal:
It is important to consider that with VA of 20/50 (0.5 logMar) the child can perform most of the daily tasks. In this way, the Kestenbaum rule can be applied, in which the magnification is given by the inverse of the VA in diopters (A = 1/VA). To achieve the power of hand or stand magnifiers and telescopes: divide the value found in diopters by 4 (unit of magnification), for example:
VA = 20/200
A = 200/20 = 10 D/4 = 2.5X
When you have a defined goal, the magnification proposed can be achieved by dividing the desired VA for the observed VA, for example:
VA = 20/160, desiring to achieve 20/20
A = 160/20 = 8X
- Select the aid according to the characteristics of the device: the needs, goals, and clinical aspects of the patient.
To achieve better acceptance of any aid, consider the child's needs, goals, and ability to handle the aid, as well as the esthetics, weight, cost, and timing of the prescription. It is important for the child to be comfortable with the aid proposed.
For reading activities, besides achieving vision for a certain size of optotype, the child should be evaluated for reading. In the presence of eccentric fixation or difficulties with the proposed aid, training should precede prescription.
Each category of visual device has its advantages and disadvantages. In low-vision daily practice, it is common for a child to have more than one aid.5
The patient should be monitored frequently to evaluate the effective use of the aid prescribed and difficulties presented in daily activities and to set up more advanced goals.
When to Prescribe
Optical aids for near vision are introduced when the reduction of the distance between the object and the eye does not allow the necessary range or when the accommodative effort is too large.
At school age, with VA up to 20/200, reducing the distance between the object and the eye is recommended until the second grade. From this stage, a stand magnifier or a hand magnifier can be used for reading small-print books such as dictionaries (Figure 10).
For VA less than 20/200 (0.1 logMar), optical aids should be prescribed earlier. If the VA is less than 20/400 and the central scotoma greater than 30 degrees, a video magnifier is indicated.
For VA equal to or less than 20/800 aids such as Braille and computer sound systems should be included, with or without other resources. Orientation and mobility techniques should be encouraged at all low vision levels.

Figure 10. A child using a stand magnifier.
When a TS is first prescribed, a manual, monocular telescope with lower magnification is recommended (Figure 11). The telescope can be prescribed for reading blackboards, and later, to use more constantly at far. It is important to let the child experiment with the TS in different situations.

Figure 11. A child using a telescope.
References
- Sterns GK, Hyvarinen L. Adressing Pediatric Issues. In: Fletcher DC. Low Vision Rehabilitation: Caring for the Whole Person. American Academy of Ophthalmology. 1999. 107‑119.
- Faye EE. Clinical Low Vision. 2a. Ed. Boston/Toronto: Little, Brown, and Company. 1984.
- Watson GR. Using Low Vision Effectively. In: Fletcher DC. Low Vision Rehabilitation: Caring for the Whole Person. American Academy of Ophthalmology. 1999. 61‑87.
- Hyvarinen L, Jacob N. What and How Does this Child See? Assessment of Visual Functioning for Development and Learning. Helsinki, Finland: Vistest Ltd. 2011. 174.
- Colenbrander A, Liegner JT, Fletcher DC. Enhancing Impaired Vision. In: Fletcher DC. Low Vision Rehabilitation: Caring for the Whole Person. American Academy of Ophthalmology. 1999. 49‑59.