By Annie Stuart, Contributing Writer, interviewing Ahmad A. Aref, MD, MBA, Steven R. Sarkisian Jr., MD, and Jeremy B. Wingard, MD
Download PDF
In March 2020, the FDA approved the bimatoprost implant Durysta (Allergan). The device delivers a prostaglandin analog, for reduction of intraocular pressure (IOP) in patients with open-angle glaucoma and ocular hypertension.
“It’s the first sustained-release therapy approved for this purpose,” said Ahmad A. Aref, MD, MBA, at the Illinois Eye and Ear Infirmary in Chicago. “Given once as an intracameral injection, it slowly elutes within the eye over a long period of time.”
Here’s an overview of how it works, how it compares with eyedrops, and who might benefit most from this recent arrival.
 |
|
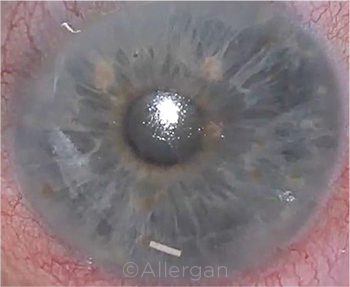
PLACEMENT. Injection can be done at the slit lamp or using an operating microscope, with the patient lying back.
|
Delivery and Duration
Implanting Durysta is not a highly complex procedure, said Jeremy B. Wingard, MD, at the Wheaton Eye Clinic in Wheaton, Ill. “Anyone who does cataract surgery or other glaucoma procedures won’t struggle with the technical aspects of it.”
Tips for delivery. The surgeon may choose to give the injection at a slit lamp or use an operating microscope with the patient lying back, said Dr. Wingard. “I’ve chosen the slit lamp, which works better logistically for me and helps the implant to fall downward into the inferior angle since the patient is sitting upright.”
Durysta comes as a prepackaged cartridge with a button on one end and a needle on the other. “After prepping the patient’s eye with antiseptic solution in a sterile office or operating room setting,” said Dr. Aref, “the surgeon inserts the needle through the cornea before depressing the button to release the implant into the anterior chamber.”
To prevent leakage when you remove the needle from the anterior chamber, it’s best if the track you take through the cornea is long, said Dr. Wingard. “If you go in far enough, and wait a few seconds after the implant is released, the Durysta will fall away from the needle into the inferior angle, putting it where it needs to go, instead of potentially following the needle to the corneal wound.”
How it works. Durysta has the same mechanism of action as the topical bimatoprost eyedrop, said Dr. Aref. Both lower IOP by increasing outflow of aqueous humor through the trabecular meshwork and uveoscleral routes.
“Durysta is designed to release the drug over four to six months,” said Dr. Aref. In the phase 1/2 trial, however, 40% of patients didn’t need retreatment for up to 12 months and 28% of patients for up to two years.1 “We know the drug is not eluting at that point,” said Dr. Wingard, “so the hope is that a change in the eye, perhaps to either the conventional or uveoscleral outflow pathway, is aiding in pressure control over a longer term. This finding will need to be confirmed with a larger number of patients in ongoing studies.”
Single administration. The FDA approved Durysta for one injection only, which is not ideal, said Dr. Aref. “As we start to get more experience with it, labeling could eventually change to accommodate repeat administration.”
However, FDA approval is different from what surgeons are allowed to do. “If a patient needs a second administration, the surgeon can offer it—whether that’s six, 12, 18, or 24 months after the first injection,” said Steven R. Sarkisian Jr., MD, at Oklahoma Eye Surgeons in Oklahoma City. “If the doctor feels it is necessary, that is something I hope will be paid for by insurance.” Whether payers will be on board for multiple injections remains to be seen, said Dr. Wingard.
Durysta Versus Eyedrops
Durysta lowers pressure in the range of what you would expect from a prostaglandin, said Dr. Sarkisian. “It’s variable, but the average is a 30% to 35% drop.”
Benefits. “Durysta gets around a lot of the challenges that conventional eyedrops pose for our patient population—especially with adherence,” said Dr. Aref. And, when given as an injection, bimatoprost doesn’t get absorbed into the fat tissue around the eye and cause the sunken-in appearance that eyedrops can cause, he said. “Once my patients are off their drops,” added Dr. Sarkisian, “their eyes almost universally feel better.”
Costs. In a cost-benefit ratio, is a patient better off getting a Lumigan eyedrop or Durysta? That depends on their insurance, said Dr. Wingard. “For comparison, though, the cost of Durysta is in line with that of Lucentis and Eylea, which are widely used for retinal diseases.”
Adverse effects. During the first day or so, many patients will have redness from the injection and Betadine prep, said Dr. Wingard. “But from my experience,” added Dr. Sarkisian, “if a patient gets chronic conjunctival hyperemia, it’s significantly less than with topical administration.”
As with eyedrops, Durysta can cause permanent changes in iris color, said Dr. Aref. “You need to prepare the patient for this.”
In the phase 3 trials,2 another potential effect with repeat treatments was loss of corneal endothelial cells, he said. “However,” said Dr. Sarkisian, “none of the patients in the study lost vision or needed a corneal transplant due to endothelial cell loss.”
Patient Selection
Each of the doctors has a slightly different take on Durysta’s potential niche in glaucoma management.
For one-time episodes? Given that the FDA approved Durysta for a single administration only, Dr. Aref will consider using it in situations where eye pressure rises temporarily. “For example, eye pressure often goes up after ocular surgery, from surgical manipulation, or from eyedrops prescribed after surgery,” he said.
He would also consider using Durysta in patients treated temporarily with steroids, which can elevate eye pressure—whether given as an eyedrop, a cream, or a pill, or even as a nasal spray for allergies. “In addition, many patients with coexisting conditions get injections of medications into the back of their eyes for treatment of macular degeneration or retinal vein occlusion, which can cause the eye pressure to go up significantly,” he said. “Durysta would help to blunt that.”
Broad inclusion criteria. Dr. Wingard has a different approach. “The ARTEMIS phase 3 trial was broad in its inclusion criteria, so the labeling is very broad, giving approval for adults with open-angle glaucoma or ocular hypertension.” He noted that this gives practitioners wide latitude for deciding on patient selection for Durysta.
In brief, the implant offers practitioners another potential solution to consider, similar to others that have come before, such as Rhopressa and selective laser trabeculoplasty (SLT), he said. “That’s where the value lies. When you get to the clinic and don’t have another better option, you can suggest this and describe how it works. With experience, you will figure out where in your paradigm of treatment this fits.” For Dr. Wingard, though, the most “straightforward” Durysta patients are those who cannot tolerate drops or who take eyedrops for a variety of reasons. Some will also be candidates for SLT.
After SLT. Dr. Sarkisian, in fact, prefers SLT as a first-line option. “But if a patient has Medicare and needs to lower pressure after SLT, Durysta is my first choice before starting an eyedrop,” he said, adding that patients are losing vision because practitioners are in denial about patients’ lack of adherence with drops. “This is such a minimally invasive treatment that we need to consider it before putting someone on an eyedrop.”
Potential contraindications. Patients with high IOP or angle-closure glaucoma are not really appropriate for Durysta, said Dr. Sarkisian. In addition, said Dr. Aref, anybody with an active eye infection or active inflammation would not be a candidate. “Those who’ve had a prior corneal transplant surgery or who have risk factors for corneal decompensation, such as patients with Fuchs endothelial dystrophy, would also want to stay away from this procedure,” he said.
If a patient lacks a good barrier between the front and back of the eye —such as following a complicated cataract surgery—that would increase the risk of the implant entering the posterior part of the eye, said Dr. Aref. Another contraindication is any patient who is at high risk for macular edema, said Dr. Wingard. He pointed out that topical medications can increase this risk, too, but that it’s easier to stop eyedrops than to remove the Durysta implant.
Patient Experiences
“I’ve done about five to 10 cases a week since Durysta became available,” said Dr. Sarkisian, “and it’s amazing how many patients call it a godsend. These are patients who either can’t afford the medicine or are very intolerant to it or they can’t see the bottle.”
Repeat performances. Some hear the word injection and become very anxious, Dr. Sarkisian said, but after the first injection, patients say, “You’re done already?” or “Is that it?” and they invariably come back for the second injection in the other eye, if needed.
Results. Dr. Wingard has treated a handful of patients since Durysta became available. “As of now, it’s been uniformly successful in my patients, with good pressure control several weeks out,” he said, cautioning that he doesn’t expect that to be true for all patients going forward. He noted that although Durysta’s effect on IOP will likely last for months in most patients, eventually the effect is expected to wane.
Case studies. One 97-year-old couldn’t tolerate eyedrops due to extremely thin skin that reacted drastically to every drop Dr. Wingard tried. She was actively losing vision with her central vision being threatened. She had already failed SLT and couldn’t come off her blood thinners to have surgery. “She got a great response with Durysta, with her pressure dropping from about 27 mm Hg to 15 mm Hg over the first two weeks postinjection,” said Dr. Wingard.
Dr. Wingard inherited another patient who had been on timolol. “He came in with pressures in the mid 20s, and the OCT showed the optic nerve worsening,” he said. “I told him, ‘We can put you on another eyedrop, do SLT, or try this new injection that just came out.’” The patient opted for the injection, explaining that he preferred a less intensive eyedrop regimen. His pressures are now around 16 mm Hg in both eyes, which were treated at separate times with Durysta.
A third patient of Dr. Wingard’s—with a complex retinal history—was on four medications in one eye, which had successfully controlled his pressure. “He jumped at the chance to try Durysta and get off some drops,” said Dr. Wingard, explaining that he’s maintained eye pressure at 12 mm Hg or 13 mm Hg, while being able to stop both Lumigan and Alphagan.
|
What to Expect
“It’s encouraging that the sustained-release formulation does not appear to compromise efficacy,” said Dr. Aref. “The phase 3 trials compared the injection with timolol—not bimatoprost eyedrops—so we can’t say for sure that Durysta is just as effective as the eyedrop formulation, but the trials suggest that they are in a similar ballpark. And this gets us closer to being able to free up patients from topical eyedrops, which is very exciting.”
Dr. Wingard added, “This is profoundly different from available options, which means it will find utility in certain patients who could not be controlled easily with other types of treatment.”
___________________________
1 Craven ER et al. Drugs. 2020;80(2):167-179.
2 Medeiros FA et al., on behalf of the ARTEMIS 1 Study Group. Ophthalmology. Published online June 13, 2020.
___________________________
Dr. Aref is associate professor of ophthalmology, vice chair for clinical affairs, medical director, and director of the glaucoma fellowship training program at the Illinois Eye and Ear Infirmary in Chicago. Relevant financial disclosures: None.
Dr. Sarkisian is founder and CEO of Oklahoma Eye Surgeons in Oklahoma City. Relevant financial disclosures: Allergan: C.
Dr. Wingard is a glaucoma specialist at the Wheaton Eye Clinic in Wheaton, Ill. Relevant financial disclosures: Aerie: C; Allergan: C,L.
For full disclosures and the disclosure key, see below.
Full Financial Disclosures
Dr. Aref Aerie: S; New World Medical: C; Bausch + Lomb: C.
Dr. Sarkisian Aerie: C; Allergan: C.
Dr. Wingard Aerie: C; Allergan: C,L.
Disclosure Category
|
Code
|
Description
|
| Consultant/Advisor |
C |
Consultant fee, paid advisory boards, or fees for attending a meeting. |
| Employee |
E |
Employed by a commercial company. |
| Speakers bureau |
L |
Lecture fees or honoraria, travel fees or reimbursements when speaking at the invitation of a commercial company. |
| Equity owner |
O |
Equity ownership/stock options in publicly or privately traded firms, excluding mutual funds. |
| Patents/Royalty |
P |
Patents and/or royalties for intellectual property. |
| Grant support |
S |
Grant support or other financial support to the investigator from all sources, including research support from government agencies (e.g., NIH), foundations, device manufacturers, and/or pharmaceutical companies. |
|