Download PDF
Injectable soft tissue fillers have become an increasingly popular option for facial rejuvenation in recent years. Their rise in popularity has been driven by a number of factors, including their minimally invasive nature.
The treating physician should keep in mind that the potential exists for complications, especially in the hands of a novice injector. Fortunately, most complications are minor and transient in nature, although the patient may consider them aesthetically displeasing and unacceptable. Major complications are rare, but they can produce permanent, disfiguring damage.
 |
|
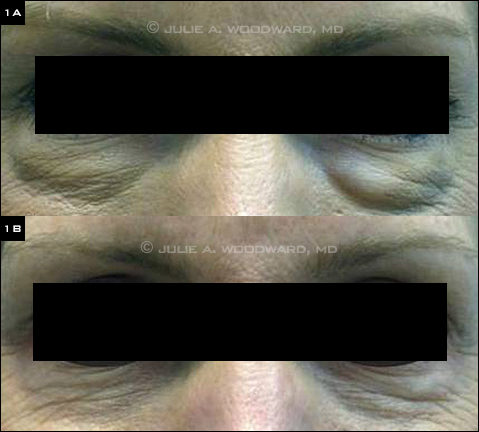
COMPLICATIONS. Patient with visible nodules following soft tissue filler injection, before (1A) and after (1B) injection of hyaluronidase to dissolve the nodules.
|
Preinjection Planning
Complications are best prevented with careful planning. Thorough knowledge of both pertinent facial anatomy and the specific characteristics of each filler is critical. In addition, managing patient expectations is an important element in the pretreatment preparation.
Anatomy. Skin thickness varies among facial areas, which affects optimal injection depth. In addition, areas such as the glabellar region have minimal collateral circulation and are at increased risk of vascular compromise with excessive injection volume.
Choice of filler. The appropriate depth of placement is dependent on the product selected and strongly influences the end result. In order of depth, medium hyaluronic acid products (Restylane, Juvederm, Perlane) should be injected into the deeper dermis, calcium hydroxyapatite (Radiesse) at the dermal-subcutaneous border, and poly-L-lactic acid (Sculptra) in fat below the dermis. An injection placed too superficially can produce nodules and an uneven surface; therefore, it is usually preferable to err on the deeper side.
Patient expectations. Before treatment, the physician should clarify the patient’s goals and expectations for both the procedure itself and the subsequent results, and the patient should be given the opportunity to identify desired treatment areas with a mirror. Standardized pre- and postprocedure photographs should be taken for documentation.
Informed consent. It’s essential to obtain informed consent; this should cover the discussion of potential side effects (the most common sequelae include swelling, bruising, and tenderness) and all details of postoperative care.
Preoperative screening. The patient should be screened for any medical issues that could affect the application of filler,1 such as pharmacologic or pathologic clotting disorders, previous vagal episodes, and any history of seizures.2
 |
|
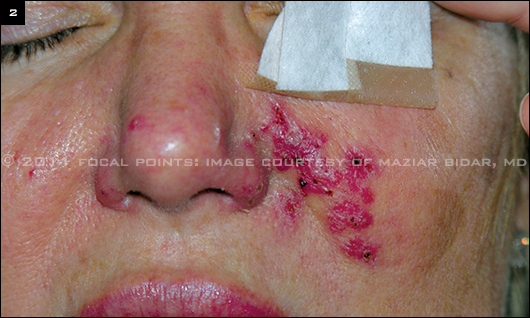
INFECTION. Bacterial infection complicating hyaluronic acid filler injection. Patient presented for second opinion.
|
Complications: Early Onset
Early-onset complications are those that occur within the first two weeks after the injection.
Minor complications. Although most minor early complications can be avoided with proper injection technique and filler selection, even the most seasoned injector can induce bruising and swelling, which a patient may consider socially embarrassing. It is, therefore, crucial to the doctor-patient relationship for the physician to discuss all potential minor complications and their impact on the timing of the injection session. (For instance, some physicians discourage patients from scheduling injections within two weeks preceding important social events.)
Bruising and swelling. This can be limited by avoiding visible vessels while injecting. Pulling the skin taut in a well-lit room can aid this practice, and an assistant should watch for developing ecchymosis. After the session, the patient should apply an ice pack for 15 minutes. It is not necessary for patients to stop blood thinners if they are appropriately counseled prior to the procedure regarding an increased risk of bruising.
If ecchymosis does develop, it can be reduced with vascular lasers or intense pulsed light delivery systems that target the red wavelength. Some physicians suggest the use of Arnica montana 20 percent gel to treat bruising.1
Swelling occurs from both the inflammatory effects of the injection itself and the increased volume of the filler. In addition, particular fillers can increase the risk of swelling. For example, many physicians avoid Juvederm in the periocular area, as its hydrophilicity can lead to significant fluid attraction and periocular edema.
Discomfort. Injection discomfort and tenderness can be a significant source of patient anxiety, especially for the first-time patient. We offer every patient lidocaine-prilocaine 5 percent cream or lidocaine 2 percent dental injection to the infraorbital nerve 15 minutes prior to filler injection. Some physicians place an ice pack directly over the proposed injection site for 30 seconds before injection. In addition, both the physician and an assistant can provide “vocal local” through engaging in conversation with the patient and by offering comforting physical contact, such as hand-holding.
If patients experience minor pain, tenderness, and/or headache after filler injection, they should be counseled to use acetaminophen on the treatment day and to avoid NSAIDs and aspirin for one week, as these can contribute to further bruising. Immediate postinjection discomfort should not be dismissed by the staff or physician, as it could indicate a more serious problem.
Major complications. Worsening of patient appearance after filler injection will be regarded by the patient as a major complication and should be addressed promptly. One of the great advantages of the hyaluronic acid fillers is that they can be dissolved by the injection of hyaluronidase (Figs. 1A, 1B).2 The surgeon should inject 0.2 mL of hyaluronidase and have the patient massage the involved area, then recheck the patient in 30 minutes to make sure he or she is satisfied with the result. Hyaluronidase can be injected multiple times if needed and can be utilized throughout the anticipated duration of the filler.
Nodules. Although patients are normally able to palpate the filler after injection, the physician should be concerned about red, painful, or tender nodules. These signs may indicate the presence of infection and should be cultured if fluctuant (Fig. 2). The patient should be placed on empiric oral antibiotics and rechecked within 48 hours.
Vascular compromise. This is the most feared early complication. Proper injection technique, choice of injection site, and choice of filler can limit the risk of vascular compromise. The glabellar region is at particular risk, given its unpredictable vascular anatomy.2,3 Both arterial embolization and venous obstruction are extremely rare; however, every office should be prepared for such an event.
Symptoms can vary from extreme pain with geographic discoloration to a dull persistant ache.3 Any concern raised by either the patient or the staff should be taken seriously and managed swiftly. The area of concern should be massaged and aspirated.3 Hyaluronidase can be injected if a hyaluronic acid filler was used.2,3 Warm compresses and 2 percent nitroglycerin paste may be applied to assist in vasodilation.2,3 Ice should be avoided. Oral prednisone is also a consideration if edema is thought to be compressing a vessel. The patient should be followed daily until significant improvement is noted and referred for a second opinion if needed.
 |
|
TYNDALL EFFECT. Flour in water demonstrating the Tyndall effect. Particles in a colloid or fine suspension scatter and reflect blue light and transmit red light, causing them to appear blue.
|
Complications: Delayed Onset
Delayed-onset complications are those that occur after the first two weeks postinjection.
Minor complications. The most common complications in this category are residual palpable or visible material, blanching, nodules, and hypersensitivity reactions.
Bumps, blanching, and nodules. If the injected material is placed too superficially or in excess quantity, it can result in visible bumps or blanching/ bluish discoloration of the surrounding area.
The bumps can sometimes appear bluish due to differential light scattering, which is known as the Tyndall effect (Fig. 3).3 The infraorbital area is particularly prone to this complication given the thin skin in that area. In some instances, this discoloration can persist beyond the effective duration of the filler itself.
Even if it is not visually apparent, material can persist as palpable lumps. This is more likely to occur if medium-weight fillers are injected in the papillary epidermis or dermis. Areas at higher risk include the nasojugal folds, nasal dorsum, lips, fine periorbital and perioral lines, and tear troughs. To minimize this occurrence, it is important to inject only in the mid-dermis or deeper and to release pressure on the syringe depressor when withdrawing the needle.
If blanching occurs during the injection, immediate firm massage may resolve the discoloration, although vascular compromise must be ruled out. Options for treating the Tyndall effect and palpable but nonvisible nodules include attempted aspiration, intralesional steroid injection, massage, dermabrasion, puncture and expression, oral allopurinol, injectable hyaluronidase,1 or surgical excision. A Q-switched, 1064-nm laser also has been successfully used to lessen the Tyndall effect.4 Most practioners’ first choice is hyaluronidase injection.
Hypersensitivity reactions. These are rare, and the FDA no longer requires allergy testing for approved fillers. Such a reaction should prompt referral to an allergist or rheumatologist for allergy and autoimmune workup.
Major complications. More significant complications include migration of the filler, granuloma formation, and infection.3
Migration. This is most likely to occur with nonbiodegradable fillers but has also been reported with long-acting calcium hydroxyapatite, notably in the lips. Migration can cause discomfort. Treatment, either by repositioning or excision, can be complicated.
True granulomas. These are rare and occur in less than 0.1 percent of cases.3 Granuloma formation typically occurs within six months but has been reported as late as 15 months postinjection. Granulomas are most likely to occur after injection with products that either do not biodegrade completely or only partially biodegrade. Biofilms, aggregates of cells adhered to living or nonliving materials, have been implicated.
Standard treatment is with either oral or intralesional steroids. The latter require judicious use, as they have been associated with localized atrophy, erythema, and pigment changes, as well as systemic vascular events.3 Adding 5-fluorouracil to the intralesional steroid has also been advocated for granuloma treatment.5 Minocycline has been noted to decrease the size of silicone granulomas.4 If these treatments fail, surgical excision can be attempted as a last resort.
Delayed infection. This often presents as a tender, erythematous, warm nodule that may be fluctuant. The patient may also develop systemic symptoms of malaise. Late presentation raises suspicion for atypical bacteria, especially mycobacteria. Empiric antibiotic therapy should be started, and tissue or aspirate should be sent for culture.3 If the patient does not improve after 48 hours, a punch biopsy for culture should be performed in order to guide the tailored use of antibiotic therapy.3
___________________________
1 Leu S et al. Br J Dermatol. 2010;163(3):557-563.
2 Cohen JL, Brown MR. J Drugs Dermatol. 2009;8(1):13-16.
3 Sclafani AP, Fagien S. Dermatol Surg. 2009;35(suppl 2):1672-1680.
4 Hirsch RJ, Stier M. J Drugs Dermatol. 2008;7(9):841-845.
5 Lemperle G et al. Plast Reconst Surg. 2006;118(3 suppl):92S-107S.
___________________________
Dr. Liao is an orbital and ophthalmic plastic surgery fellow at the Medical College of Wisconsin in Milwaukee; Dr. Ehrlich is an oculoplastic surgeon with Danbury Eye Physicians in Danbury, Conn.; and Dr. Woodward is chief of the oculoplastic and reconstructive surgery service at the Duke Eye Center in Durham, N.C. Drs. Liao and Ehrlich report no related financial interests; Dr. Woodward is a speaker for Inspire, Medicis, and SkinCeuticals.
Got Pearls?
Write a Pearls article!
Ophthalmic Pearls
EyeNet Magazine
655 Beach Street
San Francisco, CA 94109
eyenet@aao.org
|