By Rebecca Hancock, Flora Lum, MD, Chris McDonagh, Cherie McNett, Jessica Peterson, MD, MPH, and Sue Vicchrilli, COT, OCS
This content was excerpted from EyeNet’s MIPS Manual 2017.
The payment adjustment factor will result in bonuses for some clinicians and penalties for others.
CMS compares your 2017 final score against the 3-point performance threshold to determine your 2019 payment adjustment factor. If your final score is:
- 0 points, your payment adjustment factor is –4%;
- 3 points, your payment adjustment factor is neutral (no penalty, no bonus); or
- more than 3 points, you will get a small positive adjustment factor (bonus), based on a linear sliding scale (see the blue line on Table 17A, below).
This process for calculating payment adjustments is designed to be budget neutral, which means that bonuses for those with final scores above 3 points will be funded by the penalties imposed on those who fall below that threshold.
Initially, the maximum negative payment adjustment factor is –4%. During MIPS’ inaugural year—because of the special allowances that were made, such as the 3-point floor for quality measures—the first year’s penalty is effectively all or nothing. If your final score is 0 points, you’ll incur the maximum –4% payment penalty; but with minimal reporting of just 1 quality measure, you score enough points to meet the performance threshold and avoid a penalty.
During the first 4 years, the maximum penalty will steadily increase. The maximum negative payment adjustment factor is scheduled to increase as follows:
- –4% for the 2019 payment year (2017 performance year)
To ensure budget neutrality, the maximum positive payment adjustment factor will be determined after each performance year is over. For the first 4 payment years, the maximum payment adjustment factor will be as follows:
- +4% × scaling factor for the 2019 payment year (2017 performance year)
- +5% × scaling factor for 2020
- +7% × scaling factor for 2021
- +9% × scaling factor for 2022
CMS will use a scaling factor that is greater than 0 but not greater than 3. In 2018, after calculating the 2017 final scores of all MIPS participants, CMS will determine the scaling factor—and thus the maximum payment adjustment factor—for the 2019 payment year.
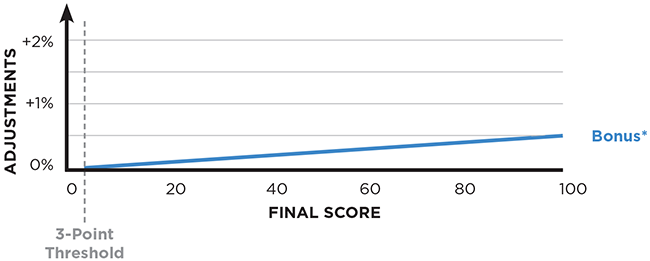
Bonuses will be based on a linear sliding scale. If your final score meets or exceeds the 3-point performance threshold, your payment adjustment factor will be based on a linear sliding scale, starting at 0% for a final score of 3 points and increasing to the maximum payment adjustment factor for a final score of 100 points. Table 17A shows an example of what this sliding scale might look like (see the blue line).
Due to budget neutrality, the sliding scale is expected to be quite flat during year 1. It is easy to avoid the penalty in 2017, and this means that the bonus pool for the 2019 payment adjustments will be relatively small; consequently, the scaling factor will be low, the maximum positive payment adjustment will be low, and the gradient of the sliding scale will be low. (The blue line on Table 17A uses a scaling factor of 0.12 for illustrative purposes; as mentioned above, the actual scaling factor won’t be known until 2018.)
Example. Suppose the scaling factor for the 2019 payment adjustment factor turns out to be 0.12. The maximum payment adjustment factor would be 0.48% (4.0 × 0.12) This would be applied to you if you have a 2017 final score of 100 points and would be the upper limit of the sliding scale.
Clinicians without an EHR system will have a 25-point handicap. If you don’t have an EHR system, you won’t be able to report ACI measures. You will only score points for quality measures (up to 60 points) and improvement activities (up to 15 points), so your maximum score will be 75 points. As CMS increases the performance threshold over the coming years, this 25-point handicap will become increasingly important. However, there are limited circumstances where clinicians without an EHR might have their performance categories reweighted, allowing them to score up to 100 points (see “Some Clinicians May Be Exempt from ACI.”)
Use 2017 to get up to speed, before CMS starts ramping up the financial rewards and risks. Over the next few years, this bonus pool will increase dramatically, funded by a sharp increase in payment penalties. This growth in penalties will be because:
- reporting requirements will become more stringent;
- the performance threshold will be raised (the proposed rule for 2018 raises it to 15 points and by 2019 it is expected to be set so high that half of MIPS participants would fall below the performance threshold); and
- the maximum penalty will rapidly increase (–9% by performance year 2020/payment year 2022).
 |
|
Table 17A. Bonus: Exceed the 3-point payment adjustment threshold, and you can expect a small positive payment adjustment based on a linear sliding scale (blue line).
|
___________________________
Next: Financial Impact: The Additional Payment Adjustment Factor (Tap Into a $500M-Bonus Pool)
Note: Meeting regulatory requirements is a complicated process involving continually changing rules and the application of judgment to factual situations. The Academy does not guarantee or warrant that regulators and public or private payers will agree with the Academy’s information or recommendations. The Academy shall not be liable to you or any other party to any extent whatsoever for errors in, or omissions from, any such information provided by the Academy, its employees, agents, or representatives.
COPYRIGHT© 2017, American Academy of Ophthalmology, Inc.® All rights reserved. No part of this publication may be reproduced without written permission from the publisher. American Academy of Ophthalmic Executives® and IRIS® Registry are trademarks of the American Academy of Ophthalmology®.