A 68-year-old woman presents with worsening distorted central blurry vision
What is your diagnosis?
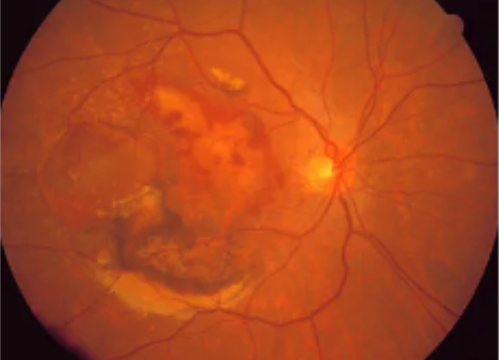
The diagnosis is...
![]()

The image is consistent with a diagnosis of wet age-related macular degeneration (AMD).
- Wet AMD is much less common than the dry form, but it is much more severe and caused by neovascularization (new, abnormal blood vessels) that grows into the macula (central retina).
- These new blood vessels may leak blood and/or fluid, and permanent vision loss occurs when there is scarring in the macula from chronic subretinal hemorrhage.
- Risk factors include advanced age, smoking, hypertension, family history of AMD, genetics, and cardiovascular disease.
- Patients typically present with unilateral blurry central vision and visual distortions that can worsen rapidly. It is commonly noticed when the patient closes the good eye, such as when rubbing the eye or applying makeup.
What is the role of the primary care or emergency medicine physician?
![]()
- Refer the patient to the retina specialist promptly for a dilated eye examination to evaluate for wet AMD.
- Use an Amsler grid, which can aid in diagnosis.
- Note the patient's response. Patients noticing wavy, blurry, or dim lines on the grid may have AMD.

What is the role of the ophthalmologist?
![]()
- Perform a dilated eye examination with a slit-lamp microscope.
- Perform ocular imaging with fluorescein angiography, optical coherence tomography (with or without OCT-angiography), and fundus autofluorescence.


What is the treatment?
![]()
- Anti-vascular endothelial growth factor (Anti-VEGF) intravitreal therapy can help reduce and stabilize neovascularization and associated retinal exudation.
- Surgical interventions include laser photocoagulation or photodynamic therapy to shrink the abnormal neovascular membranes and slow leakage.
- There is currently no cure for wet AMD; therefore, intravitreal injections are a life-long therapy for now.

Learn more: Ophthalmology resources for medical students
![]()