A freak accident on the job nearly cost industrial machinist Jeff Strayer his vision. Thanks to quick action by his coworkers, the almost-magical healing properties of placenta tissue and a skilled ophthalmologist, the 53-year-old is back on the job and seeing 20/20.
While working the night shift at a manufacturing facility in Cleveland, Ohio, Jeff picked up a milk jug-sized container of sodium hydroxide, the same chemical in Drano or lye. As he lifted it off the floor, the lid unexpectedly popped off, dousing his face and arms with the caustic chemical.
"Time really is of the essence if something like this happens." - Jeff Strayer, chemical burn survivor
"When it splashed up on me, it burned; my arms burned, my eyes burned, I couldn't see, and I was just cussing," Strayer said. "I can look back now and see that the reaction of my coworkers made such a difference, even though they weren't sure what happened. One of them quickly guided me over to a work site eyewash station to irrigate my eyes and someone called 9-1-1."
Strayer's coworkers did exactly the right thing. Initial treatment of any chemical burn should begin immediately. The eye should be flushed with water immediately, and throughout transportation to the hospital. The goal is to dilute the chemical burning through the eye's delicate tissue.
First Response Makes all the Difference

Thomas Steinemann, MD, stands outside the ophthalmology clinic in Cleveland, Ohio, where he treated Jeff Strayer for an agonizing chemical burn to his eyes.
Chemical injuries are one of the most difficult eye emergencies ophthalmologists face. What's standing between a patient and blindness is not only the severity of injury, but also how quickly they are treated and what kind of treatment they receive.
After initial treatment at a local hospital, Strayer was transferred about 12 hours later to the Level 1 Adult Trauma Center at MetroHealth in Cleveland, where ophthalmologist Thomas Steinemann, MD, took over Strayer's care.
"The damage through burning is incurred within seconds to minutes, and you could definitely lose not only your eyesight, but your entire eye." - Dr. Steinemann
Dr. Steinemann sees patients who have suffered chemical burns to their cornea – the clear, dome-shaped window of the front of the eye – about once a month. Typically, the burn is a result of an accident at work. Alkali chemicals, such as lye, ammonia and calcium hydroxide, are responsible for the most damaging injuries. The reason why is that the cornea's ability to renew and repair itself depends on special cells that lie in a narrow zone between the cornea and the white part of the eye. Once these cells, called limbal stem cells, are damaged, the body can't make more.
"The reason lye works so well for its intended use is that it's a detergent and goes right through things that are oily, greasy or fatty," said Dr. Steinemann. "It destroys cells. You don't get spare stem cells. Those have to last you a lifetime. Jeff's injury could very well have resulted in blindness."
Nearly the entire surface of his right cornea burned, damaging about two-thirds of the area where the stem cells live. His left eye suffered a mild burn, but his arms were burned so badly he needed skin grafts. Making matters worse, Strayer had refractive surgery years earlier, putting him at higher risk of possible infection and other complications.
Dr. Steinemann knew what he had to do to try and save Strayer's eye. He would need a new, old treatment. He would use a patch of amniotic membrane to heal Strayer's damaged eye.
A "Biologic Bandage"
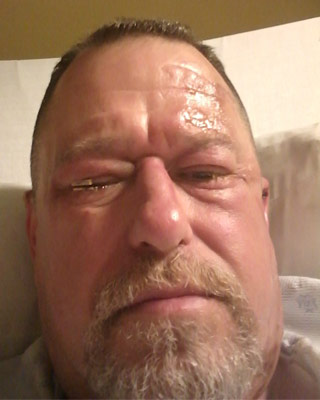
Jeff Strayer recovers in the hospital with placenta tissue applied to his right eye, which is sewn shut, as a treatment for a chemical burn injury.
Amniotic membrane is the innermost layer of placenta. The tissue is donated from live caesarean births. In the 1940s, physicians started experimenting with a chemically processed amniotic membrane to treat severe burns and reported remarkable success. But, for reasons not well documented in the literature, its popularity waned and it was not routinely practiced. Until about 20 years ago, when a researcher ophthalmologist named Scheffer C. G. Tseng, MD, PhD, began experimenting with the idea of using amniotic membrane to heal tissue damage.
It works because fetal wound healing is different from adult wound healing. Adult healing is slower, incomplete, and often results in scarring. The fetal environment is unique in human nature. The placenta tissue is made up of components that reduce inflammation and scarring, lower bacteria levels and promote faster tissue healing.
Previously, physicians would use only steroids and antibiotics to treat patients like Strayer, and hope for the best. Now, ophthalmologists have a chance to help their patients recover their vision.
In addition to a slow, tapered dose of steroid eye drops, Dr. Steinemann used a patch of amniotic membrane.
"It's like a little contact lens that fits onto the eye, but it's more like a ring, with a little doughnut hole in the middle," explained Dr. Steinemann, noting that he had to sew Strayer's eye shut to keep the ring in place and maintain the integrity of the treatment. "Inside the hole is the amniotic membrane, which is very thin and translucent – like tissue paper."
Dr. Steinemann said the membrane slowly dissolves over approximately two weeks, during which it releases "all these good things into your eye."
"It's a remarkable treatment," said Dr. Steinemann. "Dr. Tseng is brilliant. He'd read several historic studies from prior decades about using amniotic membrane for various treatments, then took it a step further to make it work for the first widespread commercial applications. I'm very grateful to Dr. Tseng. This treatment is an absolute godsend for patients. Before this, there wasn't really a way to truly heal eyes from these types of injuries."
The bad news for the patient? "Yes, it is very uncomfortable," Strayer said. "It's this piece of plastic, and you have that feeling of something in your eye."
The good news for the patient? "It worked," Strayer said.
Surprising Recovery
After 14 days in the hospital, lying in a bed with one eye sewn shut and recovering from burns to his arms, doctor and patient prepared for the big reveal.
Based on his experience and the devastating injury, Dr. Steinemann expected Strayer would likely need a second round of treatment, so the reveal began with Strayer under general anesthetic. Dr. Steinemann got a pleasant surprise when he removed the plastic device holding the membrane.
"Lo and behold, the surface of his eye was healed," Dr. Steinemann said. "I was surprised at how quickly it had healed. And relieved. When Jeff came out of anesthesia, we had some great news to share."
"I Got My Vision Back"
Strayer hopes his story will prevent others from experiencing the pain and fear he went through. But if they do, he wants people to know how to respond.
"Time really is of the essence if something like this happens," he said. "You think you might really go blind, you think you might lose your independence. But I was so fortunate; I got my vision back. That's all I care about."
"In terms of ophthalmic injuries, this is the worst chemical burn injury possible to the eye," Dr. Steinemann said. "The damage through burning is incurred within seconds to minutes, and you could definitely lose not only your eyesight, but your entire eye. The speed with which we were able to see him and the treatment options available, I think definitely saved his vision.”
The patient gives a bit more credit to his doctor. "Dr. Steinemann gets a lot of responsibility for my successful recovery. He's a great man; just a dynamite gentleman."