By Carrie L. Morris, MD, and David A. Chesnutt, MD
Edited by Sharon Fekrat, MD, and Ingrid U. Scott, MD, MPH
This article is from February 2005 and may contain outdated material.
Acquired ptosis results when the structures of the upper eyelid are inadequate to maintain normal lid elevation. Conditions that cause ptosis range in severity from life-threatening neurological emergencies to involutional processes that develop over years.
A logical approach to ptosis requires an understanding of upper eyelid anatomy. It is generally accepted that upper eyelid ptosis is defined by the positioning of the upper eyelid at least 1.5 to 2 millimeters inferior to the upper limbus (see “Anatomic Considerations” ).
 |
|
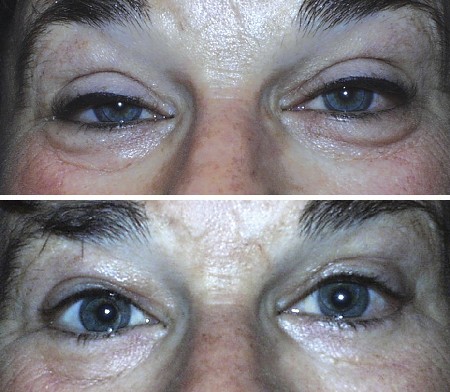
Acquired ptosis before (top) and after (bottom) surgery.
|
Initial Evaluation
Determining the cause of acquired ptosis is critical to the choice of therapy. One must first be certain that the ptosis is not a manifestation of serious underlying neurological disease. A careful evaluation of pupil size, ocular motility and facial sensation should be performed, in addition to assessment of lid height, palpebral fissure height and levator function. Moreover, true ptosis has to be differentiated from pseudoptosis, which may be caused by conditions such as blepharospasm or hemifacial spasm.
Types of Acquired Ptosis
Ptosis may be classified by considering age at onset, etiology, severity and the remaining amount of levator palpebrae superioris function:
Aponeurotic ptosis. Senescent slippage of the aponeurosis is the most common cause of mild to moderate ptosis in the elderly. The effects of gravity and loss of tone due to aging stretch the levator muscle and its aponeurosis. Disinsertion or dehiscence of the aponeurosis may be worsened by chronic inflammation, intraocular surgery, trauma or hard contact lens wear. Levator aponeurosis advancements are generally the most appropriate procedures for these cases, since they correct the underlying etiology.1
Myogenic ptosis. Dysfunction of the levator muscle prohibits the eyelid from being elevated into proper position. The most common diseases responsible for this are myasthenia gravis, myotonic dystrophy, facio-scalpulo-humeral muscular dystrophy, oculopharyngeal muscular dystrophy, congenital myopathies, chronic progressive external ophthalmoplegia and mitochondriopathy.
Unfortunately, these are generally progressive and frequently recur even after initial surgical treatment. In these cases, a sling procedure or ptosis crutches may be beneficial. The amount of eyelid elevation should be conservative to avoid ocular exposure and also may need to be supplemented with a lower eyelid-elevating procedure.1–3
Myasthenia gravis causes variable ptosis, often with ocular misalignment and other cranial or limb muscle weakness. Although the primary treatment of myasthenia is usually pharmacologic, surgery may be indicated in stable, refractory cases.
Neurogenic ptosis. Dysfunction or damage to the oculomotor or sympathetic nerve(s) or to the central nervous system may result in ptosis. The third nerve passes from the midbrain through the interpeduncular cistern to the cavernous sinus before reaching the orbital apex. Intracranial aneurysm (usually arising from the posterior communicating artery) and resulting subarachnoid hemorrhage, in addition to meningitis and other compressive and infiltrative lesions in the area, may lead to ptosis by damaging the third nerve. Because the levator is the primary muscle responsible for keeping the lid open, severe deficits of third nerve function usually cause profound or complete ptosis. Depending on the cause, a period of observation should occur prior to surgical intervention to allow for any recovery of nerve and levator muscle function. A frontalis suspension using a silicone rod or fascia lata for the sling achieves the best results in these cases.1,4
Müller’s muscle provides only a small contribution to lid height. Thus, only mild ptosis is seen in Horner’s syndrome, in which there is interruption of the sympathetic fibers that innervate Müller’s muscle. Horner’s syndrome may be caused by a variety of lesions, including carotid dissection, cavernous sinus tumors or pulmonary apex lesions that disrupt the sympathetic chain.
Indirect causes of neurogenic ptosis include diabetes, tumors, carotid-cavernous aneurysms and multiple sclerosis. Owing to the small contribution to ptosis from Müller’s muscle dysfunction, procedures directed to Müller’s muscle will correct only a small amount of ptosis. These would include the Fasanella-Servat procedure and similar measures.
Mechanical ptosis. This occurs when the eyelid is too heavy for the muscles to elevate it, such as occurs in blepharochalasis, orbital fat prolapse and eyelid tumors. The ongoing increased weight on the eyelid will cause stretching of the thin eyelid skin. Removal of the ptosis-inducing mass (if present) and excess eyelid skin, with or without a possible adjunctive levator resection, alleviates the problem.1,4
Traumatic ptosis. In some instances, the levator may be disinserted. In more extensive trauma, the levator tendon may have been transected with scar formation and secondary mechanical ptosis. There also may be third nerve damage. An individualized assessment is needed to establish the proper surgical approach. Traumatic ptosis may also worsen later in life as further levator aponeurosis slippage occurs.1,4
Treatment
Ptosis severity is commonly divided as follows: mild (1-2 mm), moderate (3-4 mm) or severe (> 4 mm). In addition, levator function is commonly categorized as good (> 8 mm), fair (5-7 mm) or poor (0-4 mm).
In determining the optimal surgical approach, one must consider the remaining levator function with the amount of ptosis to be corrected, along with the etiology of the ptosis.
Levator aponeurosis advancement, which tightens or reattaches the aponeurosis back to the tarsal plate, should address the needs of patients with good levator function. The Fasanella-Servat Müllerectomy is an alternative option for those with good levator function.2,4
Those with poor levator function will likely achieve the most benefit from frontalis sling procedure, which suspends the upper eyelid from the frontalis muscle of the forehead. This procedure, which is effective in cases such as myogenic ptosis, allows a degree of voluntary lid control. A levator resection is another option in patients with moderate to poor levator function. Partial resection of the levator palpebrae superioris achieves improved upper eyelid height by strengthening the muscle.
_____________________________
1 Finsterer, J. Aesth Plast Surg 2003;27: 193–204.
2 Dutton, J. J. et al. Atlas of Ophthalmic Surgery, Vol. 2, Oculoplastic, Lacrimal and Orbital Surgery (St. Louis: Mosby Year Book, 1992).
3 Wong, V. A. et al. Ophthalmology 2002;109: 1023–1031.
4 McCord, C. D. et al. Oculoplastic Surgery (New York: Lippincott, Williams and Wilkins, 1995).
_____________________________
Anatomic Considerations
The upper eyelid takes its form from the tarsal plate, a cartilaginous structure, which is covered by skin on its external surface and by the palpebral conjunctiva on its internal surface. The tarsal plate extends upward approximately 10 mm from the upper eyelid margin. The eyelashes insert into the inferior border of the tarsal plate to extend out through the gray line, which is the anatomical division between the anterior and posterior lamellae of the eyelid. The anterior lamella is composed of eyelid skin and orbicularis oculi muscle, while the posterior lamella is made up of the tarsus and the palpebral conjunctiva.
The orbital septum separates the preseptal soft tissue space from deeper orbital structures. The orbital septal barrier is important because it protects vital orbital structures from invasion by potentially harmful processes such as infection or hemorrhage from surgical incisions or traumatic wounds. In other circumstances, the orbital septum can be counterproductive when it confines deep hemorrhage, sometimes leading to damaging compression of the optic nerve.
Forty millimeters in length, the levator palpebrae superioris originates slightly above the annulus of Zinn adjacent to the lesser wing of the sphenoid. At the equator of the globe, a transition from muscle to aponeurosis occurs 15 to 17 mm proximal to the superior tarsal border. It is at this transition zone that the superior transverse ligament of Whitnall is formed. Of note, at this location the direction of pull of the levator muscle and the aponeurosis is converted from a proximal posterior vector to a superior vector distally. The upper eyelid crease is formed by the levator aponeurosis and the orbital septum attaching to the deep surface of the orbicularis oculi, the upper border of the tarsus, subcutaneous tissues and skin. The upper eyelid crease is located approximately 7 to 12 mm from the lashes.
_____________________________
Dr. Morris is a first-year resident in ophthalmology and Dr. Chesnutt is assistant clinical professor of ophthalmology; both are at Duke University Eye Center.