Blink
Can You Guess June's Mystery Condition?
Download PDF
Make your diagnosis in the comments, and look for the answer in next month’s Blink.
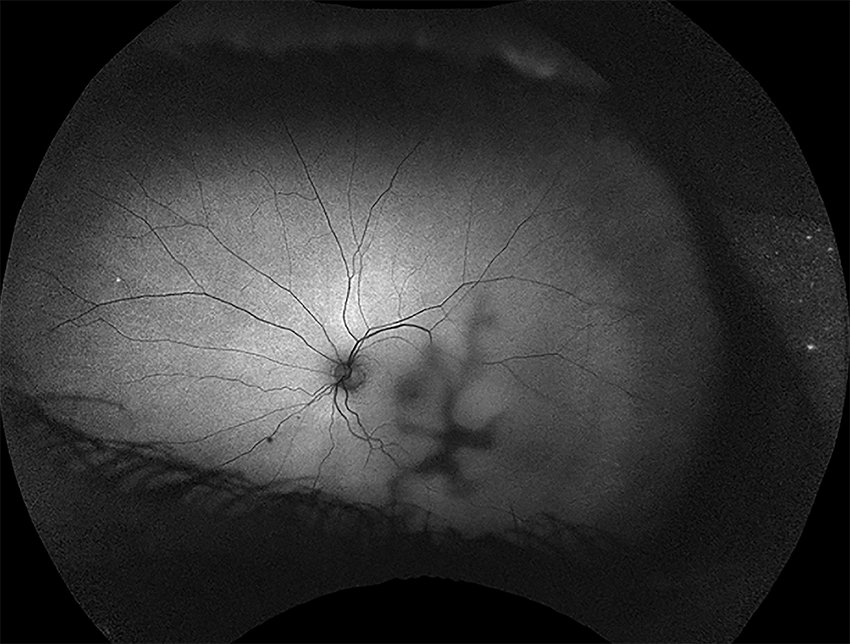
Last Month’s Blink
Chronic Exposure of IOL Optic
Written by Shuk Kei Cheng, MD, Roman Shinder, MD, and Jennifer Park, MD, at Kings County Hospital and SUNY Downstate Medical Center, Brooklyn, N.Y. Photo by Jennifer Park, MD.
A 79-year-old man presented for his regularly scheduled eye examination in late summer of 2020. It had been a while since we had seen him, and the optic of his posterior chamber IOL was exposed through an area of prior corneal perforation in his right eye (photo).
He had been our patient since 2006. His past medical history included cataract surgery in the right eye in 2013 and in the left in 2014. In 2015, ischemic central retinal vein occlusion had developed in the right eye (at this time, vision in this eye was hand motion only), which led to neovascular glaucoma. His glaucoma was poorly controlled, resulting in complete loss of vision in that eye. In 2019, the patient developed bullous keratopathy in the right eye, with subsequent Serratia marcescens keratitis, which was initially treated with fortified vancomycin and tobramycin and then—after the culture was shown to be sensitive to tobramycin—with fortified tobramycin alone. He experienced corneal perforation requiring cyanoacrylate glue application. He was then lost to follow-up.
When he returned to our clinic six months later in August of 2020, the area of prior corneal perforation was Seidel negative, and the exposed IOL was fixed in place and could not be dislodged at the slit lamp due to dense perioptic fibrosis. The patient’s vision is now no light perception in the right eye and 20/60 in the left.
Read your colleagues’ discussion.
| BLINK SUBMISSIONS: Send us your ophthalmic image and its explanation in 150-250 words. E-mail to eyenet@aao.org, fax to 415-561-8575, or mail to EyeNet Magazine, 655 Beach Street, San Francisco, CA 94109. Please note that EyeNet reserves the right to edit Blink submissions. |