Download PDF
In the words of Hippocrates, “He who would become a surgeon should find an army and follow it.” This statement indicates the millennia-old connections between the military and medicine. Throughout the centuries, many innovations formed in the crucible of combat have found their place in civilian medical care, particularly in emergency settings. Ambulances, wound debridement and disinfection, blood transfusion techniques, and medical evacuation air transport are just a few of many historical contributions from military medicine.
Yet given the differences between the military and civilian arenas, not all techniques and approaches that work effectively in a frontline hospital are necessarily transferable to a community emergency room. What are some of the promising areas of shared knowledge and experience?
In Part 1 of “From the Frontlines to the Home Front,” EyeNet focused on treatment of gunshot wounds in combat and in the community. We continue the conversation, with Vikram D. Durairaj, MD, a professor of ophthalmology and otolaryngology and the chief of oculoplastics and orbital surgery at the University of Colorado Hospital (UCH) in Aurora; Col. (Ret.) Robert A. Mazzoli, MD, former Consultant to the Surgeon General of the U.S. Army and former chief of ophthalmology at Madigan Army Medical Center in Tacoma, Wash.; and Lynn Polonski, MD, a clinical assistant professor of ophthalmology at the University of Arizona in Tucson. This month, these three oculoplastic surgeons provide their perspectives on how best to apply the lessons from the battlefield to the civilian ER.
|
Trauma Teams at Work
|
 |
|
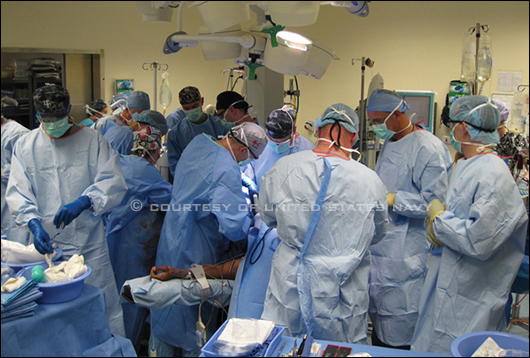
Role 3 NATO hospital in Kandahar, Afghanistan. On a scale of 1 to 4, Role 3 indicates the availability of multiple specialty medical services.
|
Combat Experience in the ER
According to Dr. Polonski, physicians with military service under their belt may be more comfortable than others in providing emergency trauma care; and, just as important, the experience of military physicians has enriched the management of ocular trauma that their civilian colleagues may face. He said, “Military ophthalmologists have absolutely, without doubt, helped the civilian sector,” and listed several examples of lessons learned (some of which were discussed at greater length in Part 1):
- Treating a trauma patient as early as possible is an advantage that was established—beyond question—in Iraq and Afghanistan.
- Addressing the condition of the globe is paramount: If it’s ruptured, then repair it as early as possible.
- Lateral canthotomies are crucial in relieving high intraocular pressure (IOP) induced by trauma. Make sure that everyone in your ER knows how to perform this procedure and that they monitor IOP—these steps can spare the optic nerve from unnecessary damage.
- Lid lacerations should be repaired within 24 hours, especially full-thickness lacerations. Most of the time all lid tissue is there, even in significant trauma, and is still vital, as long as you have a vascular supply.
- Remember that decisions made emergently on the orbit, the rim, and the lids can either optimize or seriously limit recovery of the eye’s function and the eventual outcomes for cosmesis. It can be like a puzzle, but often all the original tissue is still there.
Speed Is of the Essence
Dr. Mazzoli said that getting an injured patient to timely care is the great trick of rural and military medicine. “Air transport has been the key for getting seriously wounded troops from Iraq and Afghanistan to initial care in the theater [of combat operations] and then to Walter Reed–Bethesda or, for burns and polytrauma patients, to Brooke Army Medical Center in San Antonio. Contrary to the days when stabilizing the patient was the first priority, military transports will even take patients who are critically ill and under intubation.”
A fundamental concept of en route care is that it should be “seamless”; that is, there should be no reduction in the level of care throughout the process of transport and transfers.1
Oxygenation under stress. Dr. Mazzoli said that even if troops are being ventilated, they may be battling insufficient oxygen. “So we use the same technological support provided to premature infants with hypoxemia: extracorporeal membrane oxygenation (ECMO), which is basically a temporary cardiovascular bypass.” This technique is now being tried in civilian settings. Recently, physicians from a San Diego hospital reported success in using ECMO in the emergency department.2
Don’t leave the patient in agony. The principle of timely care extends to pain relief, as well. Delays can become a “trial of spirit” for patients and families, Dr. Mazzoli said, and pain becomes the devil in those moments. He advocates for the most efficient relief possible within medical mandates, depending on the type of trauma. “Neuro wounds should not get opioids, which would interfere with the hospital staff’s ability to monitor consciousness. So some severe polytrauma injuries, especially those involving the brain or eye, may call for the use of fentanyl.” He also said that IV acetaminophen appears to provide “pretty profound but safe pain relief.”
Early Assessment and Repair
The type of trauma matters. Regardless of the setting, the approach to treatment depends on the type of injury. According to Dr. Mazzoli, “The approach to repair of blunt trauma, for example, is different from, say, penetrating, blast, or burn trauma because the mechanism is so different. Bomb blast injuries result in a lot of tissue destruction, obviously, whereas crush trauma releases a bunch of mediators. Typically, we see a combination of mechanisms—laceration, barotrauma, perforating trauma, crush, burn, et cetera. They don’t respect a surgical plane—they are multitissue and multilayer—all grossly contaminated and horribly gruesome.”
To manage such wounds, he said, “We use inert sutures so as not to add to the inflammatory process, and we do not close deep spaces tightly, so as to avoid sequestered sutures and extraneous material that perhaps add to the subcutaneous debris burden. We use a lot of drains and vertical mattress sutures. A side benefit of this approach is that some of the foreign bodies actually migrate out.”
Get the priorities right—from the start. Dr. Polonski emphasized the importance of meticulous primary repairs. “The priorities confirmed by military surgeons prove that you can either save a patient’s vision when [the priorities] are followed or, when ignored, allow it to be lost,” he said. “I recently treated a boy who was ejected out of the back of a car. His medial canthus was avulsed, but the surgeon at hand didn’t address the repair of the levator muscle or keep the tarsal plate intact. If you don’t do it right the first time, it’s almost impossible to re-engineer. Consequently, I really think it’s crucial to have oculoplastic expertise on a university faculty and an ER staff.”
Different Types of Teamwork
Rubbing elbows with neurosurgeons, orthopedic surgeons, and thoracic surgeons is a given in a mass trauma situation, Dr. Polonski said. “We work great as a team at the University of Arizona, and that’s the only way a complicated case is going to have a successful outcome.” Dr. Mazzoli agrees that teamwork is crucial, but he has observed that the division of labor among the teams is somewhat different in the military and civilian settings.
Military teamwork. In combat, said Dr. Mazzoli, “We know we’re getting the patient out of the theater very quickly and into the hands of others on a very capable team. It’s very much damage-control surgery, which allows us some luxury of not having to worry so much about making things as pretty as we’d like on the table. We know we’re just a part of the team and that there are very good teammates behind us who will take what we give them and work magic.”
In fact, he continued, ophthalmologists in combat situations may limit their interventions even with procedures they are fully capable of performing. “For example, we’ve had retina docs deploy who would be fully capable of removing intraocular foreign bodies, but they don’t; similarly, we have oculoplastics folks who could do the fracture or complex lid repairs in the combat theater, or cornea docs who could do corneal patch grafts in the theater—but they don’t, opting to defer those interventions for the folks stateside, where conditions are more controlled. We don’t want to burn any bridges in haste.”
Of course, he added, “We try to give patients as good an initial repair as we can so our colleagues can have a good foundation to work from. But we know we don’t have to win the battle ourselves.”
Community ER teamwork. In contrast, in a civilian emergency setting, the ophthalmologist typically does not face quite the same time pressures: for example, the urgency of the patient needing to be put on a medevac plane that just landed or having to get out of the OR because of the next expected wave of casualties, Dr. Mazzoli said. “In that regard, civilian trauma may have the ‘luxury’ of taking a bit more time to do the initial repairs all at once, primarily. But that is tempered by the reality that there is not a whole team behind you waiting to take over, and the first repair is very likely the final repair that has to be done right the first time.” In part, insurance or other financial constraints may limit the involvement of additional specialists.
Ophthalmologists and ER Call
The need for ophthalmic trauma expertise in ERs everywhere is complicated by a relative shortage of ophthalmologists willing to provide it. Many ophthalmologists do not feel qualified or motivated to commit to ER call. “I understand there are ophthalmologists who aren’t comfortable handling ER cases if they haven’t kept up with trauma medicine. But it’s good, I think, to be part of a teaching program that includes such training,” Dr. Polonski said.
Both Drs. Durairaj and Polonski serve ER call in their local hospitals, and they suggest that all ophthalmologists should be willing to do the same. Given the moments of panic and tragedy the nation witnessed in the Newtown, Aurora, and Tucson shootings, for example, “Not to do emergency call is a disservice to the community,” Dr. Durairaj said.
Working to meet community—and educational—needs. In Denver, UCH and affiliated hospitals, including Denver Health and Children’s Hospital Colorado, provide level 1 trauma services for a large geographic area, and severely injured individuals are helicoptered in from hundreds of miles away, said Dr. Durairaj. The orbital trauma experts at these institutions have authored some of the largest series of reports published on oculofacial trauma, especially pediatric trauma. “Consequently,” said Dr. Durairaj, “we are a highly competitive choice for ophthalmology residents with an interest in trauma seeking ASOPRS fellowship training in oculoplastics.”
More coordination required. It is surprising, he said, that there is not yet a single, comprehensive national or even regional collaboration system in place to notify hospitals of an emerging disaster like a mass shooting. “I wish there was a better, more clear-cut alert system for the kind of rapidly escalating events that require the skills of subspecialists. Timing and collaboration in these situations can mean everything,” said Dr. Durairaj, referring to one Aurora patient he believes was saved by a neurosurgery team controlling an intracranial hemorrhage just in time.
|
Convergence of Expertise
Initiatives from both the military and civilian sides of trauma are demonstrating ways in which trauma experts can share the best of both worlds.
For example, in the United Kingdom, the National Institute of Health Research Center for Surgical Reconstruction and Microbiology was inaugurated in Birmingham in 2011, with the specific aim of bringing advanced battlefield techniques used by NATO troops in Afghanistan to improve trauma care for all.
According to Professor Dame Sally Davies, director-general of research and development at the U.K. Department of Health, “Every new unit is exciting, but this one is unique in the country and worldwide. We’re putting together military expertise with NHS [National Health Service] expertise backed up by a first-class university through research to make a difference to patients, making them better, learning lessons and sharing them.”3
In the United States, the National Trauma Institute (NTI), based in San Antonio, is working toward funding large-scale research grants to advance clinical trauma practice and to raise public awareness. This organization was founded as a demonstration project and feasibility study for a joint military/civilian trauma and burn program and included Brooke Army Medical Center and Wilford Hall Medical Center—San Antonio’s two Department of Defense level 1 trauma centers—the U.S. Army Institute of Surgical Research, and the University of Texas Health Science Center/University Hospital Trauma Center.
Although the NTI has since become an independent nonprofit, it continues to bring together military and civilian trauma physicians, both in its governance and its annual educational symposia. (For more information, see www.nationaltraumainstitute.org.)
One thing is certain: “The contribution military medicine has made to wound care is not a finished chapter in the book of medical history; for as long as there will be conflict there will always be a necessity for military medicine to devise better ways to treat the wounded.”4
___________________________
1 Bridges E, Biever K. AACN Adv Crit Care. 2010;21(3):260-276.
2 Shinar Z et al. J Emerg Med. 2012;43(1):83-86.
3 www.gov.uk/government/news/new-nhs-and-military-trauma-centre-opens.
4 Broughton G II, Burriss D. War and medicine: a brief history of the military’s contribution to wound care through World War I. In: Sen CK, ed. Advances in Wound Care. Vol 1. New Rochelle, N.Y.: Mary Ann Liebert; 2010.
___________________________
Drs. Durairaj, Mazzoli, and Polonski report no related financial interests.
___________________________
NOTE: The views expressed in this article are those of the author(s) and do not necessarily reflect the official policy or position of the U.S. Departments of the Navy, Army, or Air Force; the U.S. Department of Defense; or the U.S. government.