Download PDF
Using “deep learning” techniques, researchers in the Google Brain initiative have developed a self-optimizing algorithm that can examine large numbers of fundus photographs and automatically detect diabetic retinopathy (DR) and diabetic macular edema (DME) with a high degree of accuracy.
When the researchers tested the screening algorithm’s performance on 2 groups of images (N = 11,711), it had a sensitivity of 96.1% and 97.5% and a specificity of 93.9% for DR and DME, respectively.1
“It’s a real accomplishment that Google was able to get high sensitivity and specificity at the same time—meaning that not only is this algorithm missing very few people who have disease, but it is also unlikely to overdiagnose disease,” said Peter A. Karth, MD, MBA, a vitreoretinal subspecialist in Eugene, Ore., and at Stanford University, who is a consultant to the Google Brain project.
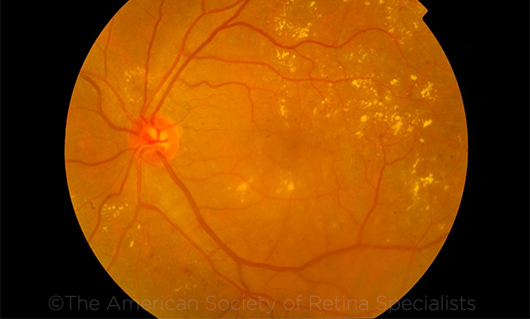 |
DIABETIC RETINOPATHY. Computers are learning to recognize diabetic eye disease in fundus photos, with the help of a self-optimizing algorithm. (This image was originally published in the ASRS Retina Image Bank. Manjiri Patwari. Diabetic Retinopathy. Retina Image Bank. 2015; Image Number 24934. © The American Society of Retina Specialists.)
|
How the system learns. The mathematical algorithm is based on deep machine learning, a type of artificial intelligence (AI) technology in which a neural network “learns” to perform a task through repetition and self-correction.
In this case, the authors reported, the computerized algorithm was trained with 128,175 human-graded fundus images that showed varying levels of diabetic retinal disease. “Then, for each image, the severity grade given by the [algorithm] is compared with the known grade from the training set, and parameters … are then modified slightly to decrease the error on that image,” they wrote. “This process is repeated for every image in the training set many times over, and the [algorithm] ‘learns’ how to accurately compute the diabetic retinopathy severity from the pixel intensities of the image for all images in the training set.”1
Dr. Karth noted that the algorithm works even though it was not designed to look specifically for the lesion-based features that a human would seek on fundus images. “What’s so exciting with deep learning is that we’re not actually yet sure what the system is looking at. All we know is that it’s arriving at a correct diagnosis as often as ophthalmologists are,” he said.
Ehsan Rahimy, MD, a Google Brain consultant and vitreoretinal subspecialist in practice at the Palo Alto Medical Foundation, in Palo Alto, Calif., agreed. “We don’t entirely understand the path that the system is taking. It may very well be seeing the same things we’re seeing, like microaneurysms, hemorrhages, or neovascularization,” he said. “But it’s also very likely that the algorithm is looking beyond those features, at things that are not readily apparent to us as human beings when we look at an image.”
AI won’t replace doctors’ intelligence. Much more work is necessary before the algorithm would be ready for clinical use, but the eventual goal is to increase access to and reduce the cost of screening and treatment for diabetic eye disease, especially in under-resourced environments, Dr. Karth and Dr. Rahimy said.
“Anytime you talk about machine learning in medicine, the knee-jerk reaction is to worry that doctors are being replaced. But this is not going to replace doctors. In fact it’s going to increase the flow of patients with real disease who need real treatments,” Dr. Rahimy said.
“This is an important first step toward dramatically lowering the cost of screening for diabetic retinopathy and, therefore, dramatically increasing the number of people who are screened,” Dr. Karth said. “We feel that with this kind of technology, once it is fully deployed, there will be more people screened for this disease and decreased rates of uncontrolled diabetic vision loss and diabetic retinopathy.”
—Linda Roach
___________________________
1 Gulshan V et al. JAMA. 2016;316(22):2402-2410.
___________________________
Relevant financial disclosures—Dr. Karth: Google Brain: C; Carl Zeiss Meditec: C. Dr. Rahimy: Google Brain: C.
For full disclosures and disclosure key, see below.
More from this month’s News in Review