Download PDF
This month, News in Review Highlights selected papers from the original papers sessions at AAO 2017. Each was chosen by the session chair because it presents important news or illustrates a trend in the field. Only 4 subspecialties are included here; papers sessions will also be held in 6 other fields. See the Meeting Program, which you’ll find in your meeting bag, or the Mobile Meeting Guide for more information.
The IRIS Registry, the nation’s only comprehensive database of ophthalmic outcomes, currently includes real-world data from 41.2 million patients. For the following separate studies, researchers mined the data to shed light on treatment patterns.
Study 1: DME treatment patterns. Researchers identified a large cohort of 13,410 newly diagnosed patients with diabetic macular edema (DME) and their initial treatment. They found that only 5,316 patients (39.6%) received any type of treatment during the first year after diagnosis. Among those who were treated during the first year, 59.3% received anti–vascular endothelial growth factor (VEGF) drugs, 34.6% were treated with laser, and 4.5% received steroids as the initial treatment.
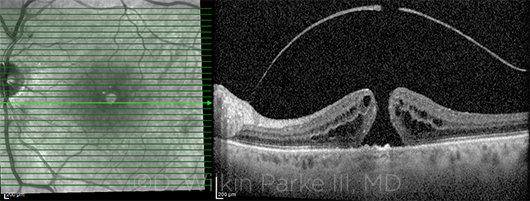 |
BACK TO THE OR? OCT of a full-thickness macular hole.
|
Dangers of inaction. “Although some patients’ DME may not be urgently vision threatening—prompting physicians to observe, rather than to treat during the first year—a large proportion of patients may not be receiving the treatment they need and are at risk for vision loss,” said coauthor Jeffrey R. Willis, MD, who practices in Sacramento, California. This may be occurring for a range of reasons, he said, from transportation and insurance issues to poor awareness about the importance of timely treatment.
Building on these findings, said Dr. Willis, future studies should investigate barriers that limit patients’ access to DME treatment. In addition, developing longer-acting drugs could be an avenue for addressing logistical challenges around current DME care.
A powerful research tool. “The IRIS Registry can be a powerful tool to help clinical researchers and health policy makers understand unmet needs in ophthalmic care,” Dr. Willis commented. “We are in the very beginning stages of understanding the utility of large datasets in ophthalmology. As more people utilize the registry, the more capable we will become in applying it to promote better health outcomes.”
Study 2: Return to the OR after macular surgery. Capitalizing on its data from a wide range of practices, D. Wilkin Parke III, MD, turned to the IRIS Registry to retrospectively assess the rate of return to the operating room within a year of macular surgery.
Rate of return. Among 11,472 eyes that had undergone vitrectomy to treat macular hole, 2,095 had a second surgery, with 851 (7.4%) returning for surgery unrelated to cataract. Among 20,291 eyes that had undergone vitrectomy for epiretinal membrane, 3,354 had a second surgery and 1,252 (6.2%) were unrelated to cataract. Most noncataract second surgeries after macular hole surgery involved a second macular hole repair. Membrane stripping was the procedure conducted most often in second surgeries after an initial epiretinal membrane surgery.
Treatment Patterns for DME in the United States: Analysis of the IRIS Registry. When: Sunday, Nov. 12, 11:39-11:46 a.m., during the first retina, vitreous original papers session (10:00 a.m.-12:15 p.m.). Where: Room 255. Access: Free.
Return to the OR After Macular Surgery: IRIS Registry Analysis. When: Tuesday, Nov. 14, 11:15-11:22 a.m., during the second retina, vitreous original papers session (10:15 a.m.-12:30 p.m.). Where: Room 255. Access: Free. |
Small-gauge better? “I pursued this research because I wanted accurate data for conducting surgical evaluations,” said Dr. Parke, who practices in Minneapolis. “But what interested me most was whether the transition from 20-gauge to small-gauge surgery had translated into a lower rate of postoperative retinal detachments (RDs).” In the study, about 2% of eyes undergoing surgery for either a macular hole or epiretinal membrane required RD repair—low, but not as low as previous small series had indicated, he said.
During the study time frame (from January 2013 through June 30, 2015), the IRIS Registry lacked the capacity to extract data such as surgical techniques being used, said Dr. Parke. However, this period could serve as a proxy for small-gauge surgeries, given that most retina surgeons were conducting them during this time, he said.
Visual results. Overall, eyes requiring second surgeries had worse visual outcomes. When a second noncataract surgery wasn’t needed, the last best-corrected visual acuity (BCVA) was 20/72 for macular hole and macular pucker surgeries. When a noncataract second surgery was needed, the BCVA was 20/155.
More at the Meeting
Want to access big data for research? Learn more at Research to Prevent Blindness–AAO IRIS Registry Grant Program (Spe25). When: Monday, Nov. 13, 10:15-11:15 a.m. Where: Room 338. Access: Free.
|
Lessons learned. Because clinical registries depend upon real-world physicians, said Dr. Parke, the data will always be less clean than with a curated prospective study. For this reason, miscoding or erroneous charting—as well as patients moving to practices that were not participating in the registry—may have affected the data.
“But the hope is that the power is great enough to minimize or render that concern irrelevant,” said Dr. Parke. “I think we can now tell our patients that there is approximately a 5%-6% chance they will need a second retina surgery and a 2% chance that a serious complication will occur after surgery.” Said another way, macular surgeries have a 94% success rate. “And considering prior studies and the fact that this was real-world data, that is better than I thought it would be.”
—Annie Stuart
___________________________
Relevant financial disclosures—Drs. Parke and Willis: None.
For full disclosures and disclosure key, see below.

More from this month’s News in Review