By Enchun M. Liu, MD, and Richard J. Rothman, MD
Edited by Steven J. Gedde, MD
Download PDF
All Bob Loblaw* wanted was a new pair of glasses. A week prior to seeing us, Mr. Loblaw paid a visit to his regular eye doctor because he felt he was overdue for an eye exam. He now found himself in our clinic being evaluated for a “suspicious lesion” in his right eye. Mr. Loblaw was a 32-year-old Caucasian man who had no visual complaints and was anxious about the possible news he could receive in our office. He was mildly myopic—which is why he was wearing glasses—but his ocular history was otherwise unremarkable. His only other medical history included a hernia repair and bowel surgery.
The Eye Exam
Mr. Loblaw’s best-corrected visual acuity was 20/20 in both eyes, and there was no afferent pupillary defect in either eye. His intraocular pressure by applanation was 19 mmHg in the right eye and 20 mmHg in the left eye. His anterior segment examination was unremarkable. On dilated funduscopic examination, his vitreous was clear in both eyes.
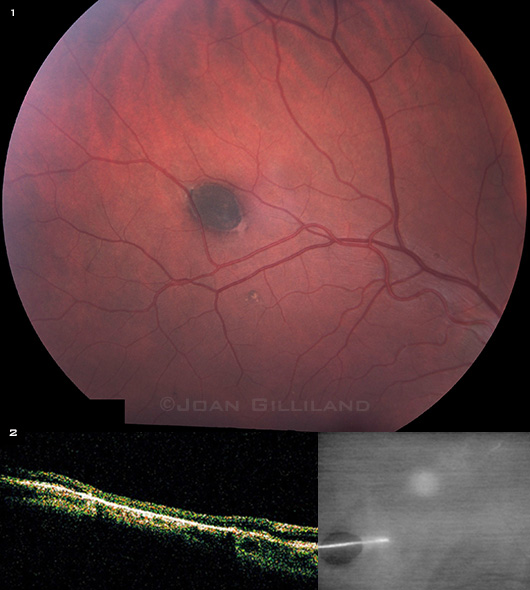
We found the lesion of concern in the midperiphery along the superotemporal arcade in the right eye (Fig. 1). Optical coherence tomography (OCT) over the lesion showed a hyper-reflective retinal pigment epithelial (RPE) layer with thinning of the overlying neurosensory retina (Fig. 2).
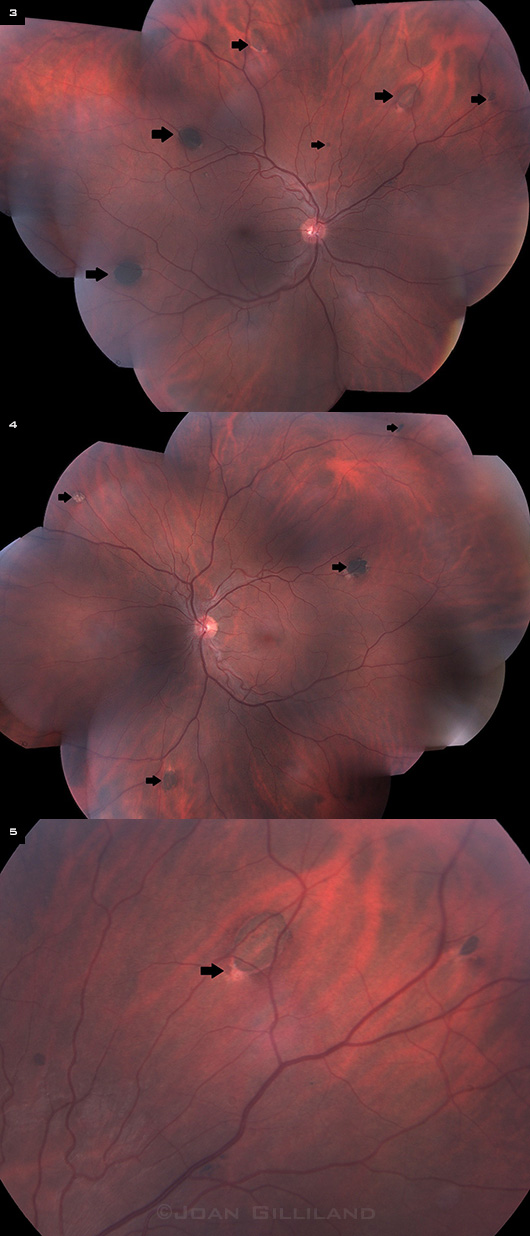
We also noted that Mr. Loblaw had multiple similar darkly pigmented lesions scattered throughout the posterior pole and midperiphery in both eyes (Figs. 3, 4).
On closer examination, we could see that they were oval in shape, with a tapered area of depigmentation at the margins of the lesions (Fig. 5).
Differential Diagnosis
The differential diagnosis for multiple hyperpigmented lesions in the fundus includes choroidal nevi, RPE hyperplasia secondary to previous trauma or inflammation, pigmented lattice degeneration, congenital hypertrophy of the retinal pigment epithelium (CHRPE), multifocal CHRPE (“bear tracks”), malignant melanoma of the choroid, and RPE hamartomas related to familial adenomatous polyposis (FAP). Upon further questioning of our patient, he revealed that he has a strong family history of FAP, and he had a prophylactic colectomy a few years ago. Both his brother and his father had numerous colonic polyps, and his uncle was treated for colorectal cancer.
|
What's Your Diagnosis?
|
 |
|
Mr. Loblaw was referred to us for evaluation of (1) a hyperpigmented lesion along the superotemporal arcade in his right eye. (2) OCT over this pigmented lesion, showing hyperreflectivity of the RPE and overlying thinning of the neurosensory retina.
|
Discussion
FAP is an autosomal dominant condition caused by a mutation in the adenomatous polyposis coli (APC) tumor suppressor gene located on chromosome 5q21.1 Affected patients have hundreds to thousands of adenomatous polyps, mostly in the large intestine, that have nearly 100 percent progression to colorectal cancer if left untreated. When there are extracolonic manifestations (such as desmoid tumors, osteomas, dental anomalies, and soft-tissue tumors) in addition to intestinal polyps, a diagnosis of Gardner syndrome can be made.1
FAP or CHRPE? FAP has commonly been associated with CHRPE.1 However, histopathologic comparison of the fundus lesions in FAP and CHRPE shows distinct differences.2,3
Histopathologic differences. CHRPE lesions appear as tall RPE cells filled with large hypertrophic melanosomes. The pigmented fundus lesions in FAP have three basic configurations on histopathology:
- a monolayer of hypertrophic cells,
- a mound of RPE cells interposed between the basement membrane of the RPE and the inner collagenous layer of Bruch’s membrane, or
- a multilayered mound of hyperplastic cells.2,3
All three are thought to be due to a generalized defect in melanogenesis from the underlying APC gene mutation.
Unlike those seen in CHRPE, the pigmented fundus lesions in FAP represent benign hamartomatous malformations of the RPE. In a review of 132 patients previously diagnosed with solitary or multifocal CHRPE, Shields and coworkers found that none of these patients had a history of FAP, Gardner syndrome, or intestinal cancer.4 In an effort to correctly differentiate the pigmented fundus lesions in FAP from CHRPE, the same authors have suggested calling these lesions RPE hamartomas associated with FAP, or RPEH-FAP.5
Clinical differences. CHRPE lesions are flat and darkly pigmented, have well-delineated smooth borders, and are often surrounded by a halo of depigmentation. With time, they may show scalloping or depigmented lacunae within the lesion.
Multifocal CHRPE are grouped in a sector or quadrant of the fundus and are characterized by a larger lesion surrounded by several smaller ones. This appearance resembles an animal paw or footprint, and thus they are commonly referred to as “bear tracks.”
Both solitary CHRPE and its multifocal variant tend to be unilateral, and the potential for malignant transformation is extremely rare.5
RPEH-FAP lesions are bilateral and haphazardly distributed throughout the fundus. They are generally smaller and more ovoid than CHRPE and have an irregular border. There is a characteristic area of depigmentation at one edge of the lesion in the shape of a comma or fish tail (Fig. 5).
RPE hamartomas are found in 70 to 80 percent of patients with FAP.1 These lesions are usually present at birth and often precede the development of intestinal polyps; thus, their presence on funduscopic examination can be a valuable aid in the diagnosis of FAP in at-risk family members.1,2 When there are multiple pigmented lesions in both eyes (usually four or more in each eye), these clinical markers have 95 to 100 percent specificity for FAP.1
Patient counseling. Although the difference between CHRPE and RPEH-FAP is subtle clinically, it is nonetheless important to make the distinction because of its implications for patient counseling. Patients found to have solitary or multifocal CHRPE on ophthalmoscopy can be counseled that they do not have an increased risk of colon cancer compared with that of the general population. However, patients who have multiple bilateral pigmented lesions with characteristic fish-tail margins should undergo a thorough family history evaluation in addition to recommendation for a screening colonoscopy.
 |
|
WE NOTE ADDITIONAL LESIONS. (3,4) Multiple hyperpigmented lesions are randomly distributed throughout the fundus in the both eyes (arrows). (5) A higher magnification of one of the fundus lesions showing fish-tail depigmentation at the margin (arrow).
|
Our Patient
When we saw Mr. Loblaw, he had already been treated with a colectomy for a known diagnosis of FAP, but he did not have any other extracolonic manifestations of Gardner syndrome. We told him that his fundus lesions are known to be associated with FAP, and he was relieved to hear that they are benign in nature. We recommended routine follow-up in one year or as needed.
___________________________
* Patient name is fictitious.
___________________________
1 Galiatsatos P, Foulkes WD. Am J Gastroenterol. 2006;101(2):385-398.
2 Traboulsi EI et al. Am J Ophthalmol. 1990;110(5):550-561.
3 Kasner L et al. Retina. 1992;12(1):35-42.
4 Shields JA et al. Ophthalmology. 1992;99(11):1709-1713.
5 Shields JA, Shields CL. Tumors and related lesions of the pigment epithelium. In: Shields JA, Shields CL, eds. Intraocular Tumors: An Atlas and Textbook. Philadelphia: Lippincott Williams & Wilkins; 2008:442.
___________________________
Dr. Liu is a vitreoretinal fellow and Dr. Rothman is a vitreoretinal specialist at The Retina Institute in St. Louis, Mo. They report no related financial interests.