Download PDF
An old foe—syphilis—has reemerged. And as a Canadian team of ophthalmologists recently found, there’s no such thing as a “typical” patient with ocular syphilis.1
“The big surprise was the variety in affected patients—male/female, young/old, single/married,” said Lulu Bursztyn, MD, MSc, FRCSC, at Western University in London, Ontario, Canada. “There is no reason to only test certain populations, as anyone can be infected.”
What sparked the study? “I had seen a few referrals from experienced ophthalmologists who were stumped,” Dr. Bursztyn said. Before too long, she realized that other clinicians were no longer thinking about syphilis, “despite the fact that it has clearly been on the rise over the past decade.”
In Canada, syphilis rates more than doubled from 2008 to 2017.1 And in the United States, the numbers of cases reported to the CDC increased by 81% from 2014 to 2018.2 “After an outbreak was officially declared in our region (London-Middlesex) in 2019, it was clear that more and more cases were going to surface, so we wanted to use these cases to help educate others,” Dr. Bursztyn said.
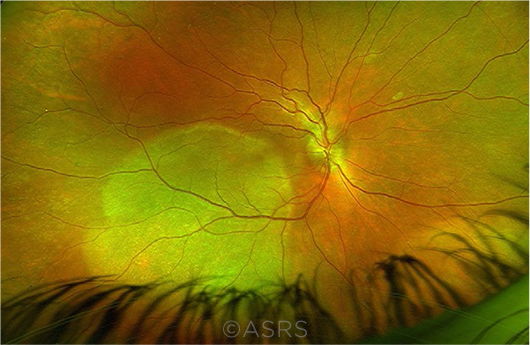 |
SUSPICION. Posterior placoid chorioretinopathy, seen in a 44-year-old woman who initially denied typical symptoms of syphilis. This image was originally published in the ASRS Retina Image Bank. John S. King, MD, Kent Zocchi, MD, Ahmed Sallam, MD, and Shree Karup, MD. Posterior Placoid Chorioretinopathy. Retina Image Bank. 2020; Image Number 69417. © The American Society of Retina Specialists.
|
Signs and symptoms. Dr. Bursztyn and her coauthors assembled a series of 26 cases of ocular syphilis, discussing five in detail. Although two of the five had “typical” features of ocular syphilis (e.g., optic neuritis, uveitis), the others did not. “There really were no pathognomonic features, and I think we demonstrated the wide variety of both symptoms and signs in our paper,” she said.
Take-home message. “The primary message is that as the prevalence of syphilis continues to increase, ophthalmologists should consider syphilis in the differential diagnosis of disease affecting any ocular structure,” Dr. Bursztyn said.
What about adding sexual history screening to the medical history? For instance, of the 26 cases presented in this report, only 12 patients disclosed risk factors for syphilis—and of these, only three disclosed their risk factors before diagnosis. However, as the authors pointed out, “patients may be reluctant to disclose [sexual history] even to focused questioning.”1 A simpler solution, then, would be to add serologic syphilis screening to any atypical case of uveitis or optic neuritis, regardless of any identified risk factors, they said.
And as Dr. Bursztyn noted, “The treatment is cheap, simple, and effective, so there is significant benefit of making the correct diagnosis.”
—Jean Shaw
___________________________
1 Schulz DC et al. Can J Ophthalmol. 2021;56(5):283-293.
2 Ghanem KG et al. N Engl J Med. 2020;382(9):845-854.
___________________________
Relevant financial disclosures: Dr. Bursztyn— None.
For full disclosures and the disclosure key, see below.
Full Financial Disclosures
Dr. Ambati iVeena: O; NEI: S; Research to Prevent Blindness: S.
Dr. Bursztyn None.
Dr. Hunter Lippincott Williams & Wilkins: P; Luminopia: C,O; Rebion: C,O,P; Slack: P.
Dr. Shen American Glaucoma Society: S; Topcon: S.
Disclosure Category
|
Code
|
Description
|
| Consultant/Advisor |
C |
Consultant fee, paid advisory boards, or fees for attending a meeting. |
| Employee |
E |
Employed by a commercial company. |
| Speakers bureau |
L |
Lecture fees or honoraria, travel fees or reimbursements when speaking at the invitation of a commercial company. |
| Equity owner |
O |
Equity ownership/stock options in publicly or privately traded firms, excluding mutual funds. |
| Patents/Royalty |
P |
Patents and/or royalties for intellectual property. |
| Grant support |
S |
Grant support or other financial support to the investigator from all sources, including research support from government agencies (e.g., NIH), foundations, device manufacturers, and/or pharmaceutical companies. |
|
More from this month’s News in Review