Download PDF
It has been estimated that a single phacoemulsification procedure, with its plethora of disposable supplies and medications, generates as much greenhouse gas emissions as a 310-mile car trip.1 Now, more than 1,200 cataract surgeons and an additional 300 OR nurses and administrators indicated that they would welcome the opportunity to shrink this carbon footprint by reusing many surgical instruments, supplies, and medications instead of discarding them after every surgery.2
The responses were elicited in an online survey developed by the Ophthalmic Instrument Cleaning and Sterilization (OICS) Task Force. Members of the task force represent the Academy, the American Society of Cataract and Refractive Surgery, the Outpatient Ophthalmic Surgery Society, and the Canadian Ophthalmological Society, said David F. Chang, MD, task force cochair. “There is strong consensus and support for tackling this problem of unnecessary surgical waste,” said Dr. Chang, who practices in Los Altos, California.
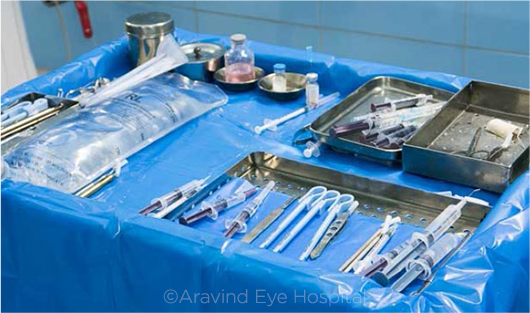 |
REUSE. Two-thirds of those surveyed said that more surgical instruments and supplies should be reused.
|
Time for action. “There were some significant surprises” in the survey results, Dr. Chang said. “I think many people in industry believe that physicians want more single-use, disposable instruments. But our survey showed that 10 times as many surgeons would choose a reusable instrument over a disposable equivalent instrument, assuming they were of equal cost and functionality, thereby dispelling the notion that the market wants more single-use products.”
The survey found that 93% of respondents believe that OR waste is excessive and should be reduced; 78% state that more supplies should be reused; 91% are concerned about global warming and climate change; and 87% want medical societies to advocate for reducing the surgical carbon footprint.
In other findings, 95% of those surveyed were willing to reduce waste by eliminating the full-body drape and by having the OR staff wear the same surgical mask all day; 91% were willing to reprocess and reuse single-use instruments; 93% were willing to send topical medications home with patients; and 97% were willing to save and donate unused surgical supplies.
Barriers to address. Key barriers to putting these strategies into action in the United States are manufacturers’ concerns about liability and the instructions for use (IFUs) that surgeons must follow, Dr. Chang said. Per the IFUs, off-label reuse is not at the surgeon’s discretion. “A strong majority of surgeons we surveyed feel that both profit incentive and liability reduction are behind that type of labeling and that it’s not really for any proven safety benefit,” Dr. Chang said. “There basically is no good evidence that reusing many single-use devices—such as metal blades, phaco tips, and tubing—is dangerous.”
What prompted the survey? In the task force’s original work—writing guidelines for the cleaning and sterilization of intraocular surgical instruments3—members cited evidence from India’s Aravind Eye Care System indicating that careful reuse and resterilization strategies could minimize waste and save money4 while still keeping the endophthalmitis rate quite low,5 Dr. Chang noted. Thus, the group launched this survey to find out if cataract surgeons in North America would support the environmentally friendlier approach taken at Aravind, he said.
Moving forward. Dr. Chang said he hopes the survey’s results will catalyze a movement toward a smaller carbon footprint for U.S. cataract surgery. “While a survey doesn’t solve the problem, I think it illuminates it and lays out potential solutions that the majority of ophthalmologists agree should exist: first, greater discretion to reuse things, based on our best clinical judgment, and second, manufacturers being more conscious of wasteful packaging and providing us with more options for reusable instruments and multiuse pharmaceuticals.”
—Linda Roach
___________________________
1 Morris DS et al. Eye. 2013;27(4):495-501.
2 Chang DF, Thiel CL. J Cataract Refract Surg. 2020;46(7):933-940.
3 Chang DF, Mamalis N. J Cataract Refract Surg. 2018;44(6):765-773.
4 Thiel CL et al. J Cataract Refract Surg. 2017;43(11):1391-1398.
5 Haripriya A et al. J Cataract Refract Surg. 2019;45(9):1226-1233.
___________________________
Relevant financial disclosures—Dr. Chang: Johnson & Johnson Vision: C.
For full disclosures and the disclosure key, see below.
Full Financial Disclosures
David F. Chang, MD Carl Zeiss: C; Eyenovia: O; iDrops: C,O; Ivantis: C,O; Johnson & Johnson Vision: C; Mynosys: C,O; Perfect Vision: C; PowerVision: C,O; Presbyopia Therapies: O; RxSight: C; Slack: P; Surface: O; Versant Ventures: O; Viewpoint: C,O.
Dr. Cheng None.
Dr. Huxlin Clerio Vision: O. Dr. Huxlin also is coinventor on U.S. Patent No. 7,549,743.
Dr. Medeiros Aerie Pharmaceuticals: C; Allergan: C,S; Annexon: C; Biogen: C; Carl Zeiss: C,S; Galimedix: C; Google: S; Heidelberg: S; IDx: C; nGoggle: P; Novartis: S; Stealth Biotherapeutics: C; Reichert: C,S.
Disclosure Category
|
Code
|
Description
|
| Consultant/Advisor |
C |
Consultant fee, paid advisory boards, or fees for attending a meeting. |
| Employee |
E |
Employed by a commercial company. |
| Speakers bureau |
L |
Lecture fees or honoraria, travel fees or reimbursements when speaking at the invitation of a commercial company. |
| Equity owner |
O |
Equity ownership/stock options in publicly or privately traded firms, excluding mutual funds. |
| Patents/Royalty |
P |
Patents and/or royalties for intellectual property. |
| Grant support |
S |
Grant support or other financial support to the investigator from all sources, including research support from government agencies (e.g., NIH), foundations, device manufacturers, and/or pharmaceutical companies. |
|
More from this month’s News in Review