By Ashvini K. Reddy, MD, and Christopher Weaver, MD
Edited By: Steven J. Gedde, MD
Download PDF
Jack Hanson,* a 57-year-old African-American man, presented to his local ophthalmologist’s clinic with a two-week history of red, profoundly light-sensitive, painful eyes. In addition, both of his ears hurt badly and were tender. He had experienced ear pain twice previously and told his physician that he felt the eye and ear problems were connected somehow—and he really wanted to determine the cause of his symptoms so he could avoid future episodes.
What We Saw
History. Mr. Hanson’s medical history included hypertension controlled with hydrochlorothiazide and an ocular history of presbyopia. His family history was remarkable for glaucoma in his maternal grandmother.
When we asked about other health problems, Mr. Hanson reported that the auricles of his ears seemed swollen and painful on two occasions in the past, but that these episodes had not involved eye inflammation. The first episode had occurred three years earlier and was resolved with steroids prescribed by his family physician. The second episode of auricular inflammation occurred a year ago and was associated with fever, myalgia, and joint pain as well as a 30-lb weight loss.
He specifically denied prior tuberculosis, immunocompromised state, sinus pain, ulcers, joint pain, and any difficulty breathing.
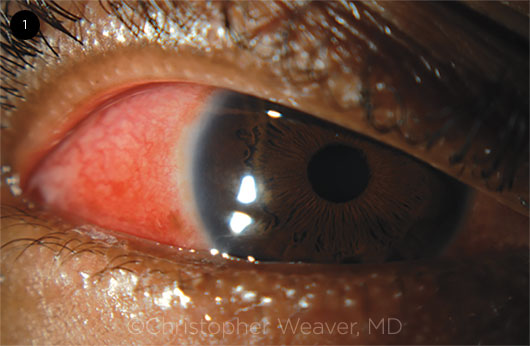
Exam. Our examination revealed that his visual acuity was 20/20 in both eyes with no afferent pupillary defect in either eye. Visual fields by confrontation were normal, as were ocular motility, intraocular pressure, and color vision. The external examination was remarkable for thickened, tender auricles bilaterally and 2+ diffuse scleritis of both eyes without proptosis (Fig. 1). Both of his globes were tender to light touch.
The anterior segment examination showed a clear cornea without thinning or keratic precipitates. We saw no cellular reaction in the anterior chamber, and no iris nodules or atrophy were present. Mr. Hanson had trace nuclear sclerosis and no vitritis.
The fundus examination was normal in both eyes, without serous retinal detachments, disc edema, or retinal vasculitis. He had no facial deformity, apart from his ear swelling, and no joint tenderness.
 |
|
SCLERITIS. Bilateral eye redness that did not blanch with phenylephrine.
|
Differential Diagnosis
Given his auricular involvement, a diagnosis of relapsing polychondritis (RP) was at the top of our differential. During a thorough workup, we also evaluated Mr. Hanson for other causes of scleritis, including infectious diseases and vasculitis. Laboratory testing for rheumatoid factor, syphilis serologies, antinuclear antibody (ANA), and antineutrophilic cytoplasmic antibodies (ANCA) were negative, and a chest x-ray was normal. A biopsy of the auricular cartilage was performed for definitive diagnosis. The pathology report confirmed a mixed perichondral infiltrate of lymphocytes and other inflammatory cells at the chondrodermal junction consistent with RP.
Discussion
RP is an inflammatory disorder believed to be caused by antibodies against type II collagen.1,2 Sudden onset of ear involvement is frequently the presenting symptom, although patients may also present with concomitant arthritis. Other common manifestations include recurrent inflammation of cartilaginous tissues: ears, nose, peripheral joints, eyes, and the laryngotracheobronchial tree. Patients may develop cardiovascular disease, and one-third of patients have vasculitis and autoimmune rheumatic disease.
Diagnostic criteria for RP include recurrent chondritis of both auricles, nonerosive inflammatory polyarthritis, chondritis of nose cartilage, ocular inflammation (keratitis, scleritis, episcleritis, uveitis), laryngotracheitis, and vestibulocochlear inflammation and damage. Although not diagnostic, patients often have anemia, elevations in erythrocyte sedimentation rate and C-reactive protein, and leukocytosis. Antibodies to collagen II are found in 40% to 50% of patients.
Eye involvement. Ocular involvement occurs in 60% of reported patients with RP and usually manifests as scleritis, episcleritis, keratitis, or conjunctivitis, but it can present with multiple findings.3 Scleritis and episcleritis often occur concomitantly with nose and joint inflammation. Compared with scleritis associated with other systemic immune diseases, scleritis associated with RP is more often bilateral, necrotizing, recurrent, and associated with decreased vision. Furthermore, over 60% of patients with RP-associated scleritis also have another systemic immune disease.3 Patients can also develop retinal vasculitis and optic neuritis.
The classic sign of scleritis is edema in the episcleral and scleral tissues with injection in the superficial and deep episcleral vessels. Ocular complications of scleritis include interstitial keratitis, marginal corneal ulcers, peripheral ulcerative keratitis, anterior uveitis, and glaucoma. Posterior scleritis may be associated with a higher risk of macular edema, exudative retinal detachment, and vitritis.
Evaluation. Because scleritis can be associated with various underlying disorders, the evaluation may include chest x-ray, urinalysis, serum creatinine, ANCA, syphilis serology, and Quantiferon testing (for tuberculosis). Other tests may be indicated as dictated by history and examination findings: radiographic imaging of the sinuses (for granulomatous polyangiitis involving the sinuses), ANA and complement proteins C3 and C4 (for systemic lupus erythematosus), rheumatoid factor and anticyclic citrullinated peptide (for rheumatoid arthritis), and imaging of the trachea (for RP). Additional imaging may be indicated to evaluate for associated orbital inflammation. Ultrasound can confirm posterior involvement, if suspected.
Management. RP-related scleritis should be managed with a multidisciplinary team, given the risk of systemic disease. The team may include rheumatologists and otolaryngologists. Treatment for RP-related scleritis may involve use of nonsteroidal anti-inflammatory drugs, steroids, or immunosuppressants. Indications for immunosuppression include failure to control disease with steroids, health-threatening steroid adverse effects, or an autoimmune condition requiring steroid-sparing therapy.
Specific agents may include the following:
- Indomethacin 25 mg orally, four times daily or naproxen 500 twice daily
- Prednisone 1 mg/kg orally daily
- Antimetabolites: methotrexate, azathioprine, or mycophenolate
- Biologics: adalimumab or infliximab
- Alkylating agents: cyclophosphamide or chlorambucil
Some patients may achieve remission following therapy. With appropriate medication and follow-up, the prognosis can be good.
Lethal sequela. It is important for physicians to be aware of RP because respiratory involvement can be fatal. Up to 25% of patients present initially with respiratory symptoms. Laryngotracheobronchitis can manifest with hoarseness, nonproductive cough, dyspnea, wheezing, and inspiratory stridor with tenderness over the thyroid cartilage and trachea. Patients are at risk for upper airway collapse and infections.
Our Patient’s Course
Mr. Hanson was educated about RP, especially the risk of life-threatening tracheal involvement and the need to seek emergency care if he suspected any problems. Once the diagnosis was confirmed, he was referred to the rheumatology and pulmonary services for coordinated care and was started on treatment with oral prednisone and methotrexate with folic acid. This regimen resulted in good control of his inflammatory disease, and he had no further episodes of scleritis or auricular inflammation. He continues to be followed for any signs of inflammation.
Conclusion
RP is a rare inflammatory disorder directed against type II collagen that can present as ocular inflammatory disease. It is important to recognize the condition early because respiratory involvement can be fatal if untreated. Multidisciplinary involvement with immunosuppression is generally needed to control systemic disease.
___________________________
*Patient name is fictitious.
___________________________
1 Borgia F et al. Biomedicines. 2018;6(3):E84.
2 Zampeli E, Moutsopoulos HM. Rheumatology (Oxford). 2018;57(10):1768.
3 Sainz-de-la-Maza M et al. Br J Ophthalmol. 2016;100(9):1290-1294.
___________________________
Dr. Reddy is associate professor of ophthalmology at Dean McGee Eye Institute in Oklahoma City, Okla. Dr. Weaver is a practicing ophthalmologist at Hecker Eye Associates in Greensboro, N.C. Financial disclosures: None