By Houman D. Hemmati, MD, PhD, and Kathryn A. Colby, MD, PhD
Edited by Ingrid U. Scott, MD, MPH, and Sharon Fekrat, MD
This article is from October 2012 and may contain outdated material.
A chemical injury of the eye presents a genuine, acute emergency and requires immediate evaluation and management.1 Although the most devastating sequelae of chemical injuries—corneal melt, limbal stem cell deficiency, and glaucoma—tend to occur over the long term, effective diagnosis and treatment in the minutes and days following the initial injury often dictate the clinical course and can prevent tragic consequences.
The goals of therapy are to restore corneal clarity, normalize the ocular surface, and prevent glaucomatous optic nerve damage. This article presents a review of the common etiologies and mechanisms of chemical injuries to the eye, clinically relevant classifications of these injuries, and management strategies, with a focus on the acute treatment of chemical burns.
Mechanisms of Injuries
Chemical injuries most commonly affect young men. At least 90 percent of these injuries occur as accidental exposures. They typically take place in industrial settings and often occur despite the use of safety glasses.
Acid burns. These burns are generally less destructive than their alkali counterparts and usually occur with exposure to strong acids that have a pH of less than 4. Hydrochloric acid (used to clean swimming pools) and sulfuric acid (found in car batteries) are some of the more common acids encountered in emergency settings.
Acids tend to denature, coagulate, and precipitate corneal proteins on contact, creating a barrier that prevents deeper penetration of the acid. This protein coagulation produces the ground-glass appearance of the cornea often seen in severe acid burns. Hydrofluoric acid (used in antirust solutions and glass etching) is an exception to this: The fluoride ion rapidly penetrates the entire thickness of the cornea through cell membranes, causing significant corneal and anterior segment destruction.
Systemic acid burns covering more than 2 percent of the body surface area are associated with severe hypocalcemia and can have fatal neurological, respiratory, and cardiovascular consequences.
Alkali burns. Chemicals commonly responsible for alkali injuries of the eye include sodium hydroxide (lye; found in drain cleaners and industrial cleaning solutions), ammonia (found in household cleaning solutions and fertilizers), and calcium hydroxide (lime; found in cement and plaster).
Alkali chemicals are lipophilic and penetrate cell membranes through saponification of membrane lipids. Hydroxyl ions, which are common to many alkali chemicals, denature the collagen matrix of the cornea and facilitate further chemical penetration. Affected tissues can undergo liquefactive necrosis, in which the inflammatory response triggers release of proteolytic enzymes, leading to a cascade of damage. Potent alkalis can reach the anterior chamber in less than 15 seconds, causing destruction of tissues in the cornea and anterior chamber (including the trabecular meshwork, lens, and ciliary body). Penetration can continue to occur long after the initial exposure takes place.
Direct chemical damage to the conjunctiva can lead to scarring, forniceal shortening, symblepharon formation, and cicatricial ectropion or entropion. Destruction of conjunctival goblet cells can contribute to a lifetime of dry eye. Severe burns to the limbal stem cells may cause limbal stem cell deficiency, resulting in opacification and eventual neovascularization of the cornea due to loss of corneal epithelial progenitor cells. Moreover, glaucoma can arise from injury to the trabecular meshwork, contraction of the anterior structures of the globe, and possibly chemical and inflammatory damage to the ganglion cells in the posterior segment of the eye.
 |
|
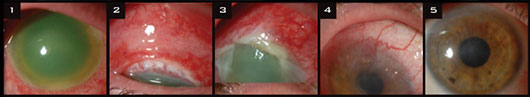
ALKALI BURN. When this patient with a grade III alkali burn was initially evaluated,(1) corneal clouding and intense intraocular inflammation were evident, (2) along with limbal ischemia. At this time, vision was counting fingers. (3) One week later, the first amniotic membrane transplantation was performed for poor epithelial healing; all told, two amniotic membrane grafts were required. (4) One month later. (5) Two months later, the patient’s vision had improved to 20/25 with an intact ocular surface. No further surgery was needed.
|
Classification of Severity
Numerous classification schemes exist to describe chemical injuries to the ocular surface, guide management, and assess prognosis. The common factor among the various schemes is a clinical determination of the extent of conjunctival, limbal, and corneal (epithelial and stromal) damage at the time of initial assessment. Key factors, including presence and degree of limbal ischemia and corneal haze, are used to classify the injury. The depth of corneal involvement, including presence of endothelial injury, may also be a prognostic indicator.
The Hughes classification scheme, as modified by Thoft, divides chemical injuries into four categories in order of worsening severity and prognosis.1
Grade I. Injuries in this category are confined to the corneal epithelium; there is no limbal ischemia, and the cornea is totally clear. These injuries carry an excellent long-term visual prognosis.
Grade II. These injuries are significant for mild corneal haze, which permits a good view of anterior chamber structures, and focal limbal ischemia. The prognosis is good, although the cornea may develop focal haze and neovascularization at the site of limbal stem cell loss.
Grade III. These injuries are characterized by significant ischemia of most of the limbus, as well as profound corneal haze that limits the view of anterior chamber structures. Due to extensive limbal stem cell loss, patients with grade III injuries have a guarded prognosis. As corneal epithelium cannot regenerate, the ocular surface must be conjunctivalized to maintain tectonic stability. This occurs at the expense of visual acuity. Improvement in vision is often not achieved without a surgical procedure.
Grade IV. These injuries carry the worst prognosis. In addition to total loss of limbal stem cells, there is destruction of the proximal conjunctival epithelium. The cornea is completely opaque and porcelainized, and it is extremely prone to melting in the acute or intermediate time frames after injury. Visual recovery may not be possible.
Initial Evaluation
Emergency response. Initial treatment of any chemical burn should begin immediately at the time and place of the injury. The affected eye(s) should be irrigated copiously with any available noncaustic fluid at the injury site and throughout transport to the hospital. Irrigation should continue at the hospital until the pH of the ocular surface has normalized to a range of between 7.0 and 7.2. Some evidence has shown a benefit when a borate buffer (Cederroth Eye Wash) is used for irrigation, compared with saline or tap water.2
The pH should be rechecked with narrow-range pH test strips (between 6 and 8) at 15- to 30-minute intervals after stabilization to confirm that there has not been a change outside normal range. Such a change can signify the presence of a hidden particle in the eye that continues to elute chemicals onto the ocular surface. A Morgan lens may be used with topical anesthesia to facilitate the irrigation process in a patient who is uncomfortable.
Ophthalmic examination. Once pH has been neutralized reliably, a complete ophthalmic examination is required to characterize the extent of the injury and plan further treatment. The initial screen should include a thorough sweep of fornices with eyelid eversion to detect and remove occult particles such as lime and plaster.
As discussed above, it is important to thoroughly assess the presence and degree of limbal ischemia as well as the degree of corneal epithelial defect and opacification. In eyes with chemosis, it is necessary to gently push aside chemotic conjunctiva from the limbus with a sterile ophthalmic sponge to gain good access to the limbus. Fluorescein should be used to assess the status of the corneal and conjunctival epithelium, with the knowledge that fluorescein staining may be difficult to appreciate in the presence of a complete epithelial defect. Intraocular pressure (IOP) should be checked, as serious chemical burns can greatly increase or lower the pressure. Examination of the rest of the eye should be attempted, although the initial exam may be limited due to the view through the cornea and patient discomfort. Finally, even in cases of purported unilateral chemical injury, the contralateral eye must still be examined carefully (including a check of the pH) in order to confirm that both eyes are not involved.
Recommended Treatment
Treatment is based on the grade of injury.1 For most injuries, the goal of treatment is to promote epithelial healing and reduce pain while decreasing inflammation and preventing bacterial superinfection.
Grade I. For grade I injuries, a mild topical antibiotic ointment such as bacitracin or erythromycin typically is prescribed, along with preservative-free artificial tears as needed. A topical steroid such as prednisolone acetate, applied four times a day for approximately a week, is usually sufficient to control inflammation and facilitate re-epithelialization. For comfort, a topical cycloplegic agent such as cyclopentolate 1 percent three times a day is often sufficient. Patients with grade I injuries should be followed at least every other day until the entire ocular surface has healed; they should continue to be followed long-term to assess for dry eye and other issues.
Grades II to IV. For more severe burns, the control of inflammation in the acute phase, particularly the first week after injury, is of utmost importance. Hourly application of topical prednisolone acetate 1 percent is recommended while the patient is awake for the first seven to 10 days. This should be rapidly tapered between days 10 and 14 to minimize the risk of corneal melting.
A long-acting cycloplegic such as scopolamine hydrochloride or atropine sulfate should be used for comfort, along with oral pain medications. To prevent suprainfection in cases with complete epithelial loss, a topical broad-spectrum antibiotic (such as a fluoroquinolone) may be given four times a day. An oral tetracycline derivative (such as doxycycline) is given to reduce the risk of corneal melting through inhibition of matrix metalloproteinases. Animal data indicate that topical and/or oral administration of high-dose vitamin C may prevent or delay ulceration; given the low risk of these agents, they may be employed with confidence. Finally, it is essential to control IOP, as more severe burns can lead to significant rises in pressure. Aqueous suppressants may be used.
Use of amniotic membrane. Some cornea specialists advocate early placement of amniotic membrane (such as Prokera) on the ocular surface in grade II, III, or IV burns, and the risks of doing so are low. However, the expense of Prokera is considerable, and its longevity is limited in very inflamed eyes.
Initial follow-up. Initially, patients with severe chemical injuries should be seen daily to assess epithelial healing, measure IOP, and monitor for progressive corneal melting. Once epithelial healing is proceeding satisfactorily, follow-up intervals can be increased, but frequent follow-up is essential until the epithelium is intact, especially if the patient remains on topical corticosteroids.
Topical corticosteroids are generally tapered after the first seven to 10 days postinjury, since after this period they may tip the balance of collagen synthesis and collagen breakdown unfavorably. If additional anti-inflammatory treatment is needed, a topical progestational steroid such as medroxyprogesterone 1 percent, which carries a much lower risk of inducing corneal melting, may be used. If, within 10 days of injury, the epithelium has failed to heal, surgical treatments may be considered.
Debridement and surgery. Necrotic corneal and/or conjunctival epithelium should be debrided with surgical sponges or excised at the slit lamp under topical anesthesia. If complete epithelial healing does not occur within the first several weeks after the injury, amniotic membrane should be applied directly on the cornea, using a purse-string fixation suture at the limbus.3 A Prokera device may also be considered.3
A further note regarding grade IV injuries: In addition to the treatment paradigm outlined in the Academy’sFocal Points,1 the globe may occasionally be stabilized by mobilizing and advancing posterior conjunctiva and Tenon’s capsule into the affected area to deliver healthy tissue and vasculature. However, the prognosis for grade IV injuries is guarded, even with appropriate management.
Learn More in Chicago
Pandora’s Box in Severe Ocular Chemical Injuries: The Entire Gamut of Management. Four experts explain what you must address during the acute phase of injury, before discussing the chronic phase. Topics include glaucoma, ocular surface reconstruction, visual rehabilitation, stem cell transplants, and keratoprosthesis. When: Tuesday, Nov. 13, 2-3 p.m. Where: Room S505ab. Access: Academy Plus course pass required.
|
Long-Term Management
In cases of severe unilateral injury, chronic limbal stem cell deficiency may be treated with limbal stem cell autograft (either direct or expanded in culture in vitro) from the healthy contralateral eye.4 If both eyes are involved, limbal stem cell allografts taken from a living relative or a cadaver may be used. Alternatively, cultured buccal mucosal autografts have been used with some success.
If significant corneal scarring or neovascularization is present, a corneal transplant may be required to restore vision once the ocular surface has stabilized. Because neovascularization reduces the likelihood of success of a traditional keratoplasty, due to an increased risk of graft rejection, a Boston keratoprosthesis may be considered.
Finally, management of glaucoma remains an important issue following chemical injury.5
___________________________
1 Colby K. Focal Points. 2010;28(1):1-14.
2 Dohlman CH et al. Cornea. 2011;30(6):613-614.
3 Fish R, Davidson RS. Curr Opin Ophthalmol. 2010;21(4):317-321.
4 Marchini G et al. Clin Experiment Ophthalmol. 2012;40(3):255-267.
5 Cade F et al. Cornea. 2011;30(12):1322-1327.
___________________________
Dr. Hemmati is a clinical fellow in ophthalmology and Dr. Colby is a cornea specialist; both are at Massachusetts Eye and Ear Infirmary in Boston. The authors report no related financial interests.