A 55-year-old man presents with sudden, painless blurred vision in his left eye
What is your diagnosis?
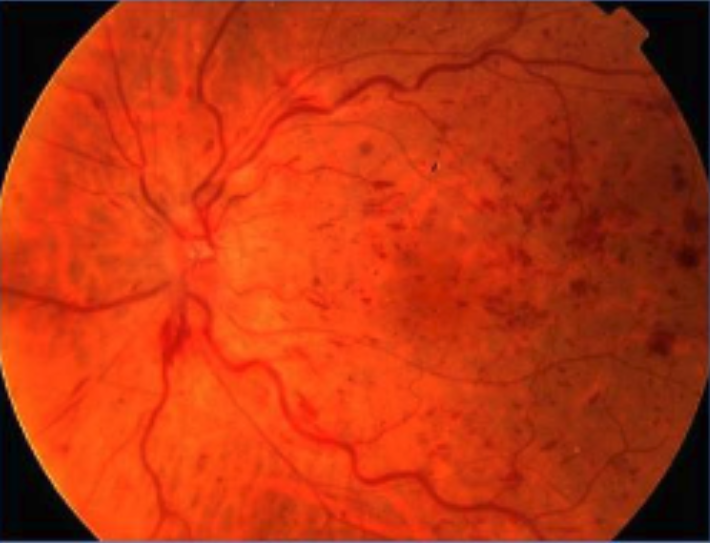
The diagnosis is...
![]()

The image is consistent with a diagnosis of a central retinal vein occlusion (CRVO) in the left eye.
- CRVO is a common cause of painless vision loss in older individuals but can occur in younger individuals as well. Patients typically present with painless sudden, unilateral, blurred, or distorted vision.
- The pathogenesis for CRVO is directly related to the central retinal artery, sharing the same adventitial sheath, where atherosclerotic changes to the artery compress the vein, leading to venous stasis, thrombosis, and ultimately occlusion (ie, Virchow’s triad).
- CRVO may either be nonischemic type or ischemic type. Ischemic CRVO portends a worse visual prognosis.
- Risk factors include age, hypertension, hyperlipidemia, diabetes mellitus, smoking, raised intraocular pressure, glaucoma, oral contraceptives, thrombophilia, coagulopathic diseases, and more.
What is the role of the primary care or emergency medicine physician?
![]()
- Refer the patient to the ophthalmologist urgently for a dilated eye examination to prevent vision loss.
- Patients with acute CRVO should also be evaluated by the medical team to work up potential underlying vasculopathic diseases, and/or ensure that any current systemic diseases are stable.
What is the role of the ophthalmologist?
![]()
- Perform a dilated eye examination with a slit-lamp microscope.
- Perform ocular imaging with fluorescein angiography (FA), optical coherence tomography, and/or fundus autofluorescence that often shows a classic “blood and thunder” image.
- FA can determine ischemic vs nonischemic causes.
- Ascertain whether there is any concomitant cystoid macular edema, retinal neovascularization, or neovascular glaucoma.
- Recommend that the patient undergo cardiovascular workup with a primary care physician (PCP).

What is the treatment?
![]()
- Monthly anti-vascular endothelial growth factor (anti-VEGF) or steroid intravitreal injections are needed when there is concomitant cystoid macular edema and/or neovascularization.
- Surgical/procedural interventions include laser photocoagulation and pars plana vitrectomy, especially in cases of severe vitreous hemorrhage.
- In the setting of neovascular glaucoma, intraocular pressure control is needed.
- Supportive treatment options vary, based on type and etiology of CRVO, such as low vision services and monocular precautions if the vision is permanently poor.

Learn more: Ophthalmology resources for medical students
![]()