Download PDF
Brolucizumab, a novel drug that blocks vascular endothelial growth factor (VEGF)–A, has been found to be noninferior to aflibercept at preserving vision in patients with active choroidal neovascularization (CNV) secondary to age-related macular degeneration (AMD).1 Published data from a phase 2 trial also suggest that patients treated every 8 weeks with brolucizumab might experience some advantages compared to patients injected with 2 mg of aflibercept, notably a more durable treatment effect and extended intervals between intravitreal injections.
Pharmacokinetics. Brolucizumab (also known as RTH258) is a humanized single-chain antibody fragment that inhibits all isoforms of VEGF-A with a molecular weight of 26 kDa.
“On a molar basis, 6 mg of brolucizumab equals approximately 12 times the 2.0-mg dose of aflibercept and 22 times the 0.5-mg dose of ranibizumab,” the authors wrote.1 “These attributes may confer potential advantages in the treatment of neovascular AMD. A small molecular weight and high drug concentration gradient between the vitreous and retina may support drug distribution into the retina. Assuming comparable half-life, higher molar doses of drug may be cleared more slowly from the eye, thus prolonging duration of action,” they explained.
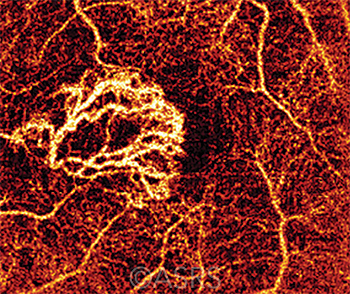 |
REDUCED DOSING? Early results indicate that brolucizumab may allow for an extended interval between intravitreal injections for CNV (shown here). This image was originally published in the ASRS Retina Image Bank. Timur Shaimov, Ruslan Shaimov, and Venera Shaimova. Type 2 Choroidal Neovascularization–Angio OCT. Retina Image Bank. 2015; Image Number 25033. © The American Society of Retina Specialists.
|
Study results. For this phase 2 study, researchers evaluated 89 patients, 44 of whom received injections of brolucizumab (6 mg). The remaining 45 received 2-mg injections of aflibercept.
Through 40 weeks of treatment, the brolucizumab group had more stable reductions in central subfield thickness (CSFT) and greater resolution of intra- and subretinal fluid. At week 40, fluid resolution had occurred in 61% of subjects receiving intravitreal brolucizumab, compared to 35% of the aflibercept patients.
With regard to unscheduled treatments, unplanned injections numbered 6 in the brolucizumab eyes and 15 in the aflibercept group. Furthermore, when the researchers extended the treatment interval to 12 weeks, approximately 50% of the evaluable brolucizumab eyes maintained their best-corrected visual acuity (BCVA) without requiring any unscheduled injections.
Additional results. In late June, Novartis released positive results from 2 phase 3 studies of brolucizumab. According to the company, researchers evaluated 3- and 6-mg doses of the drug and found that both doses provided excellent visual acuity and reduced injection burden when compared to aflibercept. However, the results have yet to be published.
Drug delivery. Brolucizumab’s small molecular size might give it another advantage in the future, said Pravin U. Dugel, MD, at Retinal Consultants of Arizona in Phoenix and the University of Southern California, in Los Angeles. Specifically, it’s possible that the drug could be delivered via an ocular implant. “We don’t have one yet [for anti-VEGF drugs], but I think we’re all convinced that one day we will. So, because of its size, brolucizumab would seem like it could be an ideal anti-VEGF agent to be packaged in this way.”
—Linda Roach
___________________________
1 Dugel PU et al. Ophthalmology. Published online May 24, 2017.
___________________________
Relevant financial disclosures—Dr. Dugel: Alcon: C; Allergan: C; Genentech: C; Novartis: C; Roche: C.
For full disclosures and disclosure key, see below.

More from this month’s News in Review