For this month’s YO Spotlight, we talk to John Cropsey, MD, a former Wills Eye Institute resident who is the only ophthalmologist at a Kenyan eye unit that is “the main referral center for roughly 10 million people.” Dr. Cropsey shares about how he entered medicine, what brought him to Kenya and the challenge of saying no.
1. Why did you become an ophthalmologist? I grew-up in Togo, West Africa, at a rural mission hospital that my parents helped start when I was four years old. My dad was a general surgeon and my mom was a nurse. The medical needs I saw were immense.
As I pursued a career to help meet that need, I asked several jungle mission surgeons, including my dad, what kind of doctor they would be if they could do it over again. They all independently said they would become ophthalmologists and return to Africa.
There is virtually no access to eye care in many parts of Africa, so my dad, a general surgeon, learned to do cataracts and trabs with loops! Even with their 10+ aphakic glasses, my dad said these were the most excited patients he'd ever seen. Helping these grandpas and grandmas see their grandchildren for the first time really touched my dad's heart.

Dr. Cropsey with some of his staff, prior to a surgical safari to Lake Tanganyika, Tanzania, by airplane and then helicopter.
2. What does a typical day look like for you? This year, I am the only ophthalmologist at Tenwek Eye Unit, the main referral center for roughly 10 million people. I have 15 amazing Kenyan staff, who make it all happen without it killing me, SO FAR.
Mondays we begin our day at 8 a.m. as a team, with reflections from the Bible, prayer and singing. This sets the tone for the week. We are here to love and serve our God and neighbors, the poor and blind.
From 8:30 a.m. to 9:30 a.m., I try to get a few administrative things done before the onslaught of patients begins! My ophthalmic clinical officer and ophthalmic nurses see most patients (cataracts, refractive error, allergies...) and save the more challenging cases for me to review (tumors, trauma, retina, neuro, plastics, cornea...). I see second opinions until about 1 p.m., take lunch at home with my family and then return to clinic from 2 p.m. until 5 p.m. to 7 p.m.
From Monday clinic's 100-plus patients, we will admit 30 to 50 patients for surgery (we have 20 beds). By the end of the day, we will have seen and managed problems from all age brackets, in every subspecialty, in their most advanced forms.
Tuesday, we start operating at 7:30 a.m. My clinical officer (equivalent to a physician’s assistant in the United States) does all of the manual small incision cataract surgeries (MSICS — sutureless extracap), while I tackle the NPO pediatric cases requiring general anesthesia: mostly congenital/developmental cataracts and trauma with the occasional glaucoma, retina, PK or strabismus case. We've done 180 pediatric cases in 2010 already, only two of those for strabismus.
We use retrobulbar blocks routinely on kids older than 8 years of age, limiting our need for ketamine/general anesthesia. Our record is doing a traumatic cataract with a retrobulbar block on a 4-year-old boy in South Sudan, where we had no other means of anesthesia. We bribed him with a bottle of Coke and a candy bar. We prayed like crazy, and he didn't budge!
Wednesday, my clinical officer finishes the cataracts and smaller cases while I face some of the longer subspecialty cases. Thursday, I finish up any surgeries still waiting from Monday, do ROP rounds in the nursery and try to do some administrative stuff. Friday is mainly post-op clinic. I take call for one week every other week, rotating with my clinical officer.
When possible, I love to join our community outreach program, which holds mobile clinics in the villages two to four times a week. A real treat is doing week-long surgical camps in remote parts of Africa. We typically can do 70 to 100 cataracts on these trips.
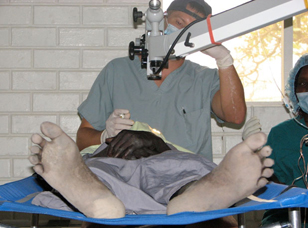
Performing MSICS on a patient in South Sudan in 100+ degree weather.
3. What do you like most about the organization/health system/region where you practice? I have the privilege of working with a team that has a vision to show the love of Jesus Christ through high-quality, compassionate eye care to those who would not otherwise have access to it.
Added perks: I eat every meal with my family, I rarely have to do paperwork for insurance companies because only 5 percent of my patients have insurance of any kind and, most days, I get to use every bit of knowledge that I've learned about life and eyes.
4. What’s your biggest frustration about the organization/health system/region where you practice? My biggest frustration is having to be the administrator of the eye unit in addition to being the leader and physician. I have poor natural administrative skills and little training. My staff and patients suffer because of it.
I mostly put admin tasks on the back burner until something is on fire and must be put out. For example, until they tell me, "You can't do surgery next week because we are out of viscoelastic," it's probably not going to get ordered because it hasn't reached "on fire" status.

With the patient above, a spear master, after surgery.
5. What’s the hardest thing you’ve had to do? Saying "NO" to patients. I can't do everything, so sometimes I have to say, "I can't take care of you." For example, retina cases take a long time, especially when you've been informally trained on the job (huge thanks to Ben Roberts, MD), so I can't do all of them. I have to pick and choose whom I think will benefit the most.
For example, I just had to turn down an 18-year-old boy with a MH and secondary RRD because I just can't take the time to do it. His other eye works well, so it's not urgent enough to warrant our limited resources, namely time. There is only one other place where he can get somewhat affordable retina care in a country of 38 million! They also said "no" and told him to see me. He has no more options.
6. What accomplishment are you most proud of? Professionally, I can't believe what God has given me:
- The privilege to do my first year out of residency in the OR with no one to bail me out;
- VR surgery with ILM peels, ICG, heavy liquid, SF6 and silicone oil;
- Sutured IOLs of every sort;
- Penetrating keratoplasties — the first in western Kenya;
- Exenterations for advanced tumors;
- Optic nerve sheath fenestrations;
- Post-auricular skin grafts on burns, trauma and cutaneous anthrax scars;
- Nearly 100 pediatric cataracts;
- A scleral buckle with prp/Avastin on a 1,600 gram (3.5 pound) baby with stage IVa ROP OU;
- MSICS — the most important and beautiful surgery in all of ophthalmology and most Western ophthalmologists have yet to hear of it;
- Tubes and trabs and more…
7. What’s the best piece of advice you’ve gotten in your career so far? "If you are working late regularly, you jeopardize everything!" This was my father-in-law's recent admonition to me when he visited Africa and saw the hours I was working. By that he meant, you jeopardizes life's most important relationships with your wife, children, God and self when you don't protect enough time for them.
This is possible even in the pursuit of helping others. I've had to say "no" a lot more at work, which is heartbreaking, but having vibrant relationships with Jessica, Elise, Micah and God are irreplaceable. I also know my patients benefit when I make those relationships a priority. Life is a lot more than just work!
P.S. If anyone wants to hear more stories about our family's experience in Africa, they can check out our blog.
* * *
About Dr. Cropsey: A former Wills Eye Institute resident, Dr. Cropsey is working in Bomet, Kenya, as part of a post-residency program with Samaritan’s Purse. He completed medical school at the University of Michigan, Ann Arbor, and an internship at the Albert Einstein Medical Center in Philadelphia before his residency at Wills.