EPIDEMIOLOGY
Global Information
- Polypoidal choroidal vasculopathy (PCV) primarily affects pigmented individuals, especially Asians and African-Americans
- Typically presents in 7th to 8th decade of life, though may present earlier than other forms of macular degeneration
- Caucasians are affected to a lesser extent and with different clinical features
- Table 1 highlights the observed differences in PCV characteristics across ethnicities.
Table 1: Polypoidal Choroidal Vasculopathy Demographics and Characteristics |
|
Ethnicity
|
Mean Age
|
% Male
|
% Bilateral
|
% Central Macula Involving
|
|
White
|
60-70
|
<50
|
20-80
|
25-68
|
|
Japanese
|
60-70
|
>60
|
<10
|
>85
|
Regional Information (Asia)
- Japan
- 23-55% of those with age-related macular degeneration (AMD) have signs of PCV
- 92% of patients with PCV have central macula involving lesions
- 71% male
- 14% bilateral
- Singapore
- 33-61.1% of those with AMD have PCV
- 58.1-62.4% male
- Up to 87.8% unilateral
- South Korea
- 24.6% of those with AMD have PCV
- 78.5% male
- 75.9% unilateral
- China and Taiwan
- 24.5-49% of those with AMD have PCV
- 71.4% male
- 91.8% unilateral
DIFFERENTIAL DIAGNOSIS
- AMD
- Choroidal neovascularization (CNV)
- Central serous chorioretinopathy (CSC)
- Pathologic myopia
- Melanocytoma
- Choroidal Tumors (hemangioma, melanoma, etc)
- Tilted disc syndrome
- Choroidal osteoma
PATHOPHYSIOLOGY/DEFINITION
PCV is a neovascular and hemorrhagic disorder of the choroid.
- Degeneration of the walls of arterioles, capillaries, and venules
- Large vascular channels and “polypoid” formations
- Thickened capillary basement membranes
- Hyalinization of choroidal vessels
- Exudation of fibrin and plasma
Genetic Factors
- Gene HTRA1 is associated with PCV as well as neovascular AMD
- Complement factor H (CFH) variants rs3753394 and rs 800292 are associated with PCV
- CRP levels are higher in PCV patients and in AMD patients than in control patients
- I62V variant of CFH is associated with PCV in Japanese patients
- ARMS2 gene for mitochondrial photoreceptor protein is associated with PCV in Japanese patients
Vascular endothelial growth factor (VEGF) plays an uncertain role in the pathophysiology of PCV.
- VEGF has been localized to the retinal pigment epithelium (RPE) in patients with PCV
- VEGF has not been seen in the vascular endothelium on immunostaining of surgical specimens
- Anti-VEGF treatment has been well-reported to be effective in treating fluid associated with PCV; however, it has shown inconsistent results in resolving the polypoid vascular lesions
Clinical Course
1. Can be variable in severity, ranging from spontaneous resolution to recurrent subretinal bleeding and subretinal pigment epithelial bleeding
2. Recurrent serosanguinous detachments of the RPE or neurosensory retina
3. Microtears of RPE
4. RPE atrophy
5. Vision loss in ~ 50% of patients
SIGNS/SYMPTOMS
Clinical Characteristics
- Serosanguinous detachments of the RPE and neurosensory retina
- PCV lesions and choroidal neovascularization (CNV)
- Typically peripapillary or central macula location
- Relatively preserved retinal architecture
- Better-than-expected visual acuity
- Pigment epithelial detachment associated with polypoid lesions
- Chronic lipid deposition
- Occasional spontaneous resolution with residual pigment mottling
Clinical characteristics may differ in Caucasian patients;
- Lesions are primarily peripapillary
Imaging
Fluorescein Angiogram (FA)
- Branching choroidal vessels
- Polypoidal lesions can at times be difficult to see on FA. Lesions may manifest as either classic or occult leakage patterns
- Atrophy of RPE
Indocyanine Green Angiography (ICG)
- Choroidal vessel hyperpermeability
- Pulsatile polypoidal vessels
- Choroidal vascular networks
Optical Coherence Tomography (OCT)
- Sub-RPE polypoidal lesions
- Pigment epithelial detachments
MANAGEMENT
- Photocoagulation
- Effective for treating extrafoveal polyps, but success rate is variable
- Persistent exudation from branching vascular network reported in 28.5%- 37.7%
- Yuzawa reported that only 10% of eyes worsened if both the polyp and network were lasered, compared to 54% of eyes worsened after laser to polyps only. However, lasering the whole network is often impossible due to the large area involved
- Combined with anti-VEGF, photocoagulation has been shown to confer additional benefit in reducing exudation and hemorrhage from the network, while focal laser can be targeted mainly to the polyps.
- Treatment of the entire lesion is effective in resolving exudative lesions and preventing further vision loss
- Treatment of only the polypoid lesion does not prevent recurrence or progression
- Laser photocoagulation is reserved for extrafoveal polyps. Treating the entire lesion including the branching vascular network may not always be possible.
- Anti-VEGF
- The pathophysiology of polypoidal lesions may not be a VEGF-driven process
- Intravitreal bevacizimab has been shown to be effective treatment for fluid associated with PCV, but has not been shown to improve polypoidal lesions
- Intravitreal ranibizumab resulted in regression of polypoidal lesions in 70% of patients in a small study
- Photodynamic Therapy (PDT)
- PDT has been shown to be effective in preserving or improving visual acuity
- PDT may be more effective for PCV than for wet AMD
- Complications of PDT include subretinal hemorrhage and vitreous hemorrhage
- The optimal therapy for PCV is still unclear. Currently there are two clinical trials comparing anti-VEGF alone with combination therapy (anti-VEGF and PDT).
- Anti-VEGF vs PDT:
- Many studies reporting up to 12-month follow-up have described stabilization of vision and improvement of exudation
- Inoue et al reported better vision at month 18 and 24 in eyes treated with intravitreal ranibizumab compared to those treated with PDT
- LAPTOP study based in Japan (Phase IV, prospective RCT) reported better visual outcomes in eyes treated with ranibizumab than eyes treated with PDT at month 12 and month 24
- Concern remains related to incomplete polyp regression, which has been thought to lead to recurrence
- Higher recurrence rate has been reported in anti-VEGF treated eyes (64.9%) compared to PDT treated eyes (47.4%) at 2 years in a study based in Korea
- EVEREST study: A multicenter RCT reported higher polyp closure rate in eyes treated with PDT (77.8% combined with ranibizumab and 71.4% PDT alone) compared to eyes treated with ranibizumab alone (28.6%). However visual acuity gain in the ranibizumab group was numerically higher than PDT monotherapy group (9.2 letters vs 7.5 letters, not statistically significant)
- Some centers (particularly in Japan) recommend reserving PDT to eyes with poor vision to minimize the risk of visual deterioration that may be seen in PDT
Treatment Algorithm
- Workup: Clinical History, Dilated Fundus Exam (FA/ICG)
- If Visual Acuity is 20/30 or Better: Observation, though treatment initially with Anti-VEGF may be considered in patients with good visual acuity but significant exudate
- If Visual Acuity is 20/40 or Worse: Consider treatment for symptomatic patients
- PDT is often effective initial treatment for PCV where available
- If the polypoidal lesion is associated with significant exudate or fluid, consider PDT + anti-VEGF therapy
- Recurrent associated fluid that is visually significant and responsive to anti-VEGF intravitreal injection may require repeat anti-VEGF injections to maintain stable vision
- If lesions are not responsive to repeat injections of an initial anti-VEGF agent, a switch to a different agent may be effective (eg,, switching from ranibizumab to aflibercept)
- If PDT is not an available treatment option, laser photocoagulation of polypoidal lesions outside of the foveal avascular zone may be an effective treatment strategy;however, laser photocoagulation has been associated with macular hemorrhage and should be performed only if the entire lesion can be treated
CASE STUDY: Japan/Asia
History of Present Illness
- A 69-year-old Japanese male patient with no past medical history or ocular history presented to a clinic complaining of decreased visual acuity of the right eye for 2 months
Examination
- Visual acuity: 20/100 right eye; 20/30 left eye
- Intraocular pressure (IOP): 15 mm/Hg both eyes
Slit-lamp examination
- Lens: mild nuclear sclerotic cataract of both eyes
Fundus examination
- Macula: Drusen. Parafoveal polypoidal vascular lesions beneath the RPE in the right eye
Testing
- FA and ICG showed polypoidal choroidal neovascularization in the right eye
- Macular OCT showed serous pigment epithelial detachments and subretinal pigment epithelium polypoidal lesion of the right eye
Treatment
- PDT
- Anti-VEGF therapy: The patient was treated with ranibizumab monthly injections for 3 months, followed by prn injections for a total of 4 injections in 6 months
Follow-up
- After 6 months, visual acuity was 20/40 in the right eye. The polypoidal neovascular lesions showed signs of regression on FA and ICG. The serous exudative detachment was significantly improved.
CASE IMAGES (Asia)
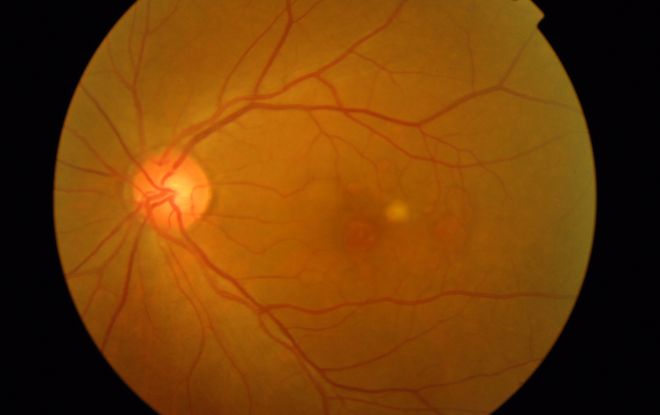 Figure 4a
Figure 4a
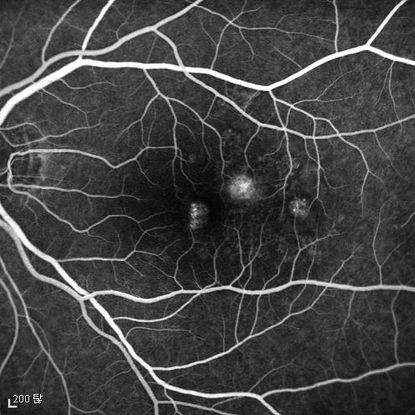
Figure 4b
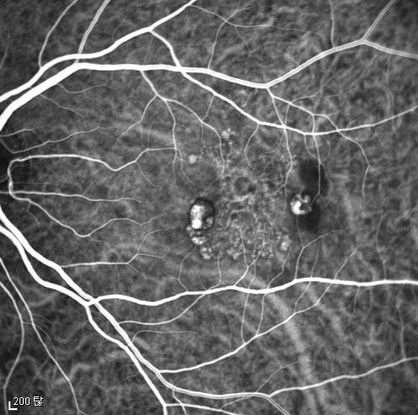 Figure 4c
Figure 4c
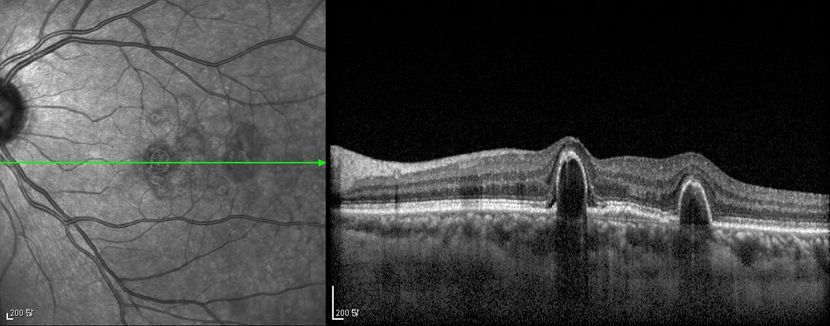
Figure 4d
Figures 4a-4d. Case Images Asia. A 58- year-old woman with reduced visual acuity for 1 month. BCVA: 20/40. Orange round lesions at the fovea in color photograph (A) represents polyps that are revealed in fluorescein angiography (B) and in indocyanine green angiography (C). Branching vascular networks are obvious in ICG. Section through the polyps in OCT (D) reveals local pigment epithelial detachments (Case and images courtesy of Young Hee Yoon MD, Asan Medical Center, Ulsan University, Seoul, Korea.)
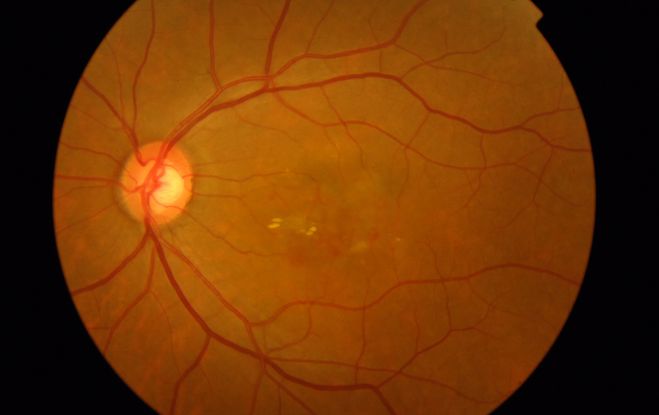 Figure 5a
Figure 5a
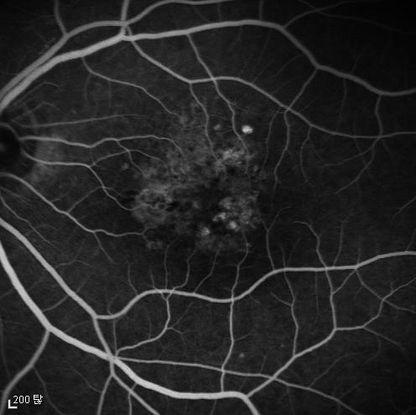 Figure 5b
Figure 5b
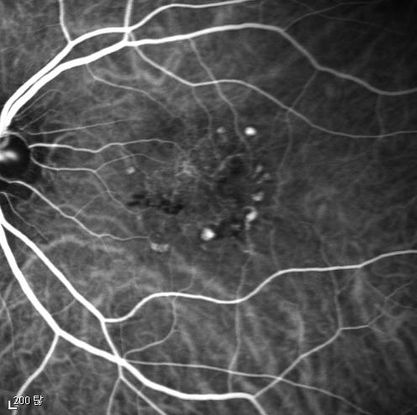
Figure 5c
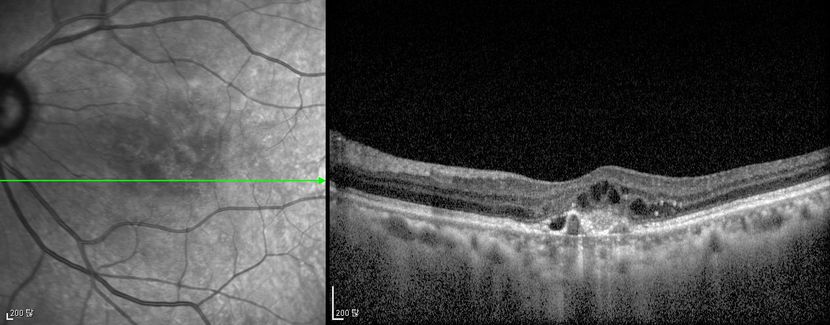
Figure 5d Figures 5a-5d. Case Images Asia. A 60- year-old woman with reduced visual acuity for 2 weeks. BCVA: 20/80. Retinal hemorrhage with exudate at the fovea in color photograph (A) represents polyps that are revealed in fluorescein angiography (B) and in indocyanine green angiography (C). Branching vascular networks are obvious in ICG. Section through the polyps in OCT (D) reveals local pigment epithelial detachments and fluid collection at subretinal and intraretinal space (Case and images courtesy of Young Hee Yoon MD, Asan Medical Center, Ulsan University, Seoul, Korea.)
REFERENCES
Ahuja RM, Stanga PE, Vingerling JR, et al. Polypoidal choroidal vasculopathy in exudative and haemorrhagic pigment epithelium detachments. Br J Ophthalmol. 2000; 84(5): 479-484.
Cho M, Barbazetto IA, Freund KB. Refractory neovascular age-related macular degeneration secondary to polypoidal choroidal vasculopathy. Am J Ophthalmol. 2009; 148 (1): 70-78.
Gemmy Cheung CM, Yeo I, Li X et al. Argon laser with and without anti-vascular endothelial growth factor therapy for extrafoveal polypoidal choroidal vasculopathy. Am J Ophthalmol . 2013; 155: 295-304 e291.
Gomi F, Sawa M, Sakaguchi H, et al. Efficacy of intravitreal bevacizumab for choroidal vasculopathy. Br J Ophthalmol. 2008; 92(1): 70-73.
Imamura, et al. Polypoidal Choroidal Vasculopathy: A Review. Surv Ophthalmol. 2010: 55(6).
Inoue M, Arakawa A, Yamane S, Kadonosono K. Short-term efficacy of intravitreal aflibercept in treatment naïve patients with polypoidal choroidal vasculopathy. Retina. Accessed July 18, 2014, Epub ahead of print.
Jeon S, Lee WK and Kim KS. Adjusted retreatment of polypoidal choroidal vasculopathy after combination therapy: results at 3 years. Retina. 2013; 33: 1193-1200.
Kondo N, Honda S, Ishibashi K, et al. LOC387715/HTRA1 variants in polypoidal choroidal vasculopathy and age-related macular degeneration in a Japanese population. Am J Ophthalmol. 2007; 144(4): 608-612.
Kwok AK, Lai TY, Chan CW, et al. Polypoidal choroidal vasculopathy in Chinese patients. Br J Ophthalmol. 2002; 86(6): 892-897.
Lafaut BA, Leys AM, Snyers R, et al. Polypoidal choroidal vasculopathy in Caucasians. Graefes Arch Clin Exp Ophthalmol. 2000; 238(9): 751-759.
Lee KY, Vithana EN, Mathur R, et al. Association analysis of CFH, C2, BF, and HTRA1 gene polymorphisms in Chinese patients with polypoidal choroidal vasculopathy. Invest Ophthalmol Vis Sci. 2008; 49(6): 2613-2619.
Lee MW, Yeo I, Wong D, Ang CL. Argon laser photocoagulation for the treatment of polypoidal choroidal vasculopathy. Eye. 2009; 23(1):145-148.
Maruko I, Iida T, Saito M, et al. Clinical characteristics of exudative age-related macular degeneration in Japanese patients. Am J Ophthalmol. 2007; 144(1): 15-22.
Nakashizuka H, Mitsumata M, Okisaka S, et al. Clinico-pathological findings of polypoidal choroidal vasculopathy. Invest Ophthalmol Vis Sci. 2008; 49(11): 4729-4737.
Okubo A, Sameshima M, Uemura A, et al. Clinicopathological correlation of polypoidal choroidal vasculopathy revealed by ultrastructural study. Br J Ophthalmol. 2002; 86(10): 1093-1098.
Pantaleoni FB, Galante VM, Da Dalt S, Pecorella I. Localizing polypoidal choroidal vasculopathy for laser treatment. Acta Ophthalmol Scand. 2007; 85(4): 456-458.
Reche-Frutos J, Calvo-Gonzales C, Donate-Lopez J, et al. Short-term anatomic effect of ranibizumab for polypoidal choroidal vasculopathy. Eur J Ophthalmol. 2008; 18(4): 645-648.
Saito M, Kano M, Itagaki K, Oguchi Y, Sekiryu T. Switching to intravitreal aflibercept injection for polypoidal choroidal vasculopathy refractory to ranibizumab. Retina. Accessed July 30, 2014, Epub ahead of print.
Sho K, Takahashi K, Yamada H, et al. Polypoidal choroidal vasculopathy: incidence, demographic features, and clinical characteristics. Arch Ophthalmol. 2003; 121: 1392-1396.
Spaide RF, Yannuzzi LA, Slakter JS, et al. Indocyanine green videoangiography of idiopathic polypoidal choroidal vasculopathy. Retina. 1995; 15: 100-110.
Terasaki H, Miyake Y, Suzuki T, et al. Polypoidal choroidal vasculopathy treated with macular translocation: clinical pathological correlation. Br J Ophthalmol. 2002; 86(3): 321-327.
Tsujikawa A, Sasahara M, Otani A, et al. Pigment epithelial detachment in polypoidal choroidal vasculopathy. Am J Ophthalmol. 2007; 143(1): 102-111.
Yuzawa M, Mori R, Haruyama M. A study of laser photocoagulation for polypoidal choroidal vasculopathy. Jpn J Ophthalmol. 2003; 47(4): 379-384.
Additional References (Asia)
Byeon SH LS, Oh HS, Kim SS et al. Incidence and clinical patterns of polypoidal choroidal vasculopathy in Korean patients. Jpn J Ophthalmol. 2008; 52: 57-62.
Cackett P WD, Yeo I. A classification system for polypoidal choroidal vasculopathy. Retina. 2009; 29: 187-191.
Cheung CMG, Li X, Mathur R, et al. A prospective study of treatment patterns and 1-year outcome of Asian Age-related macular degeneration and polypoidal choroidal vasculopathy. Plos One. 2014 Jun 30; 9(6): e101057.
Inoue M, Arakawa A, Yamane S and Kadonosono K. Long-term outcome of intravitreal ranibizumab treatment, compared with photodynamic therapy, in patients with polypoidal choroidal vasculopathy. Eye. 2013; 27:1013-1020; quiz 1021.
Kang HM and Koh HJ. Two-year outcome after combination therapy for polypoidal choroidal vasculopathy: comparison with photodynamic monotherapy and anti-vascular endothelial growth factor monotherapy. Ophthalmologica Journal international d'ophtalmologie International journal of ophthalmology Zeitschrift fur Augenheilkunde. 2014; 231: 86-93.
Koh A, Lee WK, Chen LJ et al. EVEREST study: efficacy and safety of verteporfin photodynamic therapy in combination with ranibizumab or alone versus ranibizumab monotherapy in patients with symptomatic macular polypoidal choroidal vasculopathy. Retina. 2012; 32:1453-1464.
Lai TY, Lee GK, Luk FO and Lam DS. Intravitreal ranibizumab with or without photodynamic therapy for the treatment of symptomatic polypoidal choroidal vasculopathy. Retina. 2011; 31:1581-1588.
Laude A, Cackett PD, Vithana EN, Yeo IY, et al. Polypoidal choroidal vasculopathy and neovascular age-related macular degeneration: Same or different disease? Prog Ret Eye Res. 2009; 29: 19-29.
Liu Y WF, Huang S, Luo G, et al. Subtype lesions of neovascular age-related macular degeneration in Chinese patients. Graefes Arch Clin Exp Ophthalmol. 2007; 245: 1441-1445.
Oishi A, Miyamoto N, Mandai M et al. LAPTOP study: a 24-month trial of verteporfin versus ranibizumab for polypoidal choroidal vasculopathy. Ophthalmology. 2014; 121: 1151-1152.
Wen F, Chen C, Wu D, Li H. Polypoidal choroidal vasculopathy in elderly Chinese patients. Graefes Arch Clin Exp Ophthalmol. 2004; 242(8): 625-629.
CONTRIBUTORS
Executive Editor:
R. V. Paul Chan, MD, FACS, Weill Cornell Medical College, New York, New York
Section Editor:
Asia-Pacific:
Timothy Y. Lai, MBBS, MD, MMedSc, FRCS, FRCOphth, FHKAM, Department of Ophthalmology & Visual Sciences, The Chinese University of Hong Kong
Associate Editors:
Jeff Pettey, MD, University of Utah Department of Ophthalmology and Visual Sciences, John Moran Eye Center's Residency Program Director
Grace Sun, MD, Weill Cornell Eye - Lower Manhattan, Weill Cornell Medical College Residency Program Director
Assistant Editors:
Samir Patel, BS, Weill Cornell Medical College, New York, New York
Peter Coombs, MD, Weill Cornell Medical College; New York, New York
Regional Contributors:
Asia Pacific:
Dr. Gemmy Cheung, Consultant Ophthalmologist, Singapore National Eye Centre
Dr. Andrew Fok, Hong Kong Eye Hospital, Hong Kong
Dr. Lim Tock Han, NHG Eye Institute, Tan Tock Seng Hospital, Singapore
American Academy of Ophthalmology
P.O. Box 7424
San Francisco, CA 94120-7424
415.561.8500
Copyright © 2014 American Academy of Ophthalmology®. All Rights Reserved.