Parental Education
Amblyopia is decreased vision due to abnormal visual development in infancy or childhood.1 This can be caused by strabismus, anisometropia, or visual deprivation and can be unilateral or bilateral. Amblyopia can be very effectively treated by patching or otherwise penalizing the dominant eye. In this text, the challenges associated with patching treatment for unilateral amblyopia will be discussed.
Patching is often a difficult task for many parents to accomplish. The first step toward successful parental compliance is ensuring that parents understand why it is important. Amblyopia is not something that parents can visualize easily – especially when there is no outwardly visible sign. It is also easy for parents to misunderstand the goals of patching, especially in cases where there is concurrent strabismus (they often mistakenly expect improvement in eye alignment when they are in fact only patching for gains in visual acuity). When explaining amblyopia, it is helpful to use simple language to convey a complex concept:
“When a child receives different images from each eye, due to unequal focus or eye misalignment, the child's brain is able to avoid double vision or confusion about which image is correct by simply suppressing, or ignoring, the image coming from one eye. Rather than see 2 images in the case of eye misalignment, or try to combine one clear image with one blurry image in the case of unequal focus, the brain can turn off one eye. The consequence is that as vision develops normally in the preferred eye, the eye being ignored or suppressed stops developing and, in many cases, even loses vision. If not treated, this can lead to very poor vision or even blindness.”
Emphasizing the importance of early treatment can also be helpful to illustrate why it is important that the parents comply with the child's treatment immediately rather than wait until the child is older and easier to reason with.2
“We have a limited window to treat amblyopia – when your child reaches 'visual maturity' around age 10 or so, his brain will no longer be able to make the changes it needs to make to see better, and patching stops working very well or at all. The younger a child is when we start patching, the more likely it is that there will be a good outcome.”
Compliance and Patching Dose
The mainstay of treating amblyopia is patching of the dominant eye during waking hours. The prescribed number of hours of patching will depend on the visual acuity in the amblyopic eye and whether treatment has been successful in the past. Both full-time occlusion (FTO) and part-time occlusion (PTO) have been proven successful, and the discussion of how much patching must be done should include parental input.3-5
The Pediatric Eye Disease Investigator Group (PEDIG) has completed several multicenter, randomized clinical trials comparing the efficacy of different patching regimens and alternative treatments.
The Amblyopia Treatment Study 2 (ATS 2) compared the effects of differing numbers of prescribed patching hours on amblyopia in children aged 3 to 7 years. One arm of the study compared patching 6 hours daily to patching FTO for severe amblyopia (20/100 to 20/400). The average improvement in visual acuity after 4 months of treatment was 4.8 lines in the PTO group and 4.7 lines in the FTO group. They found no difference between the two groups in visual outcome or rate of improvement.4
Another arm of ATS 2 compared patching 2 hours daily to patching 6 hours daily for moderate amblyopia (20/40 to 20/80). After 4 months of treatment, there was no statistically significant difference in acuity between the two groups. Sixty-two percent of patients achieved 20/30 acuity or at least 3 lines of improvement from baseline with either of the patching regimens after 6 months of treatment. Initially, there had been a faster rate of improvement in the group that patched 6 hours daily.3
ATS 3 looked at the effect of amblyopia treatment in older age groups (7 to 17 years) and found that patching could improve visual acuity when amblyopia had not previously been treated, but was of little benefit if amblyopia was previously treated.6
The PEDIG studies have a few limitations, including self-reported compliance, short follow-up times, lack of discussion regarding rate of improvement in vision, and a subnormal 20/30 acuity outcome measure. Differences of opinion still exist among pediatric ophthalmologists regarding the roles of part-time occlusion versus full-time occlusion therapy in the management of amblyopia. The advantages of FTO, defined as all waking hours, include shorter duration of patching (in terms of months undergoing therapy) and a clear endpoint (3 episodes of no improvement). Because FTO is the maximum possible dose, there is no need to increase patching hours if vision stops improving.7
The risk of occlusion amblyopia, or the development of amblyopia in the previously preferred/patched eye, is higher in patients undergoing FTO. Therefore, this patching regimen requires more rigid follow-up of about 1 week per year of age in children younger than 4 years.8 Children older than 4 years should have their vision checked every 4 weeks. Evidence suggests that although the incidence of occlusion amblyopia in patients treated with FTO is higher, it is almost always reversible, and patients still have a good outcome.8
Others object to FTO because patching in school can potentially lead to teasing or bullying from peers. However, practitioners who use FTO often note that this is not a commonly cited parental concern, and that many parents find that compliance is easier at school, where it can be monitored by a teacher.7,8 If intolerable social pressures are present, alternative arrangements (ie, PTO) may be preferable.
Supporters of PTO believe that less patching time achieves the same results as FTO (albeit over a longer course of time).5,9 Other advantages of PTO include less-frequent follow-up (patients are seen every 2 months or so, depending on age) and less pressure to patch in the presence of peers.10
For some children, consistency is a strong advantage to FTO. Anecdotally, compliance issues seem more common in patients treated with PTO than FTO. For example, if an occlusion regimen of four hours per day is prescribed, the patient or the parents will often attempt to “bargain” this amount down to a lower number. A child may act out when it is time to put the patch on and continue his objections until the patch is removed. By contrast, if everyone understands that the patch is to be on at all times, bargaining about duration is no longer an issue, and the child may be less likely to misbehave, as the patch is now non-negotiable.
An appropriate discussion with parents upon initiation of patching therapy for amblyopia includes mention of both PTO and FTO. The provider may mention that different providers have different interpretations of the scientific data regarding how many hours per day the patch should be worn. The provider may mention that some feel that PTO and FTO are equally effective, but that FTO may yield quicker results, and that sometimes FTO may be easier to perform than PTO.
Types of Eye Patches
There are several different types of patches available including skin patches, felt patches, and pirate patches. The skin patch fits under the glasses and adheres to the skin, which makes it more difficult to remove and does not allow the child to peek easily. This method is preferred for all patients who can tolerate it, particularly very young patients and patients with amblyopia in the 20/100 or worse range.

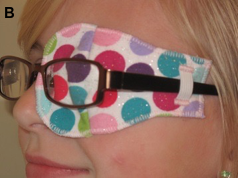

Figure 1. A. An adhesive (skin) patch (example from www.ortopadusa.com). B. A patch designed for use underneath glasses (example from www.eye-lids4kids.com). C. Pirate patches (example from www.etsy.com).
A common problem that comes up with the use of adhesive eye patches is skin irritation or chafing. Removing the patch with the help of a warm compress or in the bath can lessen the sting when it is pulled off. Petroleum jelly or skin lotion on the patched area overnight can help keep chafing to a minimum. Some children have a skin reaction to certain types of adhesive and may benefit from a brand of patch that is hypoallergenic.
Milk of magnesia can be used to protect the skin. Apply liquid milk of magnesia with a cotton ball to the area of the face where the patch sticks, being careful to avoid getting it in the eye. Allow it to dry, and then apply the eye patch. This creates a barrier between the skin and the adhesive, and is effective at reducing or preventing skin irritation.
There are different types of cloth or felt patches available for those patients who are unable to tolerate adhesive patches. Some go under the glasses against the eye, others go over the glasses. Pirate patches do not work well in combination with glasses.
Whatever style of non-sticky patch the family chooses should make contact with the skin all the way around, and parents should be certain that their child is not sneaking peeks around the edges. These types of patches work best with slightly older children whose vision is in the moderate range.
One single type of eye patch cannot fit all patients. It is important to find an option that will produce the best possible compliance in the individual using the patch.
Gaining Patient Compliance
Many children will resist wearing a patch at first. Successful patching may require persistence and plenty of encouragement from family members, neighbors, teachers, and others. Children will often be upset by the patch at first, but they will eventually learn not to remove it. It can help to engage them in an enjoyable and distracting activity immediately after placing the patch. This can help occupy them while they get used to having the patch on. It is essential that parents understand that they must both be persistent and consistent in enforcing the wearing of the patch, so that the child understands that this is an expected and non-negotiable process.
It is often helpful to provide a reward to the child for keeping the patch on for the prescribed time period. It can be helpful to create a patching calendar. For example: the child may earn a sticker for each day that they patch well without objection or without early removal. At the end of the week, if they have earned all of their stickers, they are rewarded.
In many instances, school is an excellent time to patch, taking advantage of a nonparental authority figure. Patching during school hours gives the class an opportunity to learn valuable lessons about accepting differences between children. While in most instances children may not need to modify their school activities while patching, sometimes adjustments such as sitting in the front row of the classroom will be necessary. If the patient, teacher, and classmates are educated appropriately, school patching need not be a socially stigmatizing experience. On the other hand, frequently a parental or other family figure may be more vigilant in monitoring patching than is possible in a school setting. Parents should be flexible in choosing when to schedule patching.
Some children may like to have a stuffed toy or doll who also has to patch just like they do. They may like to decorate their own patch with markers or stickers before putting it on.

Figure 2. A child whose doll wears a patch similar to her own (example from www.ortopadusa.com).
Addressing Non-Compliance
In young children, the use of arm guards (“no-no’s”), which are gentle restraints, may help during the difficult phases of patching therapy. When worn, these restraints keep most children from removing the patch by preventing them from bending their elbows. It is often not necessary for them to wear the restraints for all of the prescribed patching time; they can be used very effectively as a form of negative reinforcement. In a typical scenario, the parent puts the patch on the child, who immediately rips it off. The no-no’s are put on, as well as a new patch. After several minutes, the no-no’s are removed. However as soon as the child removes the patch the no-no’s must be replaced. Eventually most children learn that if they leave the patch on, they will not have to wear the no-no’s.
For older children, it is often helpful to restrict enjoyable activities unless the patch is on. This is particularly useful in patients participating in part-time occlusion. For example, patients who really like playing video games should only be allowed to play while they have a patch on.11
Alternatives to Patching
Sometimes the stronger (good) eye can be “penalized,” or blurred with atropine eye drops, lenses, Bangerter occlusion foils, or tape, to force the child to use and strengthen the weaker eye.9,12 Contact lenses can also be used as occlusive devices, either by over-plussing or over-minusing the lens, or by using a blacked-out occluder contact lens. Ophthalmologists often choose atropine drops or another patch alternative when the vision is better than 20/100 in the amblyopic eye or when a child is unable to wear the patch as recommended.
The first PEDIG Amblyopia Treatment Study (ATS 1) compared the use of daily atropine to patching for a range of 6 hours to FTO (at the investigator’s discretion) in patients aged 3 to 7 years with moderate amblyopia (20/40 to 20/100). There was improvement in both groups. Improvement was more rapid in the patching group, but no difference in visual outcome after 2 years was found between the two groups.13 Follow-up studies have found that after 15 years, the improvement in the amblyopic eye was maintained, and that the outcome was similar regardless of initial treatment with atropine or patching.14
ATS 4 compared daily atropine to weekend use. Weekend atropine use provides improvement in visual acuity similar to that by daily atropine use in moderate amblyopia.15
Stopping Treatment
In some cases, treatment for amblyopia may not succeed in substantially improving vision. Every effort should be made to improve the vision prior to stopping treatment. Refraction and alignment should be re-evaluated to ensure proper focus and excellent alignment. Switching the method of occlusion (from patch to atropine, or from atropine to occlusion foil, for instance) should be tried. It is hard to decide to stop treatment short of 20/20, but sometimes it is best for both the children and their families. Children who have amblyopia in one eye and good vision only in their other eye can wear safety glasses and sports goggles to protect the normal eye from injury. As long as the good eye stays healthy, these children function normally in most aspects of life.1
On the other hand, stopping the treatment after a successful result from patching therapy is an easier decision. Rather than stopping the treatment cold, one should consider “weaning off” the regimen. Recurrence was 4 times as likely in children who did not have a gradual taper of their treatment (ie, reducing patching from 6 hours daily to 2 hours daily before discontinuation resulted in better outcomes than immediate cessation).16 Other factors linked to greater likelihood of recurrence included better visual acuity at the end of treatment, a greater number of lines of improvement in visual acuity during treatment, and previous history of recurrence.16-18
Follow-Up Schedule
Full-time patching (full-time occlusion [FTO]) is defined as all waking hours. One episode of patching is one week per year of age, not to exceed four weeks without having a follow-up vision check to ensure that there is no reversal (occlusion amblyopia). For example, a 2-year-old patient undergoing full-time occlusion must have a vision check again after 2 weeks. A 5-year-old undergoing FTO must have a vision check after 4 weeks.
Part-time patching, defined as any amount less than all waking hours, allows for longer episodes of therapy. A good way to manage follow-up for patients who are part-time patching is to double the number of weeks or months that would be prescribed if they were full-time patching. For example, a 2-year-old patient patching 4 hours per day should be seen in 4 weeks (rather than the 2 weeks required if doing FTO). A 5-year-old patient patching 4 hours per day should be seen in 2 months rather than 1 month.
Conclusion
The assistance and expertise of an orthoptist, an allied health professional trained specifically in the medical management of amblyopia and strabismus, can be invaluable in a busy pediatric ophthalmology clinic. In addition to providing expertise and advice on appropriate patch titration, orthoptists are able to see patients independently. Orthoptists can see amblyopic patients for a vision check and manage patching changes on their own, freeing the ophthalmologist’s schedule for other types of patients.
Patching is not always an easy task. Working with parents to increase their understanding of amblyopia and visual development and encouraging the use of positive reinforcement can greatly improve compliance and ultimately result in better visual outcomes.
References
- American Association for Pediatric Ophthalmology and Strabismus. Amblyopia. http://www.aapos.org/terms/conditions/21. Updated May 2015. Accessed February 4, 2016.
- Holmes JM, Lazar EL, Melia BM, et al. Effect of age on response to amblyopia treatment in children. Arch Ophthalmol (Chicago, Ill : 1960). 2011;.129:1451-1457.
- Repka MX, Beck RW, Holmes JM, et al. A randomized trial of patching regimens for treatment of moderate amblyopia in children. Arch Ophthalmol (Chicago, Ill : 1960). 2003; 121:603-611.
- Holmes JM, Kraker RT, Beck RW, et al. A randomized trial of prescribed patching regimens for treatment of severe amblyopia in children. Ophthalmology. 2003; 110:2075-2087.
- Wallace DK, Edwards AR, Cotter SA, et al; Pediatric Eye Disease Investigator Group. A randomized trial to evaluate 2 hours of daily patching for strabismic and anisometropic amblyopia in children. Ophthalmology. 2006; 113:904-912.
- Scheiman MM, Hertle RW, Beck RW, et al; Pediatric Eye Disease Investigator Group. Randomized trial of treatment of amblyopia in children aged 7 to 17 years. Arch Ophthalmol (Chicago, Ill : 1960). 2005; 123:437-447.
- Scott WE, Kutschke PJ, Keech RV, Pfeifer WL, Nichols B, Zhang L. Amblyopia treatment outcomes. J AAPOS. 2005; 9:107-111.
- Longmuir S, Pfeifer W, Scott W, Olson R. Effect of occlusion amblyopia after prescribed full-time occlusion on long-term visual acuity outcomes. J Pediatric Ophthal Strabismus. 2013; 50:94-101.
- Scheiman MM, Hertle RW, Kraker RT, et al. Patching vs atropine to treat amblyopia in children aged 7 to 12 years: a randomized trial. Arch Ophthalmol (Chicago, Ill : 1960). 2008; 126:1634-1642.
- Golden RP, Olitsky SE. The effect of media press coverage on parental preferences in amblyopia treatment. J AAPOS. 2005; 9:212-215.
- Weed MC, Larson SA. Management of Amblyopia: Discussing Options for Treatment in the Age of the Internet. http://webeye.ophth.uiowa.edu/eyeforum/cases/178-Amblyopia-Management.htm. September 2013. Accessed February 4, 2016.
- Rutstein RP, Quinn GE, Lazar EL, et al; Pediatric Eye Disease Investigator Group Writing Committee. A randomized trial comparing Bangerter filters and patching for the treatment of moderate amblyopia in children. Ophthalmology. 2010; 117:998-1004.e6.
- Pediatric Eye Disease Investigator Group. A randomized trial of atropine vs. patching for treatment of moderate amblyopia in children. Arch Ophthalmol (Chicago, Ill : 1960). 2002; 120:268-278.
- Repka MX, Kraker RT, Holmes JM, et al. Atropine vs patching for treatment of moderate amblyopia: Follow-up at 15 years of age of a randomized clinical trial. JAMA Ophthalmology. 2014; 132:799-805.
- Repka MX, Cotter SA, Beck RW, et al. A randomized trial of atropine regimens for treatment of moderate amblyopia in children. Ophthalmology. 2004; 111:2076-2085.
- Holmes JM, Beck RW, Kraker RT, et al, Pediatric Eye Disease Investigator Group. Risk of amblyopia recurrence after cessation of treatment. J AAPOS. 2004; 8(5):420–428. pmid:15492733.
- Holmes JM, Melia M, Bradfield YS, Cruz OA, Forbes B. Pediatric Eye Disease Investigator Group. Factors associated with recurrence of amblyopia on cessation of patching. Ophthalmology. 2007; 114(8):1427–1432. pmid:17363058.
- Hertle RW, Scheiman MM, Beck RW, et al, Pediatric Eye Disease Investigator Group. Stability of visual acuity improvement following discontinuation of amblyopia treatment in children aged 7 to 12 years. Arch Ophthalmol. 2007;125(5):655–659pmid:17502505.