This chapter was reviewed for currency by Joshua Schliesser, MD on November 13, 2020.
Establishing a diagnosis
Definition
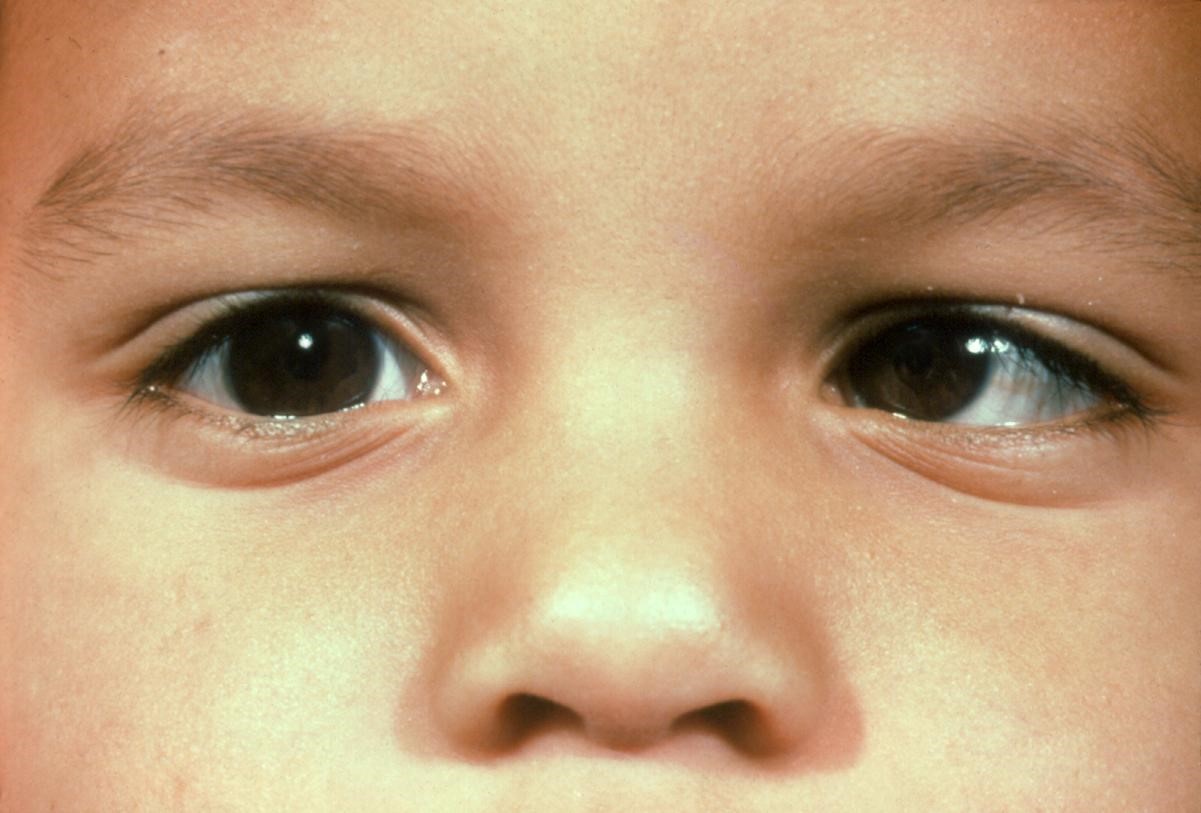
Infantile esotropia is esotropia with an onset before the age of six months, with a constant, large angle of strabismus (> 30 PD), no or mild amblyopia, small to moderate hyperopia, latent nystagmus, dissociated vertical deviation, limitation of abduction (although the patients in fact have normal abduction, they appear to have limitation due to cross fixation), and absent or reduced binocular vision, in the absence of nervous system disorders.1
Epidemiology
The birth prevalence of infantile esotropia has been studied and is reported to range from 1 in 403 live births to as high as 1 in 50 of all newborn children.2,3
History
Except in rare circumstances, large angle, constant esotropia that persists after 2-4 months of age does not resolve spontaneously.1,4 Associated conditions such as dissociated vertical deviation (DVD) and inferior oblique overaction (IOOA) tend to develop most frequently after the age of two years.5
Clinical features
Patients with infantile esotropia are typically neurologically normal, have hyperopia less than 3.50 diopters, and a moderate to large angle esotropia with angle of deviation typically greater than 30 prism diopters. Equal visual acuity is normally observed, with amblyopia occurring in less than half of patients.6 Patients will have full abduction of each eye. DVD and IOOA are frequently observed and reported to occur as high as 57% and 78% of the time, respectively. Nystagmus is also frequently observed and is usually latent type.7 On optokinetic nystagmus (OKN) testing, patients with infantile esotropia will have monocular smooth pursuit asymmetry when the nasal-to-temporal versus temporal-to-nasal OKN response is tested.8
Risk Factors
Genetics
There appears to be a multifactorial genetic basis for congenital esotropia; however, no specific genes have been identified. Parks has noted that primary monofixation syndrome occurs 11 times more frequently among first-degree relatives of patients with infantile esotropia than the general population.9 Prematurity and low birth weight are associated with increased risk of infantile esotropia.10,11
Differential Diagnosis
Accommodative esotropia
Accommodative esotropia or refractive esotropia is often acquired after six months of age, intermittent in nature, and patients typically have hyperopia greater than 3.00 diopters. Treatment is spectacles for the full cycloplegic refraction.
Partially accommodative esotropia is similar to accommodative esotropia; patients will have esotropia in which the angle of deviation is less with full cycloplegic refraction. In these patients, surgery is indicated to correct the remaining deviation.
Cranial nerve VI palsy
Patients with cranial nerve VI palsy will have an abduction deficit and esotropia of the affected eye. Patients with infantile esotropia will often seem to have abduction weakness with voluntary ductions; however, on oculocephalic testing (doll’s-head maneuver) it is possible to help demonstrate near-normal abduction.
Duane Syndrome
Patients with esotropic Duane syndrome have limited abduction with small-angle esotropia in primary gaze, abnormal face turn, and incomitance. They also have palpebral fissure narrowing of the affected eye on adduction.
Restrictive esotropia
Patients with restrictive esotropia will frequently have incomitance and an anomalous head posture. Forced duction testing is helpful in differentiating a restrictive component.
Congenital fibrosis of the extraocular muscles
Patients with congenital fibrosis of the extraocular muscles will frequently have poor ductions. Most frequently this is an upgaze deficit. Ptosis is also frequently observed.
Medial wall fracture
A history of trauma can be useful in differentiating medial wall fracture as a cause of esotropia. Similar to restrictive esotropia, patients will frequently have an anomalous head posture and incomitance. Forced duction testing can be helpful in confirming the diagnosis in this situation.
Sensory esotropia
Sensory esotropia can be seen in patients with poor vision. Infantile esotropic patients will frequently have normal vision in each eye, so any patient with suspected infantile esotropia and poor vision should undergo a complete and thorough eye exam to rule out cause for poor vision.
Nystagmus blockage syndrome
Patients with nystagmus blockage syndrome will have moderate to large amounts of manifest nystagmus and be orthotropic when inattentive, but will have variable esotropia and mild nystagmus when attentive. Observing the patient for pupillary constriction during the esotropic phase may be helpful in making this diagnosis.9
Etiology
The cause of infantile esotropia has been a topic of great debate for the greater part of the last century. Claude Worth believed that infantile esotropia was a congenital defect in fusion faculty, suggesting that despite correction, patients with infantile esotropia could never achieve good binocular vision. Bernard Chavasse later proposed that the brain had the appropriate machinery for fusion but the effect of the eyes’ misalignment impaired the patient’s ability to develop fusion. This led to the idea that early surgery for infantile esotropia could potentially result in good binocular vision. Research done by Eileen Birch and David Stager showed that stereopsis emerges abruptly in the first few months of life but degenerates pathologically within a few months in uncorrected esotropes. Primate studies done by Lawrence Tychsen showed that in monkeys with the constellation deficits that serve as markers of infantile esotropia in humans, there are structural deficits in both superficial and deep layers of the striate cortex.12
Management
Medical therapy options
The treatment of infantile esotropia is extraocular muscle surgery. Botulinum toxin (Botox®) has been suggested as an alternative to surgery in patients with small to medium angle esotropia.13 Botox® may also be used to augment the effects of extraocular muscle surgery.13
Correction of refractive error
Corrective lenses are often prescribed if the hyperopia is greater than 2.50 diopters and/or when there is 1.50 diopters or more of anisometropia.
Amblyopia treatment
Amblyopia treatment is often reserved for those patients with a strong fixation preference.
Surgical therapy options
Frequently, bilateral medial rectus recession is the initial surgery for infantile esotropia. Alternatively, recession and resection of horizontal eye muscles of the same eye may be preferred if there is amblyopia or an anatomic defect of one eye.9
Timing of surgery
The timing of strabismus surgery for infantile esotropia has been greatly debated and studied. Multiple studies have shown that surgery done before two years of age results in better binocular vision and stereopsis.6,12 It has also been suggested that patients operated on within two months of onset of infantile esotropia have the best potential for good stereopsis compared to those operated later.14 In those infants corrected earlier, the incidence of latent nystagmus and dissociated strabismus is less.6,8,14 It is important to communicate to the patient that multiple surgeries may be required to achieve orthotropia.14
Complications of treatment
Undercorrection
Patients with infantile esotropia frequently have large deviations and are more likely to have residual esotropia following maximum bilateral medial rectus recessions. There is some debate about whether three-muscle surgery should be performed at the time of initial operation for large angle esotropia. Most reoperations for infantile esotropia are for undercorrection.
Overcorrection
The incidence of overcorrection is low following surgery for infantile esotropia.17 Early surgical overcorrection should raise concern for a slipped muscle.
Surgical complications
Sight-threatening complications from strabismus surgery are uncommon. Globe perforation is estimated to occur at a rate of 1/1000 cases.15,16 Retinal detachment following globe perforation is rare, with a rate of approximately 1/25,000.15 Cellulitis following strabismus surgery has reported to occur in approximately 1/2000 cases.15,16 Endophthalmitis following strabismus surgery has been reported to occur approximately 1/30,000 cases.15 Anterior segment ischemia occurs at a rate of 1/13,000 cases.18 The incidence of lost rectus muscle has been reported as 1/5000 cases, and the incidence of slipped rectus muscle has been reported as high as 1/1300.17 Complications such as conjunctival cyst, pyogenic granuloma, and corneal dellen have also been reported.
Reoperation rates
Reoperation rates have been reported from 25% to 69%.19
Disease-Related Complications
Amblyopia
A large proportion of patients with infantile esotropia will exhibit cross-fixation, and in these patients, amblyopia, if present, is frequently only mild. Typically, occlusion therapy is reserved for patients with a fixation preference.
Monofixation syndrome
Also known as microtropia, monofixation syndrome is normally seen in patients following strabismus surgery for infantile esotropia. Patients have central suppression with decreased binocular vision. There is presence of binocular peripheral fusion.
Latent nystagmus
Latent nystagmus is frequently seen in patients with infantile esotropia. The nystagmus is conjugate and binocular. Fast phase is directed temporally of the fixating eye and switches with alternation of occlusion. No other forms of nystagmus follow this pattern.9
Dissociated deviations
Dissociated deviations are seen in patients with decreased binocular vision. The nonfixating eye will drift up, drift out, or extort but will recover with binocular refixation. Dissociated vertical deviation (DVD) is most frequently seen; however, dissociated horizontal deviation (DHD) and dissociated torsional deviation (DTD) are also seen. The incidence of dissociated strabismus is reported to occur in 60% to 80% of patients with infantile esotropia.9 DVD is treated with superior rectus recession, inferior rectus resection, or inferior oblique anterior transposition. Dissociated horizontal deviation is treated with lateral rectus recession.
Pattern strabismus
The occurrence of A or V pattern strabismus is estimated as 15-25% of all strabismic patients.20 The exact cause is not well understood, but in many patients there is oblique muscle dysfunction and/or an orbital abnormality. Addressing any oblique overaction that exists will help treat the pattern. If there is no oblique dysfunction, shifting the medial rectus muscles at time of recession towards the apex of the pattern will weaken the effective pull of the medial rectus at the apex, decreasing the amount of V or A pattern.
Prognosis
Patients with infantile esotropia frequently have good vision despite reduced binocularity. Earlier surgery is associated with improved binocularity. Treatment of amblyopia, along with multiple surgeries, may be required to achieve the best visual and binocular outcomes.
References
- Costenbader FD. Infantile esotropia. Trans Am Ophthalmol Soc. 1961; 59:397-429.
- Louwagie CR, Diehl NN, Greenberg AE, Mohney BG. Is the incidence of infantile esotropia declining?: a population-based study from Olmstead County, Minnesota, 1965 to 1994. Arch Ophthalmol. 2009; 127(2):200-203.
- Graham PA. Epidemiology of strabismus. Br J Ophthalmol. 1974; 58(3):224-231.
- Birch E, Stager D, Wright K, Beck R. The natural history of infantile esotropia during the first six months of life. Pediatric Eye Disease Investigator Group. J AAPOS. 1998; 2(6):325-328; discussion 329.
- Hiles DA, Watson BA, Biglan AW. Characteristics of infantile esotropia following early bimedial rectus recession. Arch Ophthalmol. 1980; 98(4):697-703.
- Ing MR. Early surgical alignment for congenital esotropia. Trans Am Ophthalmol Soc. 1981; 79:625-663.
- Burian HM, von Noorden GK. Binocular Vision and Ocular Motility. St. Louis: The CV Mosby Company, 1974; 282-289.
- Helveston EM, Neely DF, Stidham DB, Wallace DK, Plager DA, Sprunger DT. Results of early alignment of congenital esotropia. Ophthalmology. 1999; 106(9):1716-1726.
- Buckley EG, Plager DA, Repka MX, Wilson ME. Plager DA, ed. Contributions by Parks MM, von Noorden GK. Ophthalmology Monographs 17. Oxford: Oxford University Press. 2004.
- Holman RE, Merritt JC. Infantile esotropia: results in the neurologic impaired and “normal” child at NCMH (six years). J Pediatr Ophthalmol Strabismus. 1986; 23(1):41-45.
- Gulati S, Andrews CA, Apkarian AO, Musch DC, Lee PP, Stein JD. Effect of gestational age and birth weight on the risk of strabismus among premature infants. JAMA Pediatr. 2014; 168(9):850-856.
- Tychsen L. Can ophthalmologists repair the brain in infantile esotropia? Early surgery, stereopsis, monofixation syndrome, and the legacy of Marshall Parks. J AAPOS. 2005; 9(6):510-521.
- McNeer KW, Spencer RF, Tucker MG. Observations on bilateral simultaneous botulinum toxin injection in infantile esotropia. J Pediatr Ophthalmol Strabismus. 1994; 31(4):214-219.
- Simonsz HJ, Kolling GH, Unnebrink K. Final report of the early vs. late infantile strabismus surgery study (ELISSS), a controlled, prospective, multicenter study. Strabismus. 2005; 13(4):169-199.
- Bradbury JA. What information can we give to the patient about the risks of strabismus surgery. Eye (Lond). 2015; 29(2):252-257.
- Simon JW, Lininger LL, Scheraga JL. Recognized scleral perforation during eye muscle surgery: incidence and sequelae. J Pediatr Ophthalmol Strabismus. 1992; 29(5):273-275.
- Ing MR. Infection following strabismus surgery. Ophthalmic Surg. 1991; 22(1):41-3.
- France TD, Simon JW. Anterior segment ischemia syndrome following muscle surgery: the AAPOS experience. J Pediatr Ophthalmol Strabismus. 1986; 23:87-91.
- Trigler L, Siatkowski RM. Factors associated with horizontal reoperation in infantile esotropia. J AAPOS. 2002; 6(1):15-20.
- Dickmann A, Petroni S, Salerni A, Parrilla R, Savino G, Battendieri R, Perrotta V, Radini C, Balestrazzi E. Effect of vertical transposition of the medial rectus muscle on primary position alignment in infantile esotropia with A- or V-pattern strabismus. J AAPOS. 2011; 15(1):14-16.